Search
- Page Path
- HOME > Search
Review Articles
- Urinary Tract Infection and Urolithiasis: A Narrative Review of Pathophysiological Links and Clinical Implications
- Dong Sup Lee
- Urogenit Tract Infect 2026;21(1):3-10. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2652002001
-
 Abstract
Abstract
 PDF
PDF PubReader
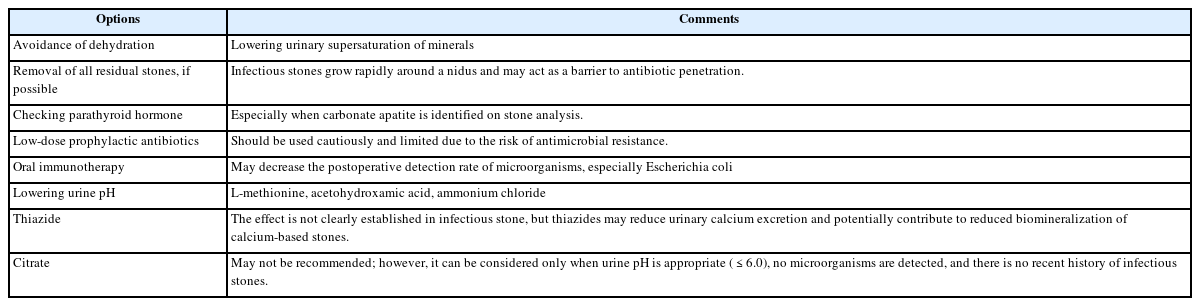
PubReader - Urinary tract infection (UTI) and urolithiasis are closely related clinical entities that frequently coexist and influence each other’s pathogenesis and clinical course. Infection-related stones, particularly struvite and carbonate apatite stones, have long been recognized as consequences of ureaseproducing bacterial infections. However, recent evidence suggests that the role of microorganisms—especially Escherichia coli—in stone disease may extend beyond traditional infection stones; in particular, biofilm formation by microorganisms may contribute to the formation and growth of calcium-based stones. This review summarizes current knowledge on the pathophysiological mechanisms linking UTI and urolithiasis, with a focus on the biochemical processes underlying infection-related stone formation, the characteristics of different stone compositions, and emerging concepts regarding bacterial involvement in metabolic stone disease. A better understanding of the interplay between UTI and urolithiasis may improve preventive strategies, guide antimicrobial and surgical decision-making, and ultimately reduce recurrence rates. This review highlights the need for an integrated clinical approach that considers both infectious and metabolic factors in patients with urinary stone disease.
- 178 View
- 6 Download

- Beyond Empirical Antibiotics: Toward Precision-Based Urinary Tract Infection Management and Korea-Specific Guidelines
- Sang Rak Bae, Hee Jo Yang
- Urogenit Tract Infect 2026;21(1):11-14. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2550048024
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader - Urinary tract infection (UTI) remains one of the most common bacterial infections, yet rising antimicrobial resistance and changing healthcare environments have challenged the traditional empiric approach to antibiotic therapy. Recent international guidelines from the European Association of Urology (EAU), Infectious Diseases Society of America (IDSA), and American Urological Association (AUA) collectively demonstrate a paradigm shift toward precision diagnostics, evidencebased antibiotic selection, standardized nonantibiotic prevention strategies, and simplified disease classification systems. The EAU has emphasized culture-based diagnosis, expanded nonantibiotic prophylaxis, and introduced a new framework distinguishing localized from systemic UTI. The IDSA has strengthened restrictions on treating asymptomatic bacteriuria, provided guidance for managing antimicrobial-resistant organisms, and simplified UTI categories. The AUA similarly highlights culture-directed diagnosis and the minimization of prophylactic antibiotics in women with recurrent UTI while formalizing nonantibiotic preventive measures. In Korea, unique resistance patterns, high extended-spectrum beta-lactamase and fluoroquinolone resistance rates, and frequent movement of patients between long-term care facilities and hospitals underscore the need for Korea-specific UTI guidelines. Although national surveillance systems such as KARMS (Korean Antimicrobial Resistance Monitoring System) and KorGLASS (Global Antimicrobial Resistance Surveillance System in Korea) provide valuable data, the evidence base remains insufficient to match the robustness of international guideline development. Establishing updated, Korean-contextualized UTI guidelines is essential for improving patient safety, optimizing antimicrobial stewardship, and effectively responding to the growing threat of resistance. The field is at a pivotal turning point, requiring proactive leadership and coordinated action within Korea’s urological and infectious disease communities.
- 152 View
- 4 Download

Original Articles
- Identification of Plasma Biomarker Signatures for Acute and Chronic Cystitis Using Olink Explore Proteomics in UK Biobank
- Chang Gu Kang, Su Kang Kim
- Urogenit Tract Infect 2026;21(1):26-39. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2550046023

-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader - Purpose
Acute and chronic cystitis represent common yet biologically distinct inflammatory disorders of the lower urinary tract. However, circulating biomarkers capable of differentiating these conditions remain poorly defined. Materials and Methods: Using COMPASS-processed Olink Explore proteomic data from UK Biobank participants, we compared plasma protein profiles across individuals with acute cystitis, chronic cystitis, and normal controls. After stringent quality-control procedures, covariate-adjusted regression models and differential abundance analyses were performed. STRING-based proteinprotein interaction (PPI) networks were constructed to examine systems-level organization of significantly altered proteins.
Results
Among 2,715 participants, acute and chronic cystitis demonstrated distinct systemic proteomic signatures. CHGA (chromogranin A) and GAST (gastrin) were consistently elevated across both phenotypes, indicating shared neuroendocrine-associated systemic responses. Acute cystitis showed selective elevation of CDH2 (cadherin-2), whereas chronic cystitis demonstrated marked increases in GDF15 (growth differentiation factor 15). PPI network analysis revealed a densely interconnected architecture in acute cystitis and a more modular, branch topology in chronic cystitis, reflecting differing organizational patterns of circulating proteins.
Conclusions
This population-level analysis identifies phenotype-specific and shared plasma protein signatures associated with acute and chronic cystitis and provides an initial framework for understanding systemic inflammatory profiles in these conditions. Interpretation should remain cautious given the cross-sectional design, reliance on historical diagnostic classification, and the absence of bladder-specific molecular data. Nonetheless, these findings highlight candidate biomarkers that merit further validation in longitudinal and mechanistic studies.
- 181 View
- 4 Download

- The Korean Antimicrobial Resistance Monitoring System for Complicated Urinary Tract Infections: A Prospective Multicenter Observational Study Conducted by the Korean Association of Urogenital Tract Infection and Inflammation
- Seong Hyeon Yu, Seung Il Jung, Donghoon Lim, Jeong Woo Lee, Seung-Ju Lee, Hong Chung, Mi-Mi Oh, Jing Bong Choi, Jae Hung Jung, Hee Jo Yang, KAUTII Investigators
- Urogenit Tract Infect 2026;21(1):15-25. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2550040020
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader - Purpose
This study aimed to report antimicrobial resistance (AMR) patterns among patients with complicated urinary tract infection (cUTI) using data from the Korean Antimicrobial Resistance Monitoring System (KARMS). Materials and Methods: In this prospective, multicenter, observational surveillance study, data from patients diagnosed with cUTI between January 2023 and September 2025 were retrieved from the KARMS database. Demographic characteristics, uropathogen distribution, and antimicrobial susceptibility profiles of representative pathogens were analyzed.
Results
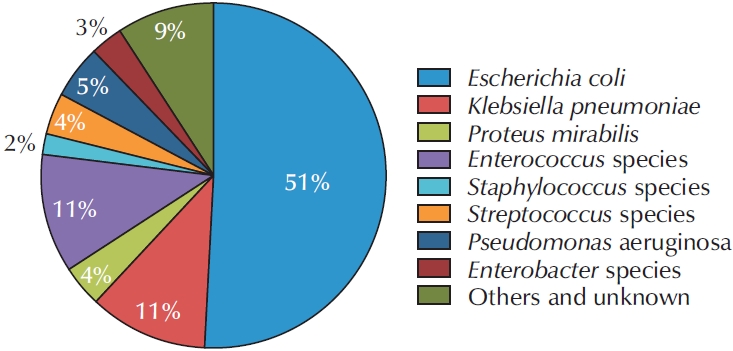
Data from a total of 698 patients were collected in the KARMS database. The mean patient age was 68.94±15.95 years. The numbers of patients with healthcare-associated UTI and recurrent UTI were 171 (24.5%) and 240 (34.4%), respectively. Escherichia coli was the most frequently identified uropathogen (n=356, 51.1%). Regarding antimicrobial susceptibility, 92.9% of isolates were susceptible to fosfomycin, 75.5% to nitrofurantoin, 47.2% to ciprofloxacin, 63.3% to cefotaxime, 80.6% to piperacillin/tazobactam, and 98.8% to ertapenem. The rate of extended-spectrum beta-lactamase positivity was 45.2% (166 of 367) and was significantly higher in pyelonephritis and urosepsis (62.3% and 62.5%, p=0.002), healthcare-associated UTI (58.6%, p=0.040), and recurrent cUTI (53.2%, p=0.028). Fluoroquinolone resistance was significantly more common in female patients (49.1%, p=0.021) and in healthcare-associated UTI (57.9%, p=0.014). Piperacillin/tazobactam resistance was significantly higher in patients with urosepsis (37.0%, p=0.004), in tertiary hospitals (17.2%, p=0.019), and in healthcare-associated UTI (26.4%, p=0.001). In addition, third-generation cephalosporin resistance was significantly higher in secondary hospitals than in tertiary hospitals (43.5% vs. 33.3%, p=0.041).
Conclusions
These data provide current information on uropathogen distribution and AMR patterns in cUTI in South Korea. Continued surveillance and ongoing data accumulation through KARMS will support evidence-based strategies for optimal antimicrobial therapy and AMR mitigation.
- 162 View
- 9 Download

Case Report
- Bilateral Xanthogranulomatous Pyelonephritis With Extensive Abscess Associated With Neurogenic Bladder: A Case Report
- Sin Woo Lee, Hee Seung Choi
- Urogenit Tract Infect 2026;21(1):40-43. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2550026013
-
 Abstract
Abstract
 PDF
PDF PubReader
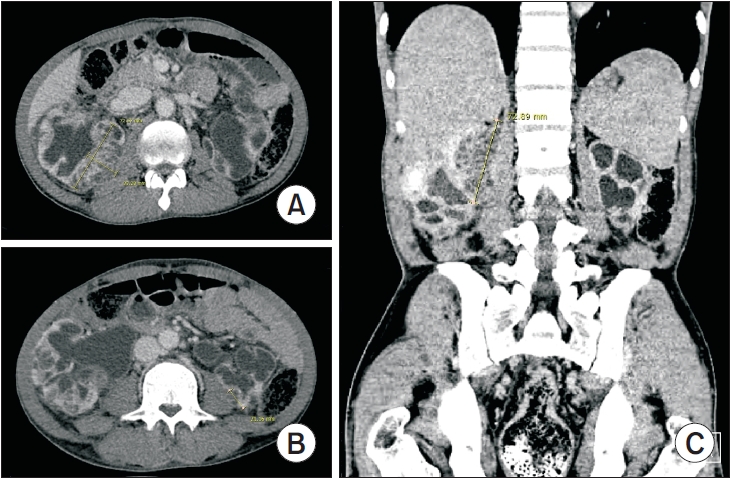
PubReader - Xanthogranulomatous pyelonephritis (XGP) is a rare and severe form of chronic pyelonephritis. We report a case of bilateral XGP complicated by extensive abscess formation. A 47-year-old man presented with fatigue and generalized weakness. Laboratory evaluation revealed leukocytosis and elevated serum creatinine levels. Urinalysis demonstrated pyuria and bacteriuria. Computed tomography (CT) revealed bilaterally enlarged kidneys with multifocal renal parenchymal and perirenal abscesses. The CT scan also demonstrated severe bilateral hydronephroureter and diffuse bladder wall thickening, with a radiologic impression of severe pyelonephritis with abscess formation and neurogenic bladder. The patient was admitted and treated with intravenous antibiotics and percutaneous nephrostomy tube placement. However, no clinical improvement was observed with conservative management. The patient subsequently underwent right open radical nephrectomy. Histopathological examination confirmed the diagnosis of XGP with extensive abscess formation. The patient experienced no further complications or recurrence after surgery. This case suggests that chronic untreated neurogenic bladder may contribute to the development of severe chronic pyelonephritis such as XGP.
- 134 View
- 4 Download

Review Article
- Adult Syphilis: A Narrative Review of Clinical Insights and Public Health Implications in Urology
- Seung-Ju Lee, Jin Bong Choi
- Urogenit Tract Infect 2025;20(3):123-131. Published online December 31, 2025
- DOI: https://doi.org/10.14777/uti.2550039017
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
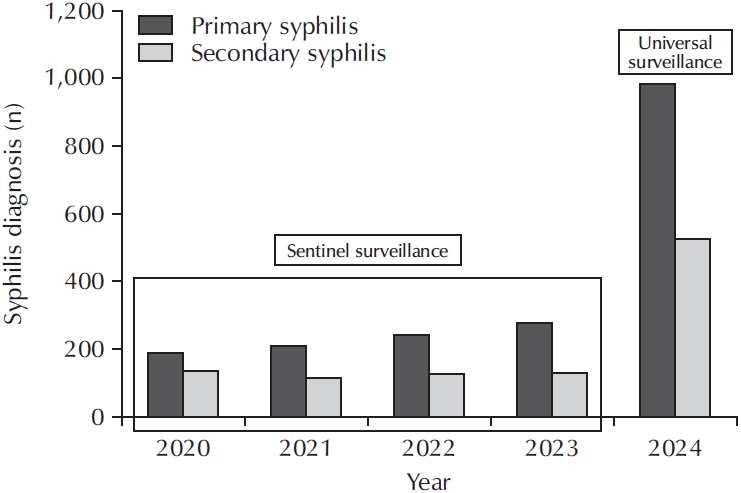
ePub - Syphilis continues to pose a major global public health concern, with more than 7 million cases reported worldwide in 2022, and its incidence continues to rise in numerous regions. In Korea, the shift from sentinel to universal notification in 2024 has revealed a markedly greater disease burden, particularly among men who have sex with men and among younger adults, underscoring changing epidemiological patterns and the urgent need for revised control strategies. In urological practice, syphilis presents with a wide range of often misleading symptoms, including painless genital ulcers, urethritis, and sexual dysfunction, that frequently resemble other genitourinary disorders and complicate diagnostic evaluation. Accurate identification relies on integrating a thorough clinical assessment with serologic testing while remaining alert to diagnostic challenges such as early latent infection, serofast states, and human immunodeficiency virus coinfection. Penicillin G remains the mainstay of therapy, with treatment regimens tailored to the stage of disease and to the presence or absence of central nervous system involvement. Effective partner notification, targeted screening, and consistent follow-up are essential to prevent reinfection and limit further transmission. At a public health level, a multifaceted strategy—strengthened surveillance systems, focused testing in high-risk populations, and embedding syphilis screening within broader sexually transmitted infection care frameworks—is critical to curbing its resurgence. In summary, prompt recognition, adherence to evidence-based management, and coordinated public health measures, together with ongoing advances in diagnostics and prevention, remain fundamental to reducing the continued spread of syphilis and mitigating its impact on both individual and population health.
- 1,324 View
- 19 Download

Case Report
- Primary Bladder and Ureteral Amyloidosis Initially Diagnosed as Chronic Cystitis: A Case Report
- Seungsoo Lee, Dan Bee Lee, Hyun Jung Lee, Won Hoon Song, Sung-Woo Park, Jong Kil Nam
- Urogenit Tract Infect 2025;20(3):167-172. Published online December 31, 2025
- DOI: https://doi.org/10.14777/uti.2550038019
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
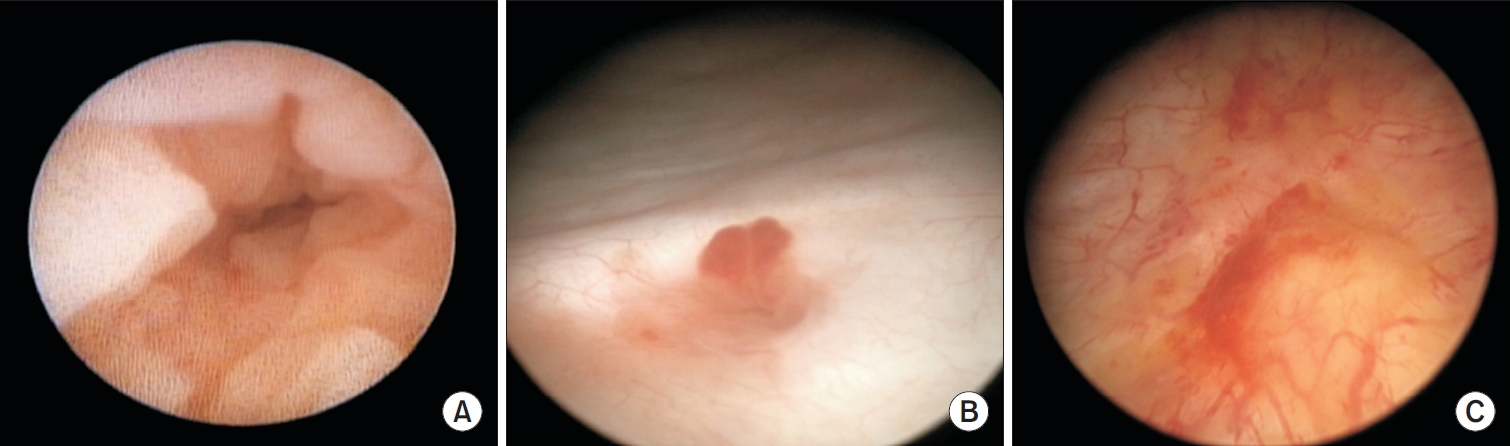
ePub - Primary localized amyloidosis confined to the urinary tract is uncommon and frequently misinterpreted due to clinical and radiologic overlap with more prevalent conditions. We describe a 69-year-old woman who experienced recurrent gross hematuria over 2 years and underwent initial transurethral resection based on a presumptive diagnosis of chronic cystitis. Subsequent evaluation revealed a left ureteral mass with hydronephrosis, raising concern for malignancy. Histopathologic examination of both bladder and ureteral specimens demonstrated amorphous eosinophilic deposits that stained positive with Congo red and showed apple-green birefringence under polarized microscopy. Immunofluorescence confirmed λ-light-chain predominance, establishing AL (amyloid light chain)-type amyloidosis without systemic involvement. The patient underwent complete endoscopic resection and remains asymptomatic during ongoing surveillance. This case highlights the diagnostic challenges posed by localized urinary amyloidosis and underscores the importance of histologic confirmation in atypical inflammatory lesions.
- 1,187 View
- 9 Download

Original Article
- Clinical Characteristics and Risk Factors of Fournier Gangrene: A 15-Years Multicenter Retrospective Study in Korea
- Seung-Kwon Choi, Sin Woo Lee, Hyung-Lae Lee, Jeong Woo Lee, Jung Sik Huh, Yeonjoo Kim, Sangrak Bae, Tae-Hyoung Kim
- Urogenit Tract Infect 2025;20(3):159-166. Published online December 31, 2025
- DOI: https://doi.org/10.14777/uti.2550036018
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader ePub
ePub - Purpose
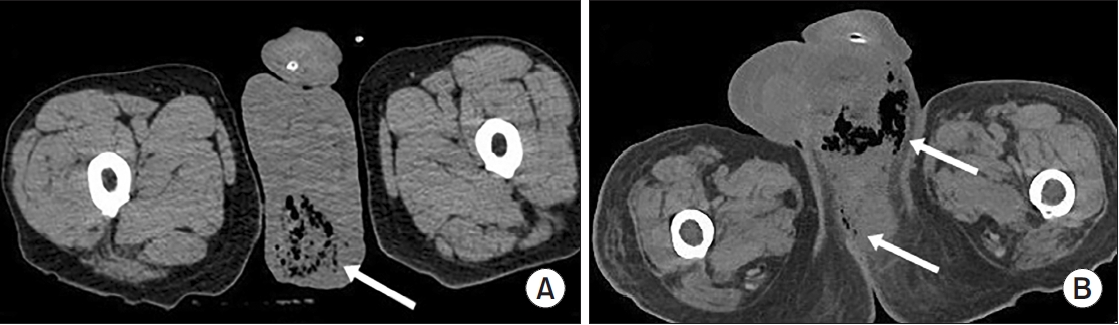
Fournier gangrene (FG) is a rare but life-threatening necrotizing infection requiring prompt recognition and intervention. This multicenter study aimed to investigate the clinical characteristics, treatment outcomes including mortality, and risk factors associated with death among patients with FG over the past 15 years in Korea. Materials and Methods: We retrospectively reviewed 84 patients diagnosed with FG between 2008 and 2022 across 7 hospitals. Demographics, comorbidities, laboratory findings, and clinical outcomes were analyzed. Mortality-related risk factors were assessed using univariate and multivariate logistic regression analysis.
Results
The mean age was 58.1±15.9 years, and 95.2% of patients were male. Diabetes mellitus (42.9%) and hypertension (36.9%) were the most prevalent comorbidities. Sepsis developed in 38.1% of patients, and the overall mortality rate was 14.3%. In univariate analysis, age ≥70 years, low body mass index, diabetes mellitus, low hemoglobin, low hematocrit, high respiratory rate, and Fournier gangrene severity index (FGSI) ≥9 were significantly associated with mortality. After data correction and multivariate adjustment, diabetes mellitus (odds ratio [OR], 39.61; 95% confidence interval [CI], 2.39–656.32; p=0.010) and respiratory rate (OR, 1.44; 95% CI, 1.09–1.91; p=0.011) were identified as independent predictors of mortality. FGSI≥9 demonstrated borderline association with mortality (p=0.08), indicating its potential clinical relevance.
Conclusions
In this multicenter Korean cohort, the mortality rate of FG remained substantial at 14.3%. Diabetes mellitus and elevated respiratory rate were independent predictors of mortality, while FGSI≥9 demonstrated a borderline yet clinically meaningful association, suggesting its role as a useful severity indicator in early risk stratification. -
Citations
Citations to this article as recorded by- A Commentary on “Clinical Characteristics and Risk Factors of Fournier Gangrene: A 15-Years Multicenter Retrospective Study in Korea”
Jae Yoon Kim
Urogenital Tract Infection.2026; 21(1): 44. CrossRef
- A Commentary on “Clinical Characteristics and Risk Factors of Fournier Gangrene: A 15-Years Multicenter Retrospective Study in Korea”
- 1,191 View
- 23 Download
- 1 Crossref

Review Articles
- Beyond the Number: Interpreting Prostate-Specific Antigen Elevation in the Context of Prostate Inflammation
- Byoungkyu Han, Ki-Hyuck Moon
- Urogenit Tract Infect 2025;20(3):132-143. Published online December 31, 2025
- DOI: https://doi.org/10.14777/uti.2550032016
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader ePub
ePub - Prostate-specific antigen (PSA) is indispensable but not cancer specific; inflammation, benign prostatic hyperplasia, urinary retention, ejaculation, and instrumentation can all elevate PSA and complicate cancer risk assessment. This review synthesizes current evidence and guidelines to support clinicians in interpreting PSA elevations when inflammation is present or suspected. Acute febrile urinary tract infection and acute bacterial prostatitis may produce very high PSA values, sometimes exceeding 100 ng/mL, and normalization can be slow; therefore, PSA testing during active infection is discouraged. When PSA is only mildly to moderately elevated, standardized repeat testing is essential because a meaningful proportion of results normalize on retesting. A magnetic resonance imaging (MRI)-first pathway improves detection of clinically significant prostate cancer while reducing overdiagnosis and enables biopsy deferral after a negative MRI under structured monitoring. PSA density (PSAD) further refines triage alongside MRI, with practical working thresholds of roughly 0.10–0.20 ng/mL/cm3 calibrated to MRI quality and pretest risk. However, asymptomatic histologic prostatitis (National Institutes of Health category IV) is common and may raise PSA without reliably altering PSAD, which means that PSAD alone cannot confirm that an elevation is attributable solely to inflammation. Validated secondary biomarkers (e.g., Prostate Health Index, 4Kscore, IsoPSA [isoform PSA], Stockholm3, Proclarix, PCA3 [prostate cancer gene 3], SelectMDx [select molecular diagnostics], ExoDx [exosome diagnostics], MPS/MPS2 [MyProstateScore/MyProstateScore 2.0]) are best used selectively when MRI is negative or equivocal and clinical risk remains uncertain. A pragmatic sequence—confirm, image, and refine—helps minimize missed clinically significant cancer while reducing unnecessary antibiotics and biopsies when inflammation is the predominant driver of PSA elevation.
-
Citations
Citations to this article as recorded by- An Unusual Presentation of a Complicated Urinary Tract Infection With Features Concerning for Malignancy: A Diagnostic Challenge
Drew K Knight, Tailla Santos, Amber J Stout, Adrian Martinez Crespo, Ilya Fonarov
Cureus.2026;[Epub] CrossRef
- An Unusual Presentation of a Complicated Urinary Tract Infection With Features Concerning for Malignancy: A Diagnostic Challenge
- 2,807 View
- 35 Download
- 1 Crossref

- Regenerative Medicine for the Kidney
- Vladimir Mashanov, Ji Hyun Kim
- Urogenit Tract Infect 2025;20(3):144-158. Published online December 31, 2025
- DOI: https://doi.org/10.14777/uti.2550028014
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
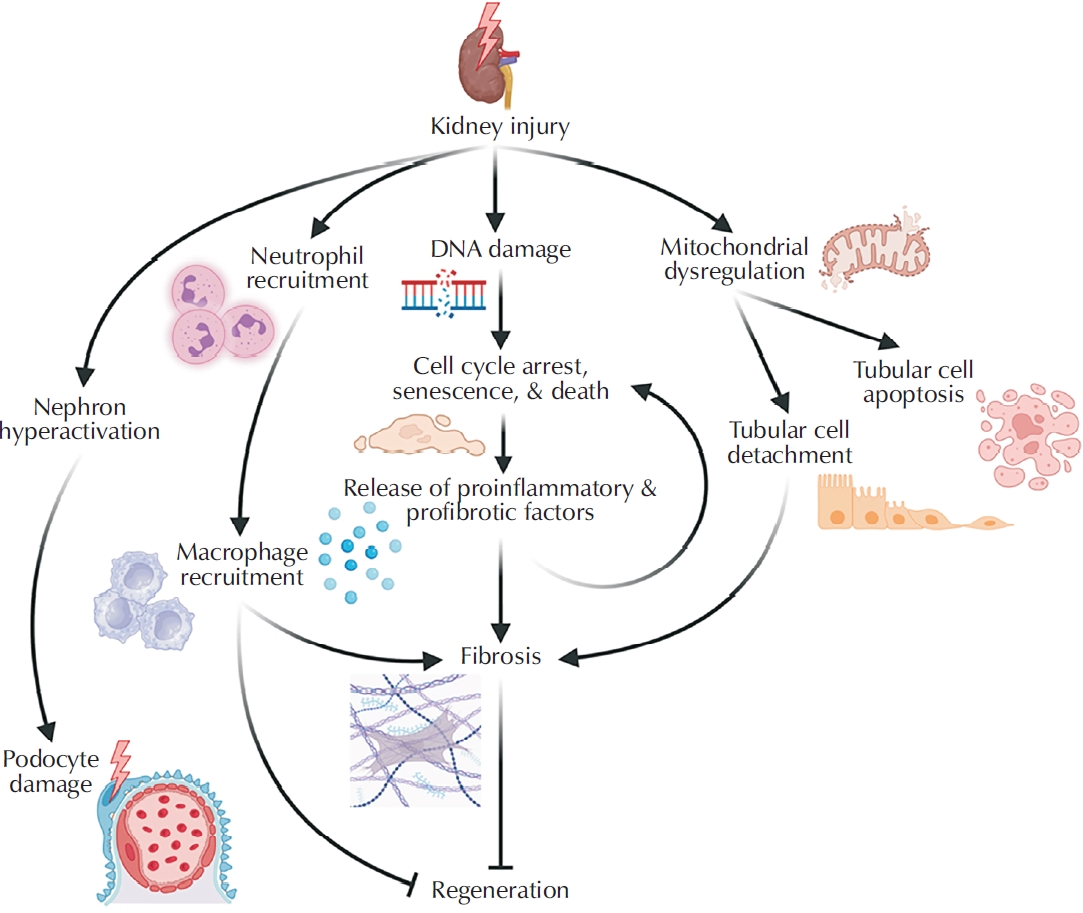
ePub - Kidney disease poses a major and growing global health challenge, with both prevalence and mortality continuing to rise. Current standard-of-care treatments, including dialysis and kidney transplantation, have significant limitations and do not adequately meet clinical needs. This unmet need has driven the development of next-generation regenerative medicine strategies, which can be broadly categorized into 3 areas: (1) approaches that enhance the kidney’s limited intrinsic regenerative capacity; (2) stem cell-based therapies; and (3) implantable bioengineered kidney constructs. This review summarizes recent advances in each of these domains and discusses the major biological, technical, and regulatory challenges that must be addressed to enable successful clinical translation.
- 1,606 View
- 18 Download

Case Report
- Cyclic Hematuria Misdiagnosed as Hemorrhagic Cystitis in a Rare Case of Vesicouterine Fistula Post-Cesarean Section: A Case Report of Youssef Syndrome
- Youngjoo Kim
- Urogenit Tract Infect 2025;20(2):114-117. Published online August 31, 2025
- DOI: https://doi.org/10.14777/uti.2550024012
-
 Abstract
Abstract
 PDF
PDF PubReader
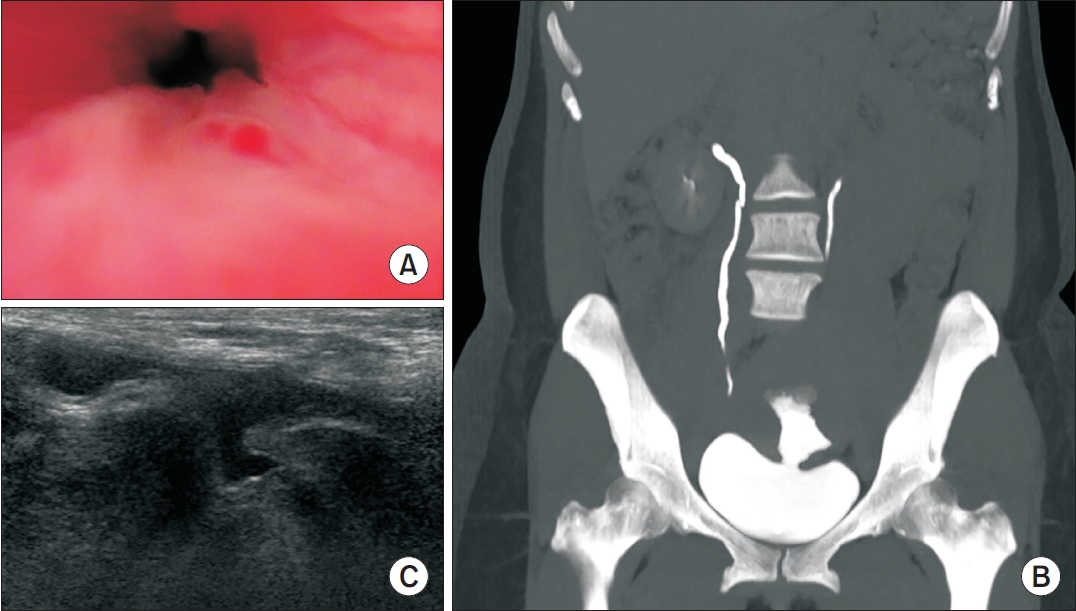
PubReader - Vesicouterine fistulas are rare complications that may occur following cesarean sections and are frequently misdiagnosed due to their diverse clinical presentations. This report presents a case involving a small vesicouterine fistula initially managed conservatively, which later manifested as cyclic hematuria mimicking hemorrhagic cystitis, ultimately leading to a diagnosis of Youssef syndrome. A 45-year-old woman developed persistent vaginal urinary leakage 3 weeks after a cesarean section. Diagnostic evaluation confirmed a small (<1 cm) vesicouterine fistula. Conservative management with Foley catheterization resulted in spontaneous closure. Four months later, the patient experienced cyclic gross hematuria and dysuria without menstruation, and was subsequently diagnosed with Youssef syndrome. Hormonal therapy using continuous oral contraceptives successfully resolved the hematuria, providing a noninvasive therapeutic option. This case highlights the importance of considering Youssef syndrome in patients with cyclic hematuria after cesarean section, in order to distinguish it from hemorrhagic cystitis and ensure timely, appropriate management.
-
Citations
Citations to this article as recorded by- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(2): 55. CrossRef
- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 1,758 View
- 13 Download
- 1 Crossref

Original Article
- Diagnostic Utility of the Sysmex UF-5000 Flow Cytometer in Acute Bacterial Prostatitis: A Retrospective Pilot Study
- Young Kyu Han, Jeong Woo Lee, Hae-Il Park, Jin Bong Choi
- Urogenit Tract Infect 2025;20(2):107-113. Published online August 31, 2025
- DOI: https://doi.org/10.14777/uti.2550022011
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader - Purpose
To evaluate the diagnostic performance of the Sysmex UF-5000 flow cytometer in detecting acute bacterial prostatitis (ABP) compared to standard urine culture. Materials and Methods: This retrospective study analyzed 45 urine samples from patients with a clinical diagnosis of ABP. Each sample was evaluated using the UF-5000 to measure red blood cells (RBC), white blood cells (WBC), and bacterial counts, and the results were compared with those from standard urine culture and Gram staining. Receiver operating characteristic curves were generated, and sensitivity, specificity, positive predictive value (PPV), and negative predictive value were determined. Concordance between Gram classification by the UF-5000 and conventional Gram staining was also evaluated.
Results
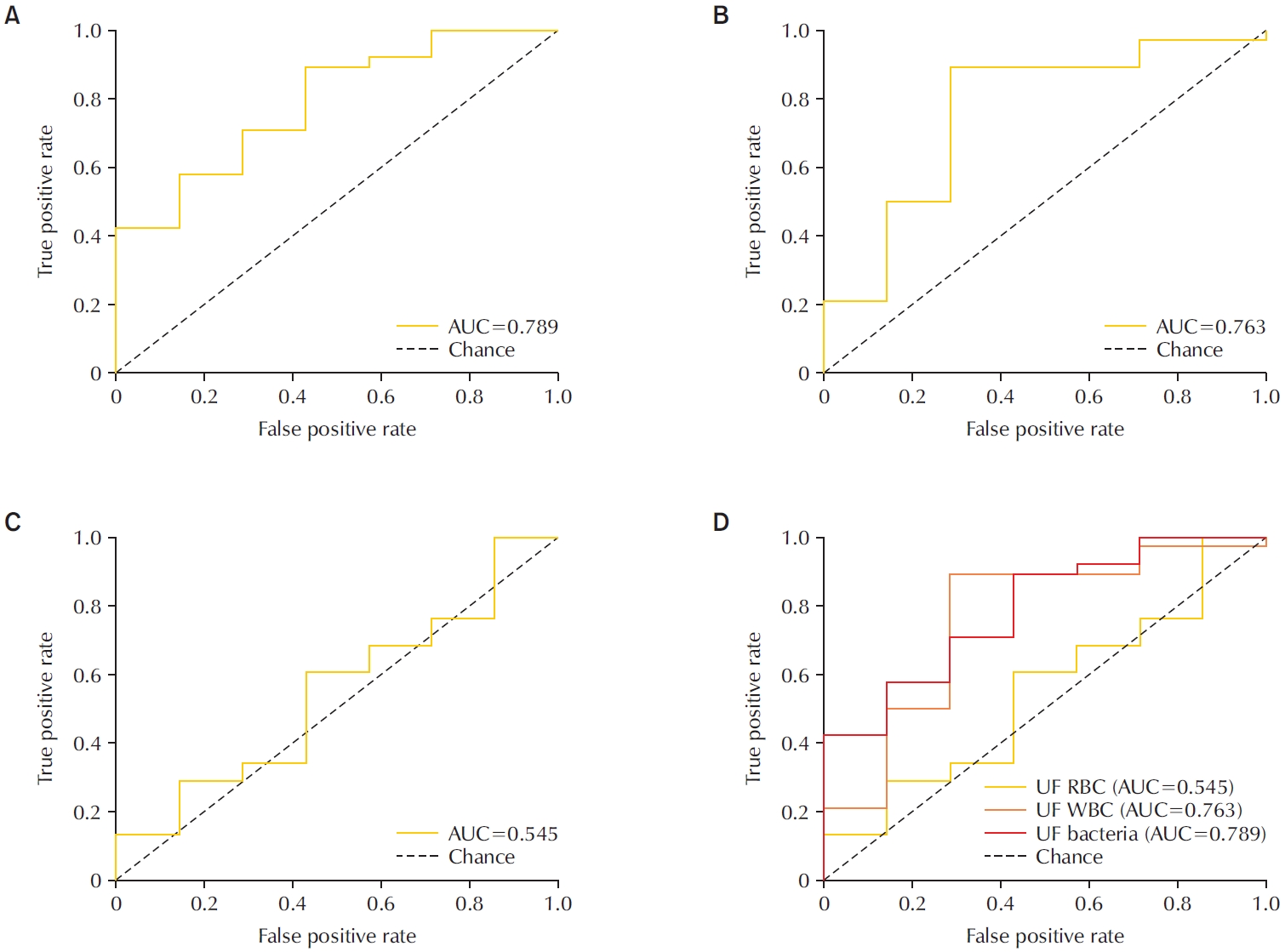
Of the 45 patients, 84.4% had positive urine cultures. The bacterial count parameter demonstrated the highest diagnostic performance (area under the curve [AUC]=0.79; sensitivity, 89.5%; PPV, 91.9%), outperforming WBC (AUC=0.76) and RBC (AUC=0.55). The Gram classification flag showed an overall concordance of 85.7% with conventional Gram staining, with a concordance rate of 88% for Gram-negative organisms.
Conclusions
The Sysmex UF-5000 exhibited good concordance with urine culture for patients with ABP, particularly through the bacterial count parameter. Although it does not replace culture, the UF-5000 may serve as a rapid adjunctive tool to support early clinical decision-making in suspected ABP cases. -
Citations
Citations to this article as recorded by- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(2): 55. CrossRef - A Commentary on “Diagnostic Utility of the Sysmex UF-5000 Flow Cytometer in Acute Bacterial Prostatitis: A Retrospective Pilot Study”
Dong-Hoon Lim
Urogenital Tract Infection.2025; 20(3): 173. CrossRef
- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 2,228 View
- 40 Download
- 2 Crossref

Review Articles
- Molecular Mechanisms of Antibiotic Resistance in Uropathogenic Escherichia coli: A Narrative Review
- Nakjun Choi, Dong Uk Kim, Eun-Jin Lee
- Urogenit Tract Infect 2025;20(2):96-106. Published online August 31, 2025
- DOI: https://doi.org/10.14777/uti.2550018009
-
 Abstract
Abstract
 PDF
PDF PubReader
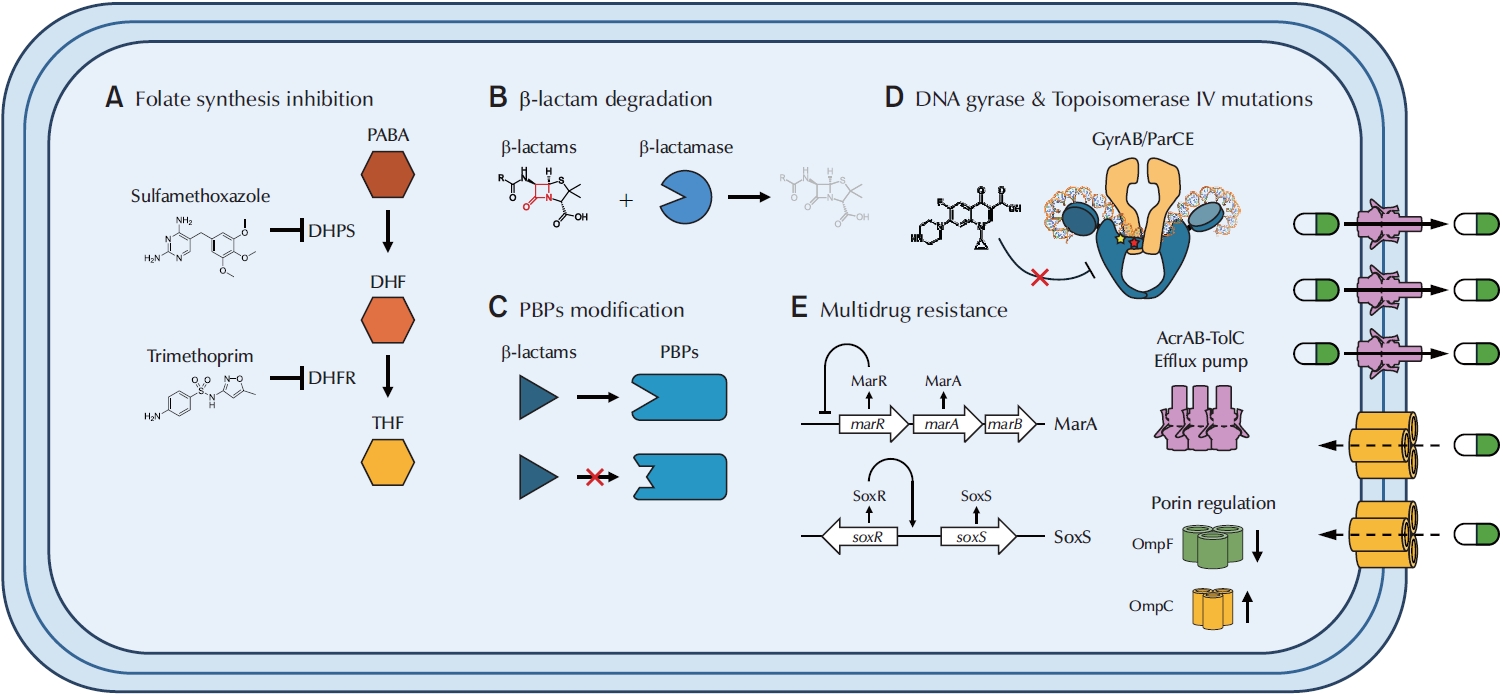
PubReader - Urinary tract infections (UTIs) are among the most prevalent bacterial infections worldwide, with uropathogenic Escherichia coli (UPEC) serving as the primary causative agent. Although antibiotic therapy remains the standard of care for UTI treatment, the increasing prevalence of antimicrobial resistance has substantially reduced the effectiveness of commonly prescribed antibiotics. Resistance to trimethoprim-sulfamethoxazole (TMP-SMX), β-lactams, and fluoroquinolones is particularly concerning, as these agents constitute the principal therapeutic options for UTIs. This review examines the molecular mechanisms underlying UPEC resistance to these three classes of antibiotics, including target site modifications, efflux pump overexpression, porin regulation, and enzymatic degradation. Furthermore, it explores how these resistance determinants contribute to the development of multidrug-resistant (MDR) UPEC strains, which demonstrate cross-resistance to multiple antibiotics and present significant challenges for clinical management. Novel therapeutic strategies, such as efflux pump inhibitors, bacteriophage therapy, and genomic-guided precision medicine, are under investigation as potential solutions to address the growing global burden of MDR UPEC, alongside alternative non-antibiotic treatments. This review aims to provide a comprehensive overview of the genetic and regulatory pathways driving antibiotic resistance in UPEC, offering insights that may guide the development of effective treatment strategies and help mitigate the ongoing spread of antimicrobial resistance.
-
Citations
Citations to this article as recorded by- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(2): 55. CrossRef
- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 7,912 View
- 157 Download
- 1 Crossref

- The Role of the Urinary Microbiome in the Prevention of Pediatric Urinary Tract Infections: A Narrative Review
- Byeongdo Song
- Urogenit Tract Infect 2025;20(2):82-95. Published online August 31, 2025
- DOI: https://doi.org/10.14777/uti.2550016008
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader - Urinary tract infections (UTIs) are a common condition in children and often lead to hospitalization. A considerable proportion of children with UTIs (up to 30%) experience at least one recurrence, placing them at risk for long-term complications such as renal scarring. Since the concept of the microbiome was first introduced in 2001, increasing attention has been given to the role of the urinary tract microbiome in maintaining urinary tract homeostasis. Dysbiosis of the urinary microbiome has been recognized as a factor associated with an increased risk of various urinary tract diseases, including UTIs. However, the specific role of the urinary microbiome in the pathophysiology of pediatric UTIs remains incompletely understood. The present review examines recent studies on the urinary microbiome in children and summarizes current strategies for modulating the urinary microbiome to prevent UTI recurrence in the pediatric population.
-
Citations
Citations to this article as recorded by- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(2): 55. CrossRef
- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 5,267 View
- 65 Download
- 1 Crossref

- Beta-Lactamase-Mediated Antibiotic Resistance in Urinary Tract Infections: Mechanisms and Therapeutic Strategies
- Fanglin Shao, Dengxiong Li, Jie Wang, Zhouting Tuo, Zhipeng Wang, Wuran Wei, Ruicheng Wu, Dechao Feng
- Urogenit Tract Infect 2025;20(2):67-81. Published online August 31, 2025
- DOI: https://doi.org/10.14777/uti.2550012006
-
 Abstract
Abstract
 PDF
PDF PubReader
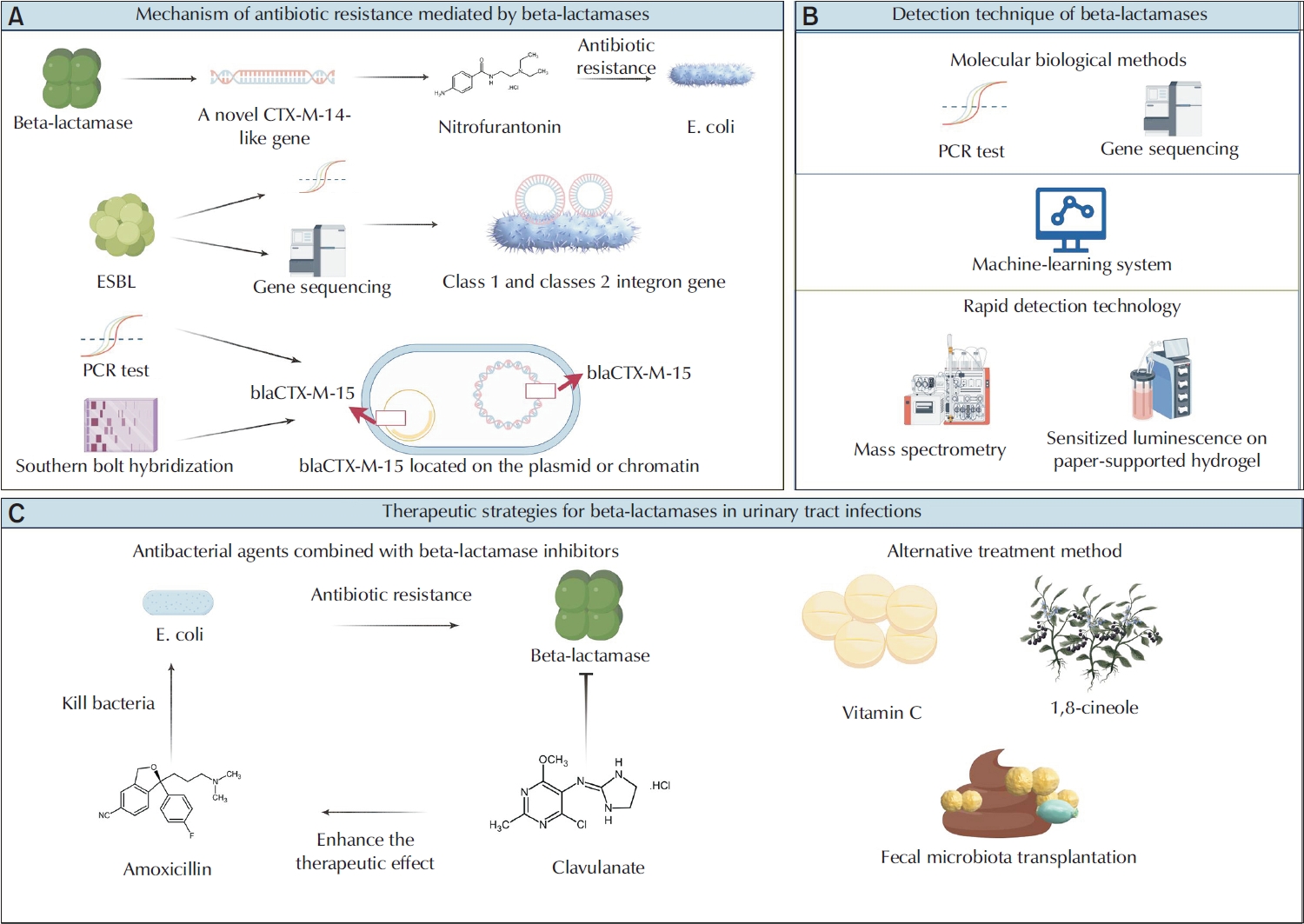
PubReader - Urinary tract infections (UTIs) are among the most prevalent bacterial infections globally, and are primarily caused by Escherichia and Klebsiella. The overprescription and inappropriate use of antibiotics have accelerated the emergence of multidrug-resistant bacteria. Beta-lactamases play a critical role in mediating antibiotic resistance in UTIs. These enzymes promote bacterial resistance through multiple mechanisms, including gene mutation, plasmid-mediated horizontal gene transfer, and the involvement of integrons. Comprehensive knowledge of the ways in which beta-lactamases contribute to resistance in UTIs is essential for improving treatment strategies. Advances in detection technologies, such as gene sequencing and mass spectrometry, have greatly enhanced the ability to monitor and predict bacterial resistance. Current therapeutic strategies include the application of beta-lactamase inhibitors, the development of novel antibiotics, and alternative treatments that have shown efficacy against beta-lactamase-mediated antibiotic resistance. This paper reviews the mechanisms of beta-lactamase-mediated resistance in UTIs and provides an in-depth overview of several detection methods and therapeutic approaches.
-
Citations
Citations to this article as recorded by- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(2): 55. CrossRef
- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 8,809 View
- 98 Download
- 1 Crossref

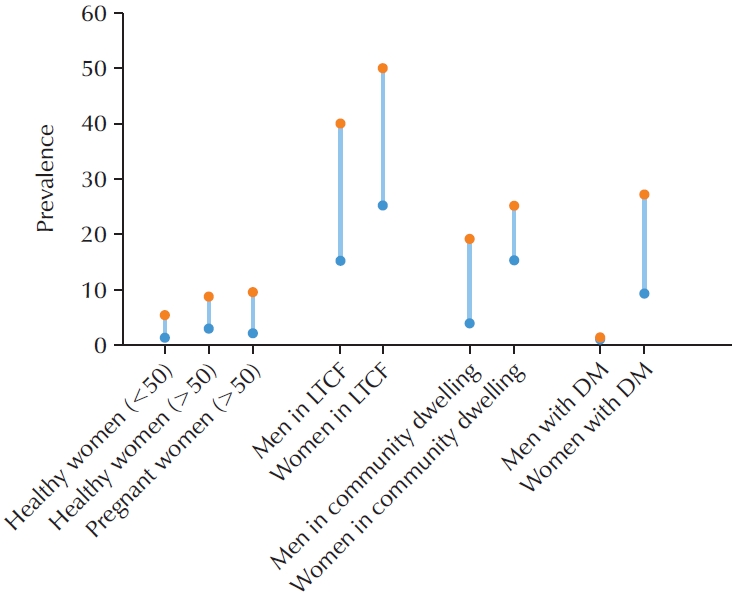
- Asymptomatic Bacteriuria in Older Adults – Diagnosis, Management, and Future Directions: A Narrative Review
- Ki Hong Kim, Hee Jo Yang
- Urogenit Tract Infect 2025;20(2):58-66. Published online August 31, 2025
- DOI: https://doi.org/10.14777/uti.2550002001
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader - Asymptomatic bacteriuria (ASB) is defined as the presence of bacteria in the urine in the absence of urinary tract infection (UTI) symptoms. The prevalence of ASB increases with advancing age, particularly among older patients with underlying health conditions. ASB is especially common among residents of long-term care facilities; however, distinguishing ASB from symptomatic UTI in this population remains a significant clinical challenge. The frequent occurrence of ASB often results in unnecessary antibiotic administration, thereby contributing to the development of antibiotic resistance. Current clinical guidelines recommend screening for and treating ASB only in certain circumstances, such as prior to urological procedures or in pregnant women. There is a pressing need for improved diagnostic approaches to differentiate ASB more accurately from UTI, particularly in older adults. Reducing unnecessary urine testing and inappropriate antibiotic use may help prevent over-treatment and minimize associated risks, including Clostridium difficile infection and increased antimicrobial resistance.
-
Citations
Citations to this article as recorded by- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(2): 55. CrossRef
- Editorial for Urogenital Tract Infection (UTI) 2025 Vol. 20 No. 2 – Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 16,779 View
- 214 Download
- 1 Crossref

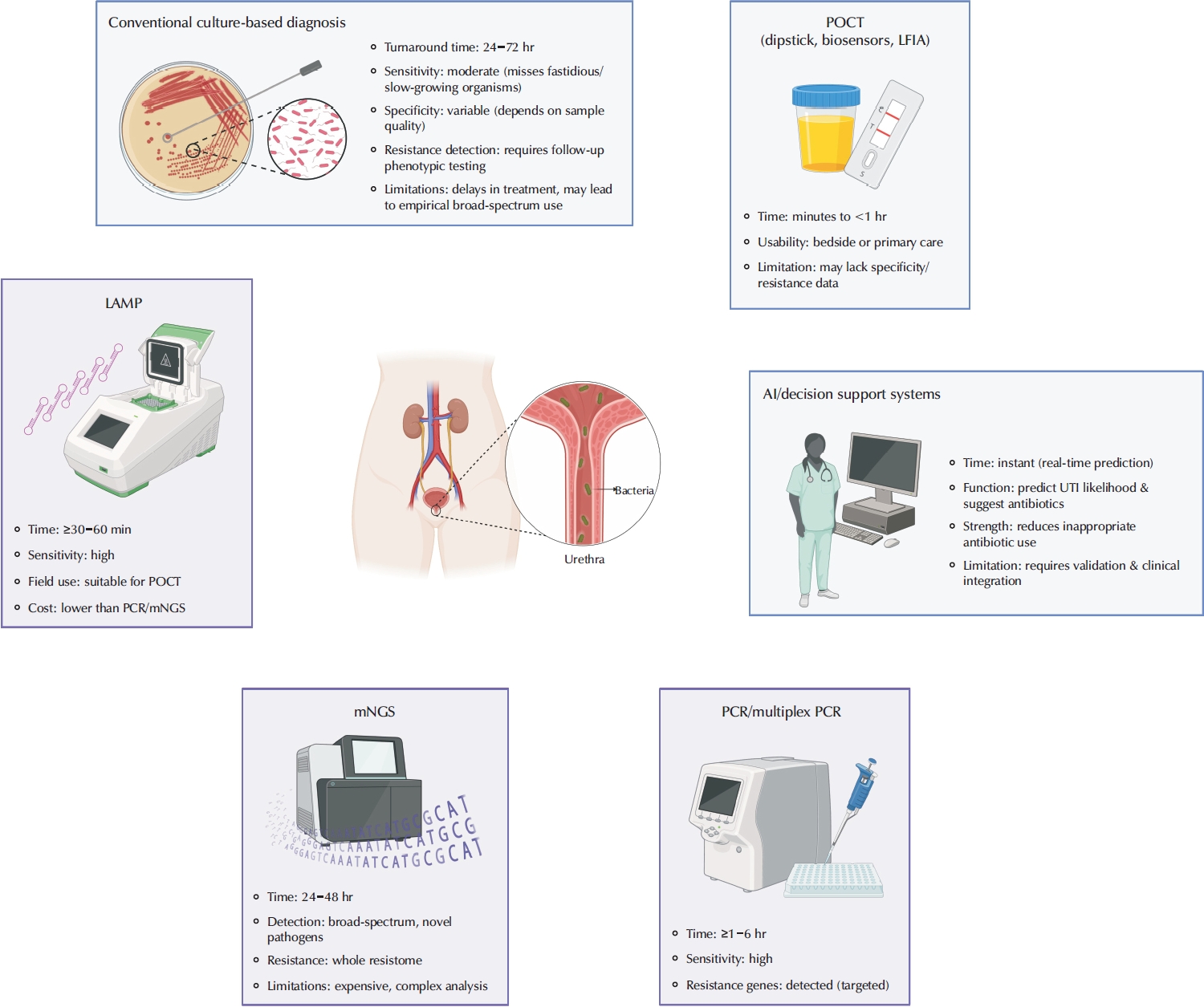
- Advances in the Diagnosis of Urinary Tract Infection: A Narrative Review
- Juan Victor Ariel Franco, Nicolás Meza
- Urogenit Tract Infect 2025;20(1):17-27. Published online April 30, 2025
- DOI: https://doi.org/10.14777/uti.2550020010
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Urinary tract infections are among the most frequent bacterial infections, significantly impacting patient morbidity and healthcare resources. Prompt and accurate diagnosis is crucial to ensure effective treatment, prevent complications such as pyelonephritis or sepsis, and reduce inappropriate antibiotic use, contributing to antimicrobial resistance (AMR). Despite consensus across international guidelines from organizations, challenges persist, particularly in distinguishing true infections from asymptomatic bacteriuria or nonspecific symptoms, especially in older adults. Recent advancements in diagnostic technology have emerged to address these limitations, including molecular diagnostics, point-of-care testing (POCT), and artificial intelligence (AI)-driven predictive models. Molecular techniques, notably polymerase chain reaction, loop-mediated isothermal amplification, and metagenomic next-generation sequencing, offer enhanced sensitivity and specificity, rapid detection times, and comprehensive identification of pathogens and resistance profiles. POCT innovations, such as lateral flow immunoassays, enzymatic-based rapid tests, and novel biosensors, facilitate prompt bedside diagnosis, although specificity challenges remain. Meanwhile, AI and machine learning models demonstrate significant potential for risk stratification, prediction of infection, and improving antibiotics prescription practices yet face barriers related to validation, practical integration, and clinical acceptability. Despite promising developments, significant gaps remain, including limited real-world implementation evidence, high costs, and insufficient data from diverse populations. Further rigorous clinical studies, economic evaluations, and practical implementation assessments are urgently required. Addressing these research gaps could substantially improve patient outcomes, optimize antibiotic stewardship, and reduce the global burden of AMR.
-
Citations
Citations to this article as recorded by- Diagnosis of urinary tract infections in the pediatric population – current practices, advances and progress
Maria Bitsori, Roza-Ioanna Poulaki, Emmanouil Galanakis
Expert Review of Anti-infective Therapy.2026; 24(1): 139. CrossRef - An update on Escalating Drug Resistance among Uropathogenic Bacteria: Challenges in Treatment and Scope for Maneuver
Mohd Asim, Syed Ahmed Rizvi, Vikar Ahmed, Qazi Mohd Rizwanul Haq
Current Microbiology.2026;[Epub] CrossRef - Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(1): 1. CrossRef
- Diagnosis of urinary tract infections in the pediatric population – current practices, advances and progress
- 12,407 View
- 381 Download
- 3 Crossref

Original Article
- Efficacy of Urovaxom for Improving Chronic Pelvic Pain Syndrome Symptoms in Prostate Cancer Patients Who Underwent Radical Prostatectomy: A Multicenter, Prospective Cohort Study
- Jun-Koo Kang, Yun-Sok Ha, Sungchan Park, Tae Gyun Kwon, Tae-Hwan Kim
- Urogenit Tract Infect 2025;20(1):42-47. Published online April 30, 2025
- DOI: https://doi.org/10.14777/uti.2550014007
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Purpose
Chronic pelvic pain syndrome (CPPS) is a multifactorial condition that can significantly diminish quality of life. Although some patients have reported persistent pelvic pain after radical prostatectomy (RP), the prevalence and direct causal relationship between CPPS and RP remain unclear. This multicenter prospective study aimed to evaluate the efficacy of Urovaxom for improving CPPS symptoms. Materials and Methods: A total of 52 prostate cancer patients who underwent RP were enrolled and administered Urovaxom (60 mg/day) for 12 weeks. Changes in National Institutes of Health Chronic Prostatitis Symptom Index (NIH-CPSI), overactive bladder symptom score (OABSS), International Prostate Symptom Score (IPSS), and inflammation markers (white blood cell [WBC], C-reactive protein [CRP]) were analyzed using the Wilcoxon signed-rank test.
Results
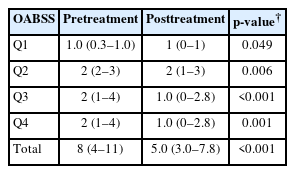
After 12 weeks of treatment, the NIH-CPSI total score significantly decreased from 19 (interquartile range [IQR], 16–23) to 12.5 (IQR, 8.0–16.8) (p<0.001). The OABSS total score decreased from 8 (IQR, 4–11) to 5 (IQR, 3.0–7.8), and the IPSS total score decreased from 13.5 (IQR, 10.0–22.8) to 10.5 (IQR, 5.0–17.0) (p<0.001). WBC levels showed a slight increase (p=0.028), but the clinical relevance of this change is uncertain and warrants further investigation. CRP changes were not statistically significant (p=0.274).
Conclusions
Urovaxom demonstrated significant efficacy in improving CPPS symptoms, particularly pain and reduced quality of life, in patients following RP. These findings suggest Urovaxom as a potential therapeutic option for CPPS after management using RP. -
Citations
Citations to this article as recorded by- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(1): 1. CrossRef - Addressing an Unmet Need in Postprostatectomy Care: Perspectives on Urovaxom
Byeong Jin Kang
Urogenital Tract Infection.2025; 20(2): 118. CrossRef
- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 6,214 View
- 57 Download
- 2 Crossref

Case Report
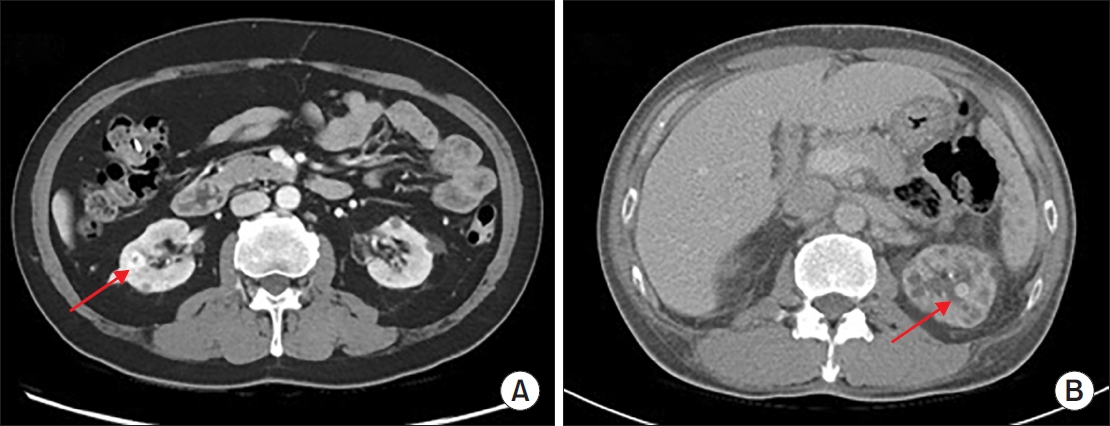
- Hemangioma Mistaken for Renal Cell Carcinoma in a Patient With End-Stage Renal Disease: A Case Report
- Hyung-Lae Lee, Dong-Gi Lee, Jeong Woo Lee, Jeonghyouk Choi
- Urogenit Tract Infect 2025;20(1):48-51. Published online April 30, 2025
- DOI: https://doi.org/10.14777/uti.2550008004
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Hemangiomas are rare, benign vascular neoplasms that are more common in patients with end-stage renal disease. Here, we describe 2 cases of hemangioma misdiagnosed as renal cell carcinoma before renal transplantation. The key finding in our case was the misdiagnosis of hemangiomas as renal cell carcinoma based on computed tomography and magnetic resonance imaging in patients with end-stage renal disease. Because living transplantation was planned for our patients, we performed rapid surgical resection of the heterogeneously enhancing renal masses to avoid delays in transplantation. Our case highlights the importance of rapid surgical resection of enhanced renal masses to confirm diagnosis, thereby avoiding delays in patients scheduled for renal transplantation.
-
Citations
Citations to this article as recorded by- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(1): 1. CrossRef
- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 2,704 View
- 23 Download
- 1 Crossref

Original Article
- Mortality and Risk Factors for Emphysematous Pyelonephritis in Korea: A Multicenter Retrospective Cohort Study
- Seung-Kwon Choi, Jeong Woo Lee, Seung Il Jung, Eu Chang Hwang, Joongwon Choi, Woong Bin Kim, Jung Sik Huh, Jin Bong Choi, Yeonjoo Kim, Jae Min Chung, Ju-Hyun Shin, Jae Hung Jung, Hong Chung, Sangrak Bae, Tae-Hyoung Kim
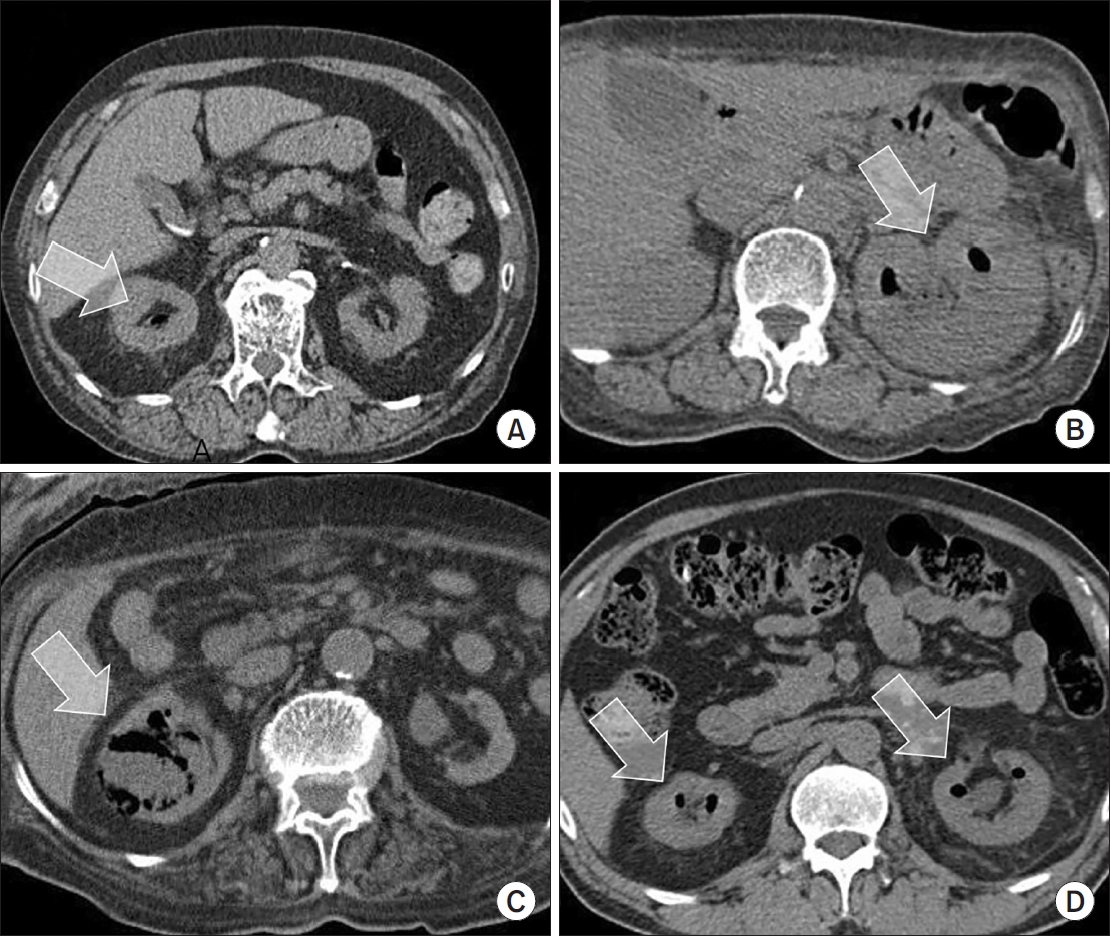
- Urogenit Tract Infect 2025;20(1):34-41. Published online April 30, 2025
- DOI: https://doi.org/10.14777/uti.2550006003
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Purpose
Emphysematous pyelonephritis (EPN) is a life-threatening disease requiring immediate treatment. This multicenter retrospective cohort study aimed to analyze the mortality rate and risk factors associated with EPN. Materials and Methods: Between January 2011 and February 2021, 217 patients diagnosed with EPN via computed tomography who visited 14 teaching hospitals were retrospectively analyzed. Clinical data, including age, sex, comorbidities, Huang and Tseng classification, hydronephrosis, acute kidney injury, blood and urine tests, surgical interventions, percutaneous drainage, and conservative treatments, were compared between the survival and death groups. Risk factors for mortality due to EPN were analyzed using univariate and multivariate methods.
Results
The mean age of survivors and deceased patients was 67.8 and 69.0 years, respectively (p=0.136). The sex distribution (male/female) was 48/146 and 8/15, respectively (p=0.298). Of the 217 patients, 23 died, resulting in a mortality rate of 10.6%. In univariate analysis, the Huang and Tseng classification (p=0.004), platelet count (p=0.005), and acute kidney injury (p=0.007) were significantly associated with mortality from EPN. In multivariate analysis, only the Huang and Tseng classification (p=0.029) was identified as a risk factor. Mortality rates according to the Huang and Tseng classification were as follows: class I (5.88%), class II (7.50%), class IIIa (14.28%), class IIIb (25.00%), and class IV (23.07%).
Conclusions
EPN is associated with a high mortality rate. Among various clinical factors, the Huang and Tseng classification was the most significant indicator for predicting mortality. -
Citations
Citations to this article as recorded by- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(1): 1. CrossRef
- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 4,115 View
- 77 Download
- 1 Crossref

Review Articles
- A Narrative Review of Syphilis Notification Systems in Korea: Change to Mandatory Surveillance System
- Seung-Ju Lee, Jin Bong Choi
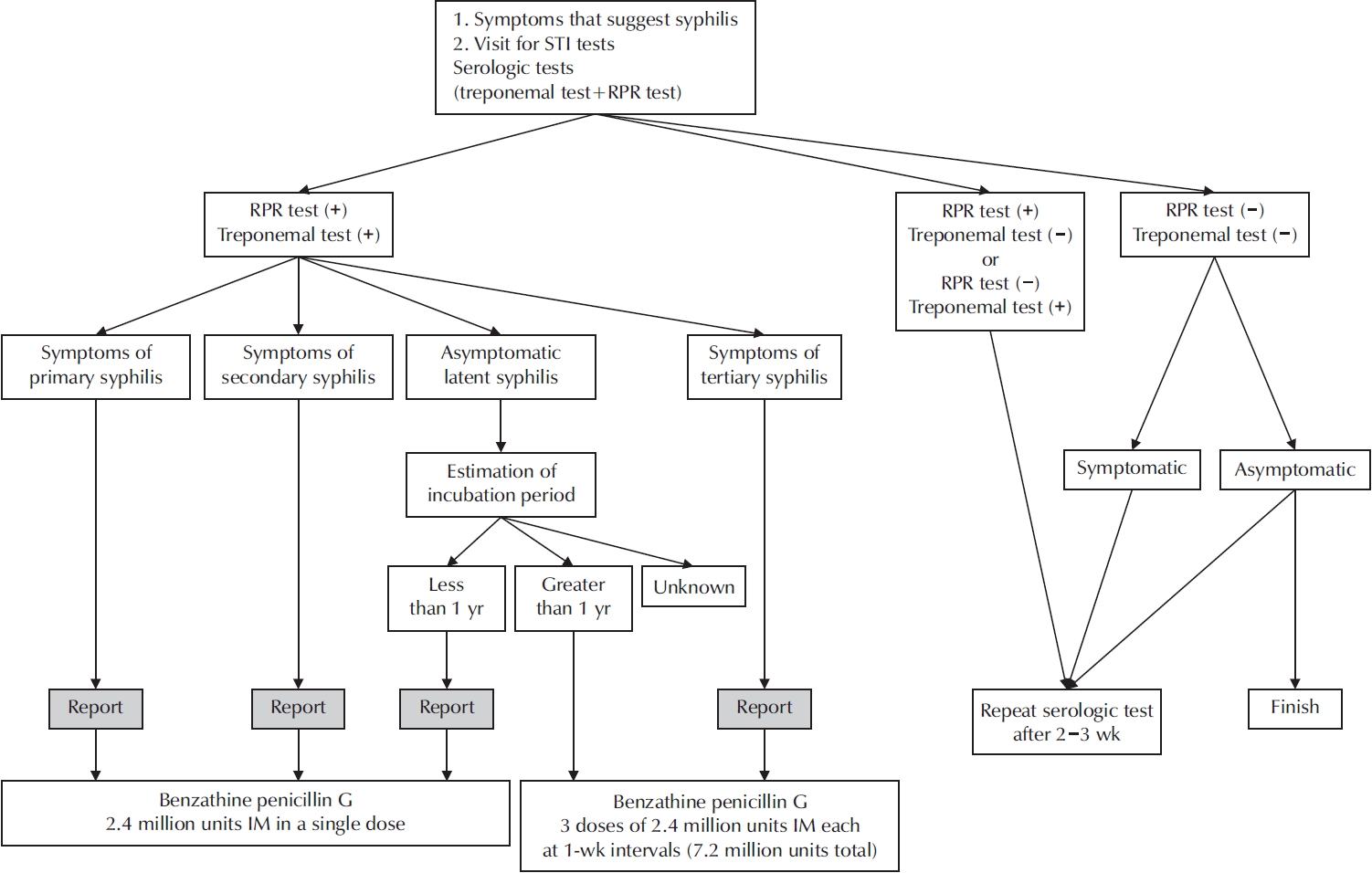
- Urogenit Tract Infect 2025;20(1):28-33. Published online April 30, 2025
- DOI: https://doi.org/10.14777/uti.2550004002
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - New cases of syphilis are clearly showing an increasing trend worldwide. However, in a sentinel surveillance system, the collection of information on disease outbreaks is limited, making it difficult to understand the overall outbreak situation and perform detailed analyses of patients' demographic characteristics and disease stages. In accordance with the revision of the Infectious Disease Prevention Act, syphilis was converted from a grade 4 infectious disease subject to sentinel surveillance to a grade 3 infectious disease subject to mandatory surveillance from January 1, 2024, with all medical institutions required to report syphilis diagnosis within 24 hours.
-
Citations
Citations to this article as recorded by- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(1): 1. CrossRef - Adult Syphilis: A Narrative Review of Clinical Insights and Public Health Implications in Urology
Seung-Ju Lee, Jin Bong Choi
Urogenital Tract Infection.2025; 20(3): 123. CrossRef
- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 6,150 View
- 43 Download
- 2 Crossref

- Emerging Insights Into Microbiome Therapeutics for Urinary Tract Infections: A Narrative Review
- Hoonhee Seo, Md Abdur Rahim, Indrajeet Barman, Mohammed Solayman Hossain, Hanieh Tajdozian, Fatemeh Ghorbanian, Md Sarower Hossen Shuvo, Jiho Choi, Sukyung Kim, Heejo Yang, Ho-Yeon Song
- Urogenit Tract Infect 2025;20(1):4-16. Published online April 30, 2025
- DOI: https://doi.org/10.14777/uti.2448034017
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Urinary tract infections (UTIs) are among the most common bacterial infections worldwide, affecting millions annually and posing a significant global health concern. Traditional therapies for UTIs are becoming increasingly ineffective due to rising drug resistance and their tendency to disrupt the host's healthy microbiota, leading to further side effects. Consequently, there is an urgent need to develop alternative therapeutic agents that differ from conventional regimens and have fewer or no side effects. In this context, microbiome therapeutics offer a promising solution, given their demonstrated efficacy against various infectious diseases. Advances in scientific technology, particularly next-generation sequencing, have deepened our understanding of urinary microbiome dynamics, revealing a complex interplay within the urobiome that influences the onset and progression of UTIs. Uropathogenic bacteria do not solely cause UTIs; shifts in the composition of the urinary microbiome and interactions within the microbial community, known as host-microbiota interactions, also play a significant role. Although recent studies underscore the potential of targeting the urinary microbiome to manage UTIs and related complications, this field is still emerging and faces numerous regulatory and technical challenges. Further in-depth and comprehensive research is required to advance this pioneering concept into clinical practice.
-
Citations
Citations to this article as recorded by- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
Koo Han Yoo
Urogenital Tract Infection.2025; 20(1): 1. CrossRef - Efficacy and safety of N-acetylcysteine vs. probiotics in in-vivo biofilm prevention on ureteral stents: a prospective randomized controlled pilot in vivo study
Iqbal Singh, Himanshu Agrawal, Shailender Maurya, Himanshu Tanwar, Sanjay Gupta, N. P. Singh
International Urology and Nephrology.2025; 58(3): 811. CrossRef
- Editorial for UTI 2025 Vol. 20 No. 1 - Highlights of This Issue’s Papers and the UTI Editors’ Pick
- 16,040 View
- 190 Download
- 2 Crossref

- The Necessity of Human Papillomavirus Vaccination in Men: A Narrative Review
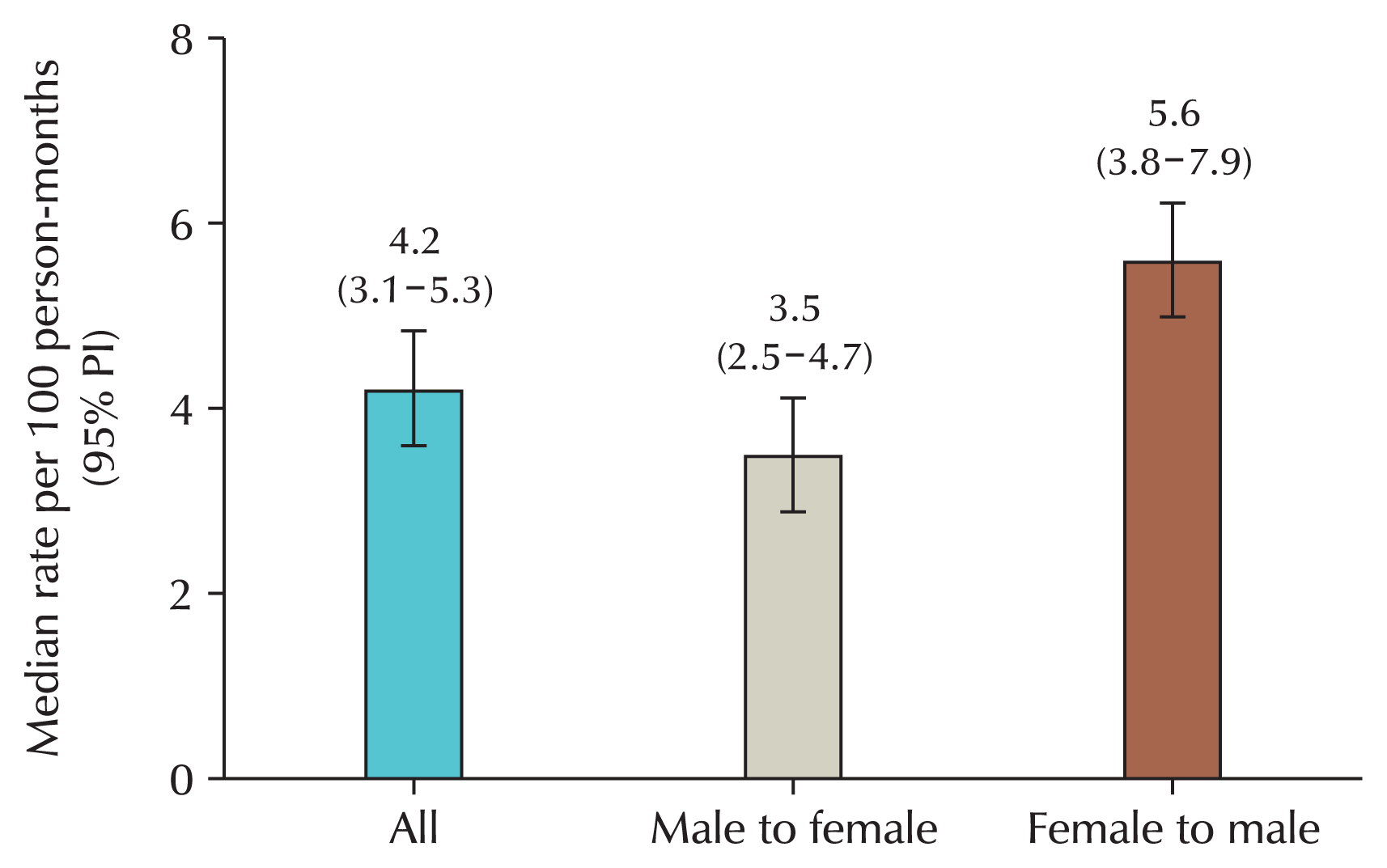
- Sooyoun Kim, Sangrak Bae
- Urogenit Tract Infect 2024;19(3):51-59. Published online December 31, 2024
- DOI: https://doi.org/10.14777/uti.2448030015
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Anogenital wart caused by human papillomavirus (HPV) is the most common sexually transmitted infection. High-risk strains, such as types 16 and 18, cause penile cancer in men, cervical and vulvar cancers in women, and head and neck cancers and anal cancer in both sexes. Since these malignant tumors can be prevented through vaccination, the importance of vaccination is emphasized. However, because HPV is known to cause cervical cancer, vaccination is only being administered to women. Some countries vaccinate men as well, but in South Korea, only girls are included in the National Immunization Program. However, screening for HPV in men is not possible, and the virus causes various malignant tumors, with a sharp increase in head and neck cancers, as well as a surge in genital warts in the country. In addition, HPV worsens sperm quality. Moreover, the need for vaccines is increasing as the known methods for preventing HPV-related diseases in men are decreasing and the disease burden is increasing. As cost-effectiveness studies have shown that the cost-effectiveness of vaccination is lower for men than for women, it is unlikely that male vaccination will be included in national immunization programs. Many countries overseas, especially a very small number of OECD (Organization for Economic Cooperation and Development) countries including South Korea, are implementing mandatory vaccination for women. Vaccinating men and women, would be cost-effective and efficient in achieving herd immunity. In addition to herd immunity, the inclusion of male vaccination in the National Immunization Program is imperative given the rapidly increasing incidence of diseases in men.
-
Citations
Citations to this article as recorded by- Prevalence of sexually transmitted infections among persons aged 15–24 in the Republic of Korea: A retrospective population-based descriptive study
Jinhee Seo, Minji Han, Sangrak Bae, Sooyoun Kim
Investigative and Clinical Urology.2026; 67(2): 201. CrossRef - Human Papillomavirus Infection and Vaccine Uptake Among Males in the United Arab Emirates and the Wider Middle East and North Africa Region: A Narrative Review
Humaid AlKaabi, Raya Abu-Khalaf, Sandra Abu-Khalaf, Layan Abu-Khalaf, Yahia Khalil
Cureus.2025;[Epub] CrossRef
- Prevalence of sexually transmitted infections among persons aged 15–24 in the Republic of Korea: A retrospective population-based descriptive study
- 12,877 View
- 130 Download
- 2 Crossref

Original Article
- Outbreak of Cystoscopy-Related Urinary Tract Infections With Pseudomonas aeruginosa in South Korea, 2022: A Case Series
- Beomsoo Kim, Young-Sin Choi, Jun-Koo Kang, Yun-Sok Ha, Seock Hwan Choi, Bum Soo Kim, Hyun Tae Kim, Eun Sang Yoo, Tae Gyun Kwon, Jae-Wook Chung, Tae-Hwan Kim
- Urogenit Tract Infect 2024;19(3):97-103. Published online December 31, 2024
- DOI: https://doi.org/10.14777/uti.2448028014
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Purpose
This study conducted an epidemiological investigation of Pseudomonas aeruginosa urinary tract infections (UTIs) following cystoscopy at Chilgok Kyungpook National University Hospital. Materials and Methods: From May 16 to July 15, 2022, among 353 patients who underwent cystoscopy, 6 patients reported febrile UTIs following cystoscopy. They were admitted to the urology department of the hospital after visiting the Emergency Department. P. aeruginosa was found in the urine cultures of 4 of the 6 hospitalized patients. During the epidemiological investigation, no changes were observed in factors such as the reprocessing procedures for endoscopic equipment. Therefore, microbiological tests were performed using environmental samples derived from the endoscopic equipment and cleaning process.
Results
P. aeruginosa was identified in a dual-enzymatic detergent (EmPower) used during the endoscope cleaning process. After changing the disinfectant and cleaning process, no further bacterial growth was observed in subsequent microbiological tests.
Conclusions
This study highlights the potential of cystoscopes to serve as reservoirs for bacteria due to inadequate cleaning during the disinfection process. To minimize the risk of infections following cystoscopy, it is important to pay close attention to the reprocessing and cleaning of cystoscopes. -
Citations
Citations to this article as recorded by- A Commentary on “Outbreak of Cystoscopy-Related Urinary Tract Infections With Pseudomonas aeruginosa in South Korea, 2022: A Case Series”
Byoungkyu Han
Urogenital Tract Infection.2025; 20(1): 52. CrossRef
- A Commentary on “Outbreak of Cystoscopy-Related Urinary Tract Infections With Pseudomonas aeruginosa in South Korea, 2022: A Case Series”
- 4,858 View
- 78 Download
- 1 Crossref

Review Article
- Postoperative Microscopic Pyuria and Role of Damage-Associated Molecular Pattern: A Literature Review
- Min-Kyu Kim, Ki Hong Kim
- Urogenit Tract Infect 2024;19(3):73-79. Published online December 31, 2024
- DOI: https://doi.org/10.14777/uti.2448026013
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - All patients who undergo transurethral prostate surgery exhibit pyuria and microscopic hematuria in postoperative urinalysis. Postoperative asymptomatic pyuria is associated with the inflammatory process and surface remodeling of the prostate, rather than infection. Various studies have investigated the incidence, duration, and risk factors for postoperative pyuria, noting that factors like age, surgery time, and prostate size can influence outcomes. Postoperative pyuria reflects tissue recovery and inflammation, and the use of antibiotics in asymptomatic patients may not be appropriate.
- 6,480 View
- 32 Download

Case Report
- Klebsiella pneumoniae-Induced Emphysematous Prostatic Abscess Accompanied by a Spinal Cord Infarction: Case Report
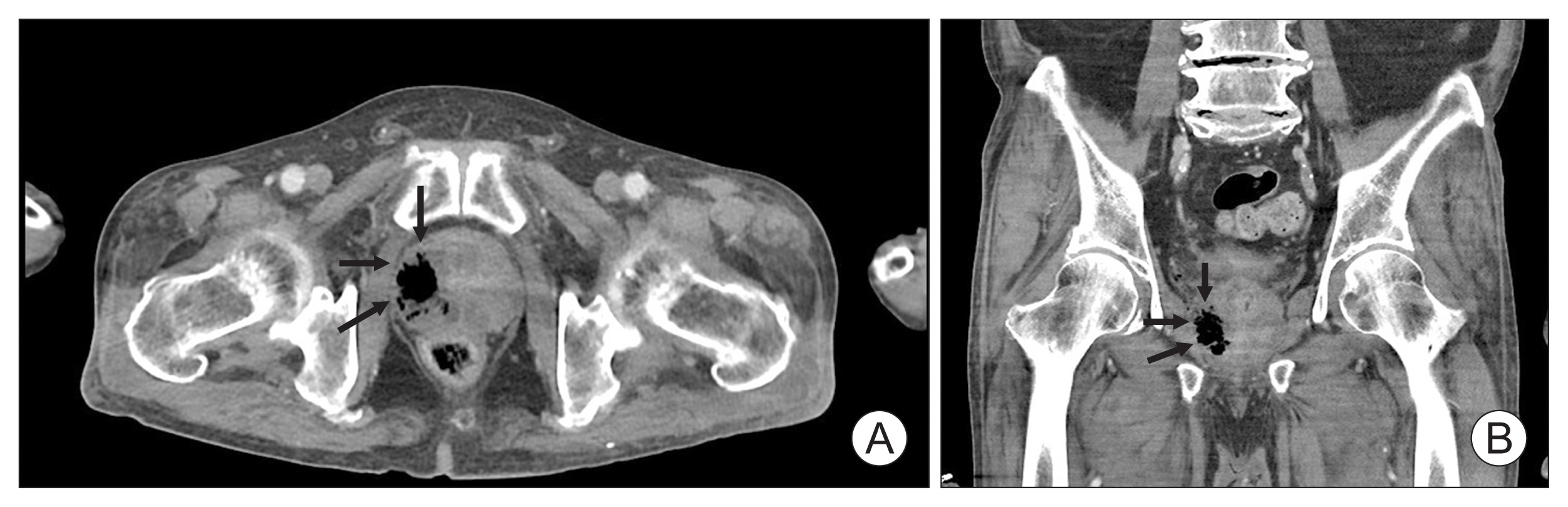
- Seong Uk Jeh, Min Sung Choi, Chang Seok Kang, Dae Hyun Kim, Jae Hwi Choi, See Min Choi, Sung Chul Kam, Jeong Seok Hwa, Jae Seog Hyun
- Urogenit Tract Infect 2024;19(3):104-108. Published online December 31, 2024
- DOI: https://doi.org/10.14777/uti.2448024012
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Various strains can be found in emphysematous prostatic abscesses (EPAs), but the most frequent causative organism is Klebsiella pneumoniae . Hypervirulent K. pneumoniae can disseminate to distant sites by forming a muco-polysaccharide network outside the capsule. Here, we present the first case of K. pneumoniae in an EPA accompanied by a spinal cord infarction. A 65-year-old man was referred to our hospital due to sudden-onset paraplegia after a 5-day history of fever, myalgia, and voiding difficulty. Abdominal computed tomography revealed a collection of air pockets in the prostate, and diffusion-weighted magnetic resonance imaging showed high signal intensity in the thoracic spinal cord. The patient was initially treated with antibiotics and surgical drainage. On the third hospital day, therapeutic heparin was added after discussion with a neurologist. The patient had no inflammatory symptoms, experienced some improvement in paraplegia, and was discharged on the 14th hospital day. This study adhered to the case report guidelines.
- 2,788 View
- 25 Download

Review Articles
- Mechanistic Insights Into Persistent Bacterial Cystitis as a Basis for Vaccine Development: A Narrative Review
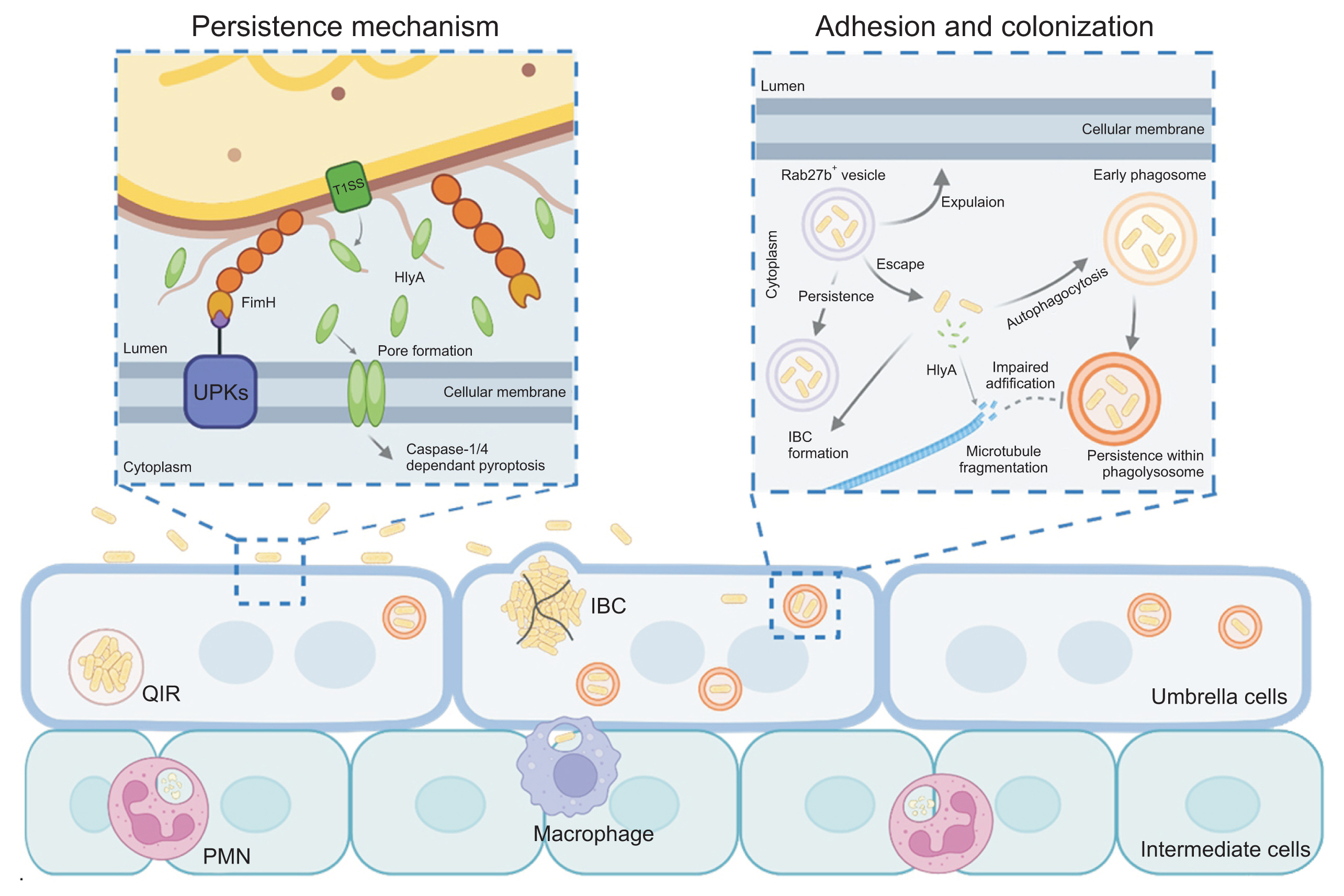
- Karen Serrano-Arevalo, Manisha Naskar, Hae Woong Choi
- Urogenit Tract Infect 2024;19(3):60-72. Published online December 31, 2024
- DOI: https://doi.org/10.14777/uti.2448022011
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Urinary tract infections (UTIs) are primarily caused by uropathogenic Escherichia coli (UPEC), which frequently lead to recurrent infections. These bacteria utilize several strategies to establish infection in the host; in particular, virulence factors such as fimbriae and α-hemolysin facilitate persistent infection, evade host immune responses, and minimize antibiotic exposure. To date, antibiotics have been the primary treatment for UTIs. However, an increasing emphasis has been placed on the need for UTI vaccines, with mucosal vaccine products now available in several countries. Additionally, vaccines targeting intracellular UPEC, utilizing adjuvants, are currently under development. Understanding the pathogenic mechanisms of uropathogens has enabled the development of new treatment approaches, paving the way for next-generation preventive and therapeutic methods that could effectively manage recurrent UTIs in the future.
-
Citations
Citations to this article as recorded by- Mechanisms and clinical implications of bacterial persistence in recurrent urinary tract infections
Changil Choi, Dong Soo Kim, Jin Bong Choi, Taesoo Choi, Jeong Woo Lee
Investigative and Clinical Urology.2026; 67(2): 123. CrossRef - Bacterial biofilm – as a contributor to urinary tract infections
Zuzanna Trześniewska-Ofiara, Mariola Mendrycka, Agnieszka Woźniak-Kosek
Biuletyn Głównej Biblioteki Lekarskiej.2025; 58(384): 83. CrossRef
- Mechanisms and clinical implications of bacterial persistence in recurrent urinary tract infections
- 8,179 View
- 83 Download
- 2 Crossref

- Artificial Intelligence for Autonomous Robotic Surgery in Urology: A Narrative Review
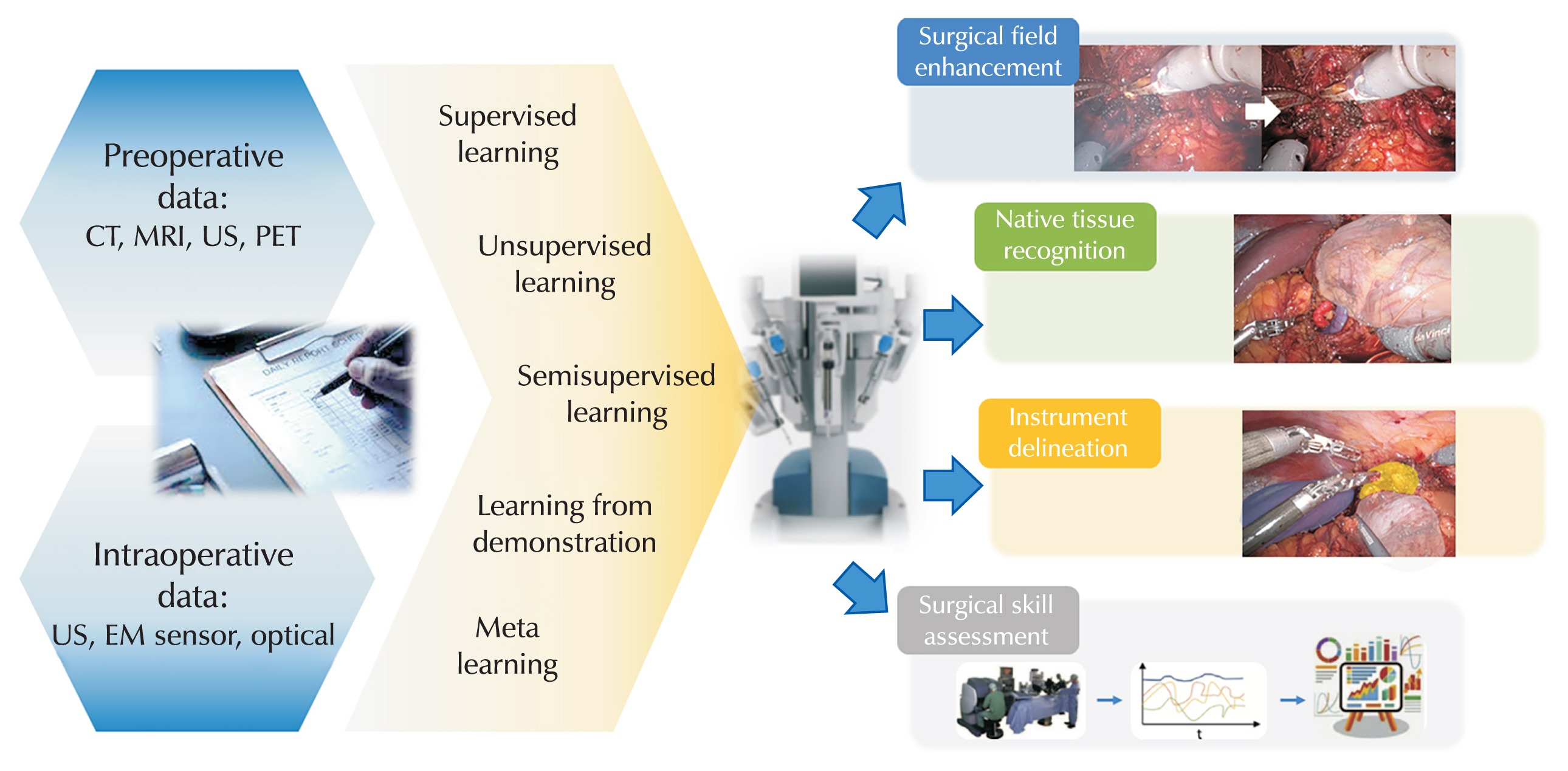
- Dae Young Lee, Hee Jo Yang
- Urogenit Tract Infect 2024;19(3):80-88. Published online December 31, 2024
- DOI: https://doi.org/10.14777/uti.2448020010
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Artificial intelligence (AI) has emerged as a transformative force in various sectors, including medicine, where it processes high-dimensional data to improve diagnostics and treatment outcomes. This review explores AI applications in urological surgery, highlighting advancements such as image classification and robotic assistance in surgical procedures. AI has demonstrated exceptional diagnostic accuracy, with some systems achieving up to 99.38% in detecting prostate cancer. Additionally, AI facilitates real-time anatomical recognition and instrument delineation, increasing surgical precision. While current robotic systems operate under human supervision, ongoing research aims to advance autonomous surgical capabilities. The future of AI in robotic surgery is promising, especially regarding the possibility of improved outcomes; nonetheless, challenges related to autonomy, safety, and ethics remain.
-
Citations
Citations to this article as recorded by- From data to decision: integrating causality AI and predictive analytics in endourological practice—a descriptive guide for clinicians from EAU Endourology
Chady Ghnatios, Zine-Eddine Khene, Rose Mary Attieh, Céline Mardelli, Carlotta Nedbal, Giovanni Cacciamani, Pieter De Backer, Peter Kronenberg, Tzevat Tefik, Ben Turney, Olivier Traxer, Bhaskar K. Somani, Frederic Panthier
World Journal of Urology.2026;[Epub] CrossRef
- From data to decision: integrating causality AI and predictive analytics in endourological practice—a descriptive guide for clinicians from EAU Endourology
- 15,450 View
- 192 Download
- 1 Crossref

Original Article
- Impact of the Timing of Percutaneous Nephrostomy on the Prognosis of Obstructive Urolithiasis With Sepsis: A Retrospective Cohort Study
- Ji Eun Yu, Hyung Joon Kim, Hong Wook Kim, Young Seop Chang, Jin Bum Kim, Dong Hoon Koh
- Urogenit Tract Infect 2024;19(3):89-96. Published online December 31, 2024
- DOI: https://doi.org/10.14777/uti.2448018009
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Purpose
The aim of this study was to investigate the prognostic impact of time to percutaneous nephrostomy (PCN) insertion on obstructive ureteral stones with sepsis. Materials and Methods: Data were collected on patients who presented at our Emergency Department between 2017 and 2021 with obstructive uropathy due to urinary stones and underwent PCN insertion. Patients were stratified into 4 groups in accordance with the quick sepsis-related organ failure (qSOFA) score at presentation (<2 or ≥2) and time to PCN insertion (<4 hours or ≥4 hours) as follows: group 1, qSOFA < 2 and time to PCN insertion < 4 hours; group 2, qSOFA < 2 and time to PCN insertion ≥ 4 hours; group 3, qSOFA ≥ 2 and time to PCN insertion < 4 hours; group 4, qSOFA ≥ 2 and time to PCN insertion ≥ 4 hours. The prognostic impacts of the time to PCN insertion were compared between these groups
Results
The total cohort consisted of 96 patients, of whom 70 were classified as either group 1 or 2 (qSOFA < 2). Overall, 37 patients had a positive urine culture. The median time to PCN insertion was 218 minutes, and the median length of stay was 14 days. The hospitalization period was significantly shorter in group 3 than in group 4 (p=0.041).
Conclusions
A shorter length of stay was associated with more rapid PCN insertion in patients with obstructive uropathy and a high risk of sepsis. -
Citations
Citations to this article as recorded by- Clinical Characteristics, Microbiological Spectrum, Biomarkers, and Imaging Insights in Acute Pyelonephritis and Its Complicated Forms—A Systematic Review
Marius-Costin Chițu, Teodor Salmen, Paula-Roxana Răducanu, Carmen-Marina Pălimariu, Bianca-Margareta Salmen, Anca Pantea Stoian, Viorel Jinga, Dan Liviu Dorel Mischianu
Medicina.2026; 62(1): 222. CrossRef
- Clinical Characteristics, Microbiological Spectrum, Biomarkers, and Imaging Insights in Acute Pyelonephritis and Its Complicated Forms—A Systematic Review
- 5,513 View
- 45 Download
- 1 Crossref

Case Report
- Hyperbaric Oxygen Therapy for the Treatment of Chronic Prostatitis/Chronic Pelvic Pain Syndrome: Case Report
- Kwang Jin Kim, Yoonsuk Lee, Yong Sung Cha, Tae Wook Kang, Hyun Chul Chung, Hong Chung, Hyun Kim, Jae Hung Jung
- Urogenit Tract Infect 2024;19(2):44-47. Published online August 31, 2024
- DOI: https://doi.org/10.14777/uti.2024.19.2.44
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Hyperbaric oxygen therapy (HBOT) was conducted on two male patients with chronic prostatitis/chronic pelvic pain syndrome who were resistant to conventional medical therapies. Both patients underwent 20 sessions of 100% oxygen inhalation (2.0 atmosphere absolute for 90 min/day, five days/week for four weeks) in a hyperbaric chamber. The follow-up period was three months. Although the patients reported a slight improvement in the pain domain of the National Institutes of Health-Chronic Prostatitis Symptom Index (NIH-CPSI) after HBOT, no changes were noted in the other domains of NIH-CPSI and International Prostate Symptom Score. No adverse events were encountered during or after HBOT.
- 6,359 View
- 42 Download


 KAUTII
KAUTII

 First
First Prev
Prev