Current issue
- Page Path
- HOME > Browse Articles > Current issue
Editorial
- Editorial for Urogenital Tract Infection 2026 Vol. 21 No. 1 - Highlights of This Issue’s Papers and the Urogenital Tract Infection Editors’ Pick
- Tae Gyun Kwon, Phil Hyun Song, Koo Han Yoo
- Urogenit Tract Infect 2026;21(1):1-2. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2026edi01
- 277 View
- 12 Download

Review Articles
- Urinary Tract Infection and Urolithiasis: A Narrative Review of Pathophysiological Links and Clinical Implications
- Dong Sup Lee
- Urogenit Tract Infect 2026;21(1):3-10. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2652002001
-
 Abstract
Abstract
 PDF
PDF PubReader
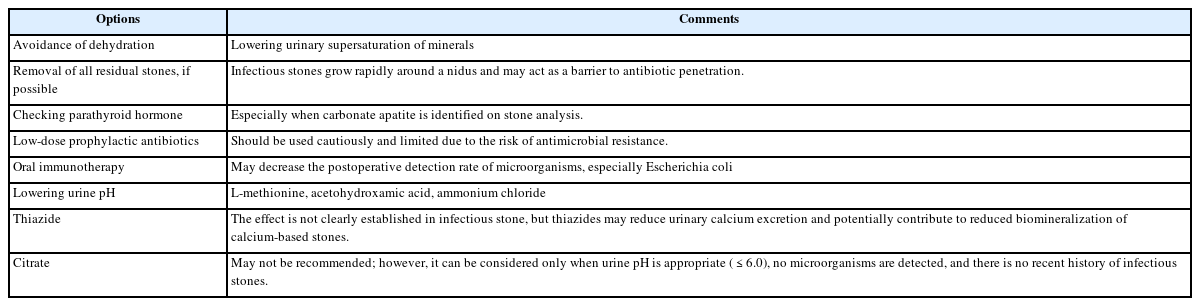
PubReader - Urinary tract infection (UTI) and urolithiasis are closely related clinical entities that frequently coexist and influence each other’s pathogenesis and clinical course. Infection-related stones, particularly struvite and carbonate apatite stones, have long been recognized as consequences of ureaseproducing bacterial infections. However, recent evidence suggests that the role of microorganisms—especially Escherichia coli—in stone disease may extend beyond traditional infection stones; in particular, biofilm formation by microorganisms may contribute to the formation and growth of calcium-based stones. This review summarizes current knowledge on the pathophysiological mechanisms linking UTI and urolithiasis, with a focus on the biochemical processes underlying infection-related stone formation, the characteristics of different stone compositions, and emerging concepts regarding bacterial involvement in metabolic stone disease. A better understanding of the interplay between UTI and urolithiasis may improve preventive strategies, guide antimicrobial and surgical decision-making, and ultimately reduce recurrence rates. This review highlights the need for an integrated clinical approach that considers both infectious and metabolic factors in patients with urinary stone disease.
- 359 View
- 10 Download

- Beyond Empirical Antibiotics: Toward Precision-Based Urinary Tract Infection Management and Korea-Specific Guidelines
- Sang Rak Bae, Hee Jo Yang
- Urogenit Tract Infect 2026;21(1):11-14. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2550048024
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader - Urinary tract infection (UTI) remains one of the most common bacterial infections, yet rising antimicrobial resistance and changing healthcare environments have challenged the traditional empiric approach to antibiotic therapy. Recent international guidelines from the European Association of Urology (EAU), Infectious Diseases Society of America (IDSA), and American Urological Association (AUA) collectively demonstrate a paradigm shift toward precision diagnostics, evidencebased antibiotic selection, standardized nonantibiotic prevention strategies, and simplified disease classification systems. The EAU has emphasized culture-based diagnosis, expanded nonantibiotic prophylaxis, and introduced a new framework distinguishing localized from systemic UTI. The IDSA has strengthened restrictions on treating asymptomatic bacteriuria, provided guidance for managing antimicrobial-resistant organisms, and simplified UTI categories. The AUA similarly highlights culture-directed diagnosis and the minimization of prophylactic antibiotics in women with recurrent UTI while formalizing nonantibiotic preventive measures. In Korea, unique resistance patterns, high extended-spectrum beta-lactamase and fluoroquinolone resistance rates, and frequent movement of patients between long-term care facilities and hospitals underscore the need for Korea-specific UTI guidelines. Although national surveillance systems such as KARMS (Korean Antimicrobial Resistance Monitoring System) and KorGLASS (Global Antimicrobial Resistance Surveillance System in Korea) provide valuable data, the evidence base remains insufficient to match the robustness of international guideline development. Establishing updated, Korean-contextualized UTI guidelines is essential for improving patient safety, optimizing antimicrobial stewardship, and effectively responding to the growing threat of resistance. The field is at a pivotal turning point, requiring proactive leadership and coordinated action within Korea’s urological and infectious disease communities.
- 329 View
- 9 Download

Original Articles
- The Korean Antimicrobial Resistance Monitoring System for Complicated Urinary Tract Infections: A Prospective Multicenter Observational Study Conducted by the Korean Association of Urogenital Tract Infection and Inflammation
- Seong Hyeon Yu, Seung Il Jung, Donghoon Lim, Jeong Woo Lee, Seung-Ju Lee, Hong Chung, Mi-Mi Oh, Jing Bong Choi, Jae Hung Jung, Hee Jo Yang, KAUTII Investigators
- Urogenit Tract Infect 2026;21(1):15-25. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2550040020
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader - Purpose
This study aimed to report antimicrobial resistance (AMR) patterns among patients with complicated urinary tract infection (cUTI) using data from the Korean Antimicrobial Resistance Monitoring System (KARMS). Materials and Methods: In this prospective, multicenter, observational surveillance study, data from patients diagnosed with cUTI between January 2023 and September 2025 were retrieved from the KARMS database. Demographic characteristics, uropathogen distribution, and antimicrobial susceptibility profiles of representative pathogens were analyzed.
Results
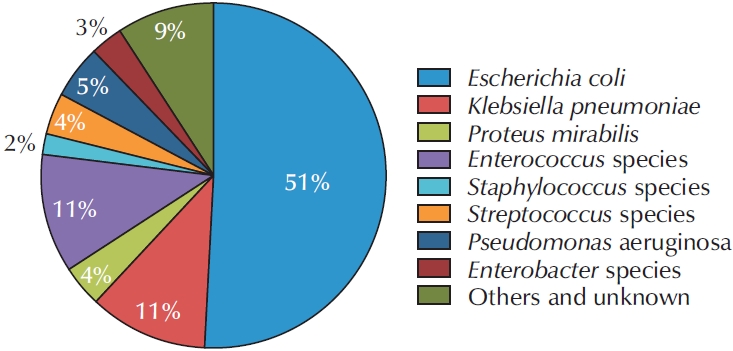
Data from a total of 698 patients were collected in the KARMS database. The mean patient age was 68.94±15.95 years. The numbers of patients with healthcare-associated UTI and recurrent UTI were 171 (24.5%) and 240 (34.4%), respectively. Escherichia coli was the most frequently identified uropathogen (n=356, 51.1%). Regarding antimicrobial susceptibility, 92.9% of isolates were susceptible to fosfomycin, 75.5% to nitrofurantoin, 47.2% to ciprofloxacin, 63.3% to cefotaxime, 80.6% to piperacillin/tazobactam, and 98.8% to ertapenem. The rate of extended-spectrum beta-lactamase positivity was 45.2% (166 of 367) and was significantly higher in pyelonephritis and urosepsis (62.3% and 62.5%, p=0.002), healthcare-associated UTI (58.6%, p=0.040), and recurrent cUTI (53.2%, p=0.028). Fluoroquinolone resistance was significantly more common in female patients (49.1%, p=0.021) and in healthcare-associated UTI (57.9%, p=0.014). Piperacillin/tazobactam resistance was significantly higher in patients with urosepsis (37.0%, p=0.004), in tertiary hospitals (17.2%, p=0.019), and in healthcare-associated UTI (26.4%, p=0.001). In addition, third-generation cephalosporin resistance was significantly higher in secondary hospitals than in tertiary hospitals (43.5% vs. 33.3%, p=0.041).
Conclusions
These data provide current information on uropathogen distribution and AMR patterns in cUTI in South Korea. Continued surveillance and ongoing data accumulation through KARMS will support evidence-based strategies for optimal antimicrobial therapy and AMR mitigation.
- 330 View
- 13 Download

- Identification of Plasma Biomarker Signatures for Acute and Chronic Cystitis Using Olink Explore Proteomics in UK Biobank
- Chang Gu Kang, Su Kang Kim
- Urogenit Tract Infect 2026;21(1):26-39. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2550046023

-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader - Purpose
Acute and chronic cystitis represent common yet biologically distinct inflammatory disorders of the lower urinary tract. However, circulating biomarkers capable of differentiating these conditions remain poorly defined. Materials and Methods: Using COMPASS-processed Olink Explore proteomic data from UK Biobank participants, we compared plasma protein profiles across individuals with acute cystitis, chronic cystitis, and normal controls. After stringent quality-control procedures, covariate-adjusted regression models and differential abundance analyses were performed. STRING-based proteinprotein interaction (PPI) networks were constructed to examine systems-level organization of significantly altered proteins.
Results
Among 2,715 participants, acute and chronic cystitis demonstrated distinct systemic proteomic signatures. CHGA (chromogranin A) and GAST (gastrin) were consistently elevated across both phenotypes, indicating shared neuroendocrine-associated systemic responses. Acute cystitis showed selective elevation of CDH2 (cadherin-2), whereas chronic cystitis demonstrated marked increases in GDF15 (growth differentiation factor 15). PPI network analysis revealed a densely interconnected architecture in acute cystitis and a more modular, branch topology in chronic cystitis, reflecting differing organizational patterns of circulating proteins.
Conclusions
This population-level analysis identifies phenotype-specific and shared plasma protein signatures associated with acute and chronic cystitis and provides an initial framework for understanding systemic inflammatory profiles in these conditions. Interpretation should remain cautious given the cross-sectional design, reliance on historical diagnostic classification, and the absence of bladder-specific molecular data. Nonetheless, these findings highlight candidate biomarkers that merit further validation in longitudinal and mechanistic studies.
- 372 View
- 9 Download

Case Report
- Bilateral Xanthogranulomatous Pyelonephritis With Extensive Abscess Associated With Neurogenic Bladder: A Case Report
- Sin Woo Lee, Hee Seung Choi
- Urogenit Tract Infect 2026;21(1):40-43. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2550026013
-
 Abstract
Abstract
 PDF
PDF PubReader
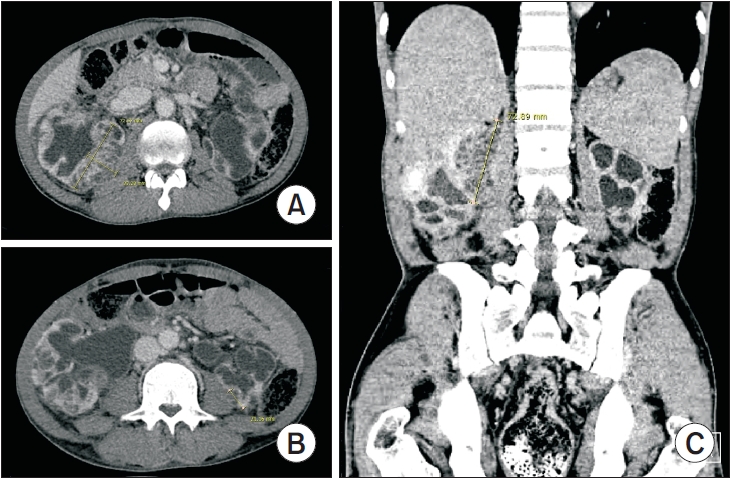
PubReader - Xanthogranulomatous pyelonephritis (XGP) is a rare and severe form of chronic pyelonephritis. We report a case of bilateral XGP complicated by extensive abscess formation. A 47-year-old man presented with fatigue and generalized weakness. Laboratory evaluation revealed leukocytosis and elevated serum creatinine levels. Urinalysis demonstrated pyuria and bacteriuria. Computed tomography (CT) revealed bilaterally enlarged kidneys with multifocal renal parenchymal and perirenal abscesses. The CT scan also demonstrated severe bilateral hydronephroureter and diffuse bladder wall thickening, with a radiologic impression of severe pyelonephritis with abscess formation and neurogenic bladder. The patient was admitted and treated with intravenous antibiotics and percutaneous nephrostomy tube placement. However, no clinical improvement was observed with conservative management. The patient subsequently underwent right open radical nephrectomy. Histopathological examination confirmed the diagnosis of XGP with extensive abscess formation. The patient experienced no further complications or recurrence after surgery. This case suggests that chronic untreated neurogenic bladder may contribute to the development of severe chronic pyelonephritis such as XGP.
- 269 View
- 8 Download

Letter to the Editor
- A Commentary on “Clinical Characteristics and Risk Factors of Fournier Gangrene: A 15-Years Multicenter Retrospective Study in Korea”
- Jae Yoon Kim
- Urogenit Tract Infect 2026;21(1):44-45. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2652016008
- 195 View
- 6 Download







 First
First Prev
Prev