Abstract
-
Purpose
This study aimed to report antimicrobial resistance (AMR) patterns among patients with complicated urinary tract infection (cUTI) using data from the Korean Antimicrobial Resistance Monitoring System (KARMS).
-
Materials and Methods
In this prospective, multicenter, observational surveillance study, data from patients diagnosed with cUTI between January 2023 and September 2025 were retrieved from the KARMS database. Demographic characteristics, uropathogen distribution, and antimicrobial susceptibility profiles of representative pathogens were analyzed.
-
Results
Data from a total of 698 patients were collected in the KARMS database. The mean patient age was 68.94±15.95 years. The numbers of patients with healthcare-associated UTI and recurrent UTI were 171 (24.5%) and 240 (34.4%), respectively. Escherichia coli was the most frequently identified uropathogen (n=356, 51.1%). Regarding antimicrobial susceptibility, 92.9% of isolates were susceptible to fosfomycin, 75.5% to nitrofurantoin, 47.2% to ciprofloxacin, 63.3% to cefotaxime, 80.6% to piperacillin/tazobactam, and 98.8% to ertapenem. The rate of extended-spectrum beta-lactamase positivity was 45.2% (166 of 367) and was significantly higher in pyelonephritis and urosepsis (62.3% and 62.5%, p=0.002), healthcare-associated UTI (58.6%, p=0.040), and recurrent cUTI (53.2%, p=0.028). Fluoroquinolone resistance was significantly more common in female patients (49.1%, p=0.021) and in healthcare-associated UTI (57.9%, p=0.014). Piperacillin/tazobactam resistance was significantly higher in patients with urosepsis (37.0%, p=0.004), in tertiary hospitals (17.2%, p=0.019), and in healthcare-associated UTI (26.4%, p=0.001). In addition, third-generation cephalosporin resistance was significantly higher in secondary hospitals than in tertiary hospitals (43.5% vs. 33.3%, p=0.041).
-
Conclusions
These data provide current information on uropathogen distribution and AMR patterns in cUTI in South Korea. Continued surveillance and ongoing data accumulation through KARMS will support evidence-based strategies for optimal antimicrobial therapy and AMR mitigation.
-
Keywords: Urinary tract infection, Republic of Korea, Antibiotic resistance
HIGHLIGHTS
The antimicrobial resistance (AMR) of complicated urinary tract infection (cUTI) in South Korea has reached a serious level, not only fluoroquinolone and 3rd generation cephalosporin, even in piperacillin/tazobactam. In addition, AMR of cUTI was especially higher in healthcare-associated UTI.
INTRODUCTION
Urinary tract infection (UTI) is one of the most common bacterial infections worldwide [
1]. Clinically, UTIs are categorized as uncomplicated or complicated based on clinical presentation, anatomical involvement, and infection severity [
2,
3]. Uncomplicated cystitis accounts for the majority of UTIs and typically presents with localized symptoms such as dysuria, urgency, frequency, and a sensation of incomplete bladder emptying [
4]. In contrast, complicated UTI (cUTI) is often accompanied by systemic symptoms, including fever, chills, and costovertebral angle pain or tenderness, and is associated with higher morbidity and mortality due to the possibility of secondary bloodstream infection [
2,
5]. cUTIs are generally linked to specific anatomical or functional urinary tract abnormalities or compromised host defenses, making them more difficult to eradicate than uncomplicated UTIs [
6].
The primary treatment for cUTI is antimicrobial therapy, along with appropriate management of the underlying anatomical or functional abnormalities. Optimal antibiotic selection depends on infection severity, host factors, and local microbiological patterns. However, cUTIs occur in a heterogeneous patient population with diverse comorbidities, resulting in a broader range of causative microorganisms compared to uncomplicated infections. Additionally, the global emergence and rapid spread of multidrug-resistant organisms, including extended-spectrum β-lactamase (ESBL)-producing
Escherichia coli and carbapenem-resistant
Enterobacterales, has made treatment increasingly challenging and represents a significant public health concern [
7,
8]. The prevalence of antimicrobial resistance (AMR) in cUTI is particularly high in Asian regions, including South Korea [
9,
10], contributing to substantial clinical and socioeconomic burdens through increased morbidity and mortality [
2]. Therefore, continuous surveillance of AMR is essential to obtain accurate information on pathogen distribution, microbiological characteristics, and antimicrobial susceptibility patterns in the community, which is crucial for optimizing cUTI treatment strategies.
In response to these needs, the Korean Association of Urogenital Tract Infection and Inflammation (KAUTII) established the Korean Antimicrobial Resistance Monitoring System (KARMS) in 2023 to facilitate nationwide surveillance of AMR. KARMS for UTIs is a web-based monitoring program (
https://uti.karms.kr/main-page, accessed from 1 January 2023) that operates through collaboration with medical centers throughout South Korea. To date, KARMS provides continuously updated national data on AMR in UTIs [
1,
3]. The present study aimed to provide an interim report for the prevalence and AMR patterns of representative uropathogens in patients with cUTI.
MATERIALS AND METHODS
1. KARMS and Participating Institutions
KARMS was established in 2023 as a web-based, prospective, multicenter, national observational surveillance system for AMR in UTIs. The system is officially endorsed by the KAUTII and is implemented through cooperation with medical centers nationwide via the KARMS website (
https://uti.karms.kr/main-page, accessed from 1 January 2023). To date, a total of 32 hospitals have participated in KARMS. These hospitals are located across 6 administrative provinces in South Korea (Seoul, Gyeonggi-do, Chungcheong-do, Jeolla-do, Gyeongsang-do, and Gangwon-do).
Thirty-four urologists contributed clinical data to the KARMS registry for patients aged 18 years and older who were diagnosed with clinically and microbiologically confirmed cUTI. The collected data included nationality, age, sex, outpatient or inpatient status, menopausal status (for women), association classification (community-acquired, healthcare-associated, or hospital-acquired), uncomplicated or complicated status, UTI classification (cystitis, pyelonephritis, catheter-associated UTI, acute prostatitis, chronic prostatitis, asymptomatic bacteriuria, or urosepsis), and recurrence status. cUTI was defined as a UTI occurring in individuals with specific anatomical or functional urinary tract abnormalities or compromised host defenses, including urinary obstruction or retention due to anatomical or neurological disease, immunosuppression, renal failure, renal transplantation, pregnancy, or the presence of foreign bodies such as calculi, indwelling catheters, or other urinary drainage devices [
5]. Healthcare-associated UTI was defined as an infection detected at or within 48 hours of hospital admission based on specific criteria, including transfer from longterm care facilities, hemodialysis, immunosuppression, active or metastatic cancer, contact with family members infected with multidrug-resistant organisms, advanced age or physical disability, recent surgery (within 6 months), or treatment with radiation therapy [
11]. Hospital-acquired UTI was defined as an infection detected after the initial 48 hours of hospital admission [
11]. Recurrent UTI was defined as 3 or more UTIs within 1 year or 2 or more UTIs within the last 6 months [
3]. Investigators were provided reference definitions mentioned above from the KARMS website. Data for patients with clinically and microbiologically confirmed cUTI from January 2023 to September 2025 were retrieved and analyzed. Of the 2005 cases recorded in the KARMS database, 1,307 were excluded due to age <18 years, mixed or negative urine culture results, or diagnosis of uncomplicated UTI.
All patients in the present study underwent urine culture with subsequent identification of the isolated uropathogen. ESBL positivity and antimicrobial susceptibility testing were performed in each participating hospital using automated systems or standard microbiological methods, and interpreted according to Clinical and Laboratory Standards Institute (CLSI) breakpoints [
12]. Carbapenemase screening was also performed as a part of the routine workflow of the local clinical microbiology laboratories. Antimicrobial susceptibility was classified as S (susceptible), I (intermediate), or R (resistant), based on CLSI interpretive breakpoints [
13]. Susceptibility data were collected for the following antimicrobial agents: amikacin, amoxicillin/clavulanate, cefazolin, cefepime, cefotaxime, cefoxitin, ceftazidime, ciprofloxacin, ertapenem, fosfomycin, gentamycin, imipenem, levofloxacin, meropenem, nitrofurantoin, piperacillin/tazobactam, and trimethoprim/sulfamethoxazole.
Statistical analyses were performed using Stata 16.1 (StataCorp LLC, USA). Descriptive analyses were conducted to summarize the demographic characteristics of the study population. Continuous variables are reported as means and standard deviations, and categorical variables are reported as frequencies (%). ESBL positivity and resistance to fluoroquinolones, third-generation cephalosporins, and piperacillin/tazobactam were compared according to clinical variables (sex, hospital type, UTI classification, association, and recurrence status) using Pearson 2-sided chi-square test or Fisher exact test, as appropriate. A p-value <0.05 was considered statistically significant.
5. Security and Ethics Statement
All data were managed under the security policies of the KAUTII, with access control implemented through user authentication and firewall protection to prevent unauthorized access. Data were accessible only to approved investigators, and compressed research files were provided with password protection. This study protocol was reviewed and approved by the institutional review board of Chonnam National University Hospital (CNUH-2024-085) and Chonnam National University Hwasun Hospital (CNUHH-2023-017). The study was conducted in accordance with the principles of the Declaration of Helsinki and the Ethical Guidelines for Clinical Studies. Patient consent was waived because only anonymized registry data were analyzed.
RESULTS
1. Baseline Characteristics
A total of 698 patients with cUTI were eligible for inclusion in the present study from the KARMS database. The baseline characteristics of the study population are summarized in
Table 1. The mean age was 68.94±15.95 years, and 449 patients (64.3%) were female. The numbers of patients treated at primary, secondary, and tertiary medical centers were 4 (0.6%), 126 (18.0%), and 568 (81.4%), respectively. With respect to geographic distribution, the largest proportion of patients were from Gangwon-do province (n=228, 32.7%), followed by Jeolla-do (n=143, 20.5%), Gyeonggi-do (n=121, 17.3%), Seoul (n=114, 16.3%), Chungcheong-do (n=84, 12.0%), and Gyeongsang-do (n=8, 1.2%). A total of 171 patients (24.5%) had healthcare-associated UTI and 240 (34.4%) had recurrent UTI. Regarding UTI classification, 66 (9.5%) had acute prostatitis, 86 (12.3%) had catheter-associated UTI, 8 (1.1%) had chronic prostatitis, 252 (36.1%) had cystitis, 136 (19.5%) had pyelonephritis, and 32 (4.6%) had urosepsis. Data without any UTI classification were considered as unknown (n=76, 10.9%). ESBL positivity was identified as 45.2% (166 of 367).
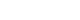
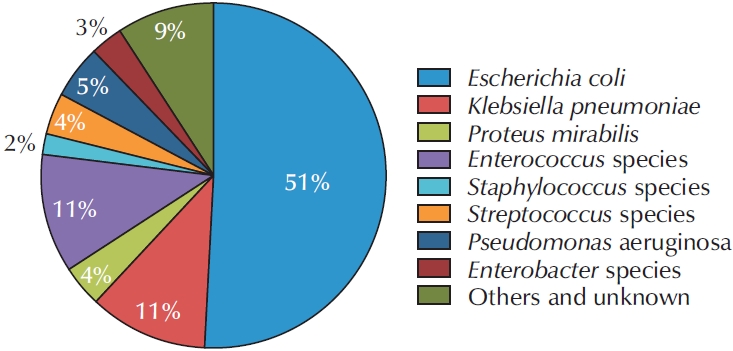
E. coli was the most frequently identified uropathogen (n=356, 51.1%), followed by
Enterococcus species (n=80, 11.5%) and
Klebsiella pneumoniae (n=76, 10.9%). In addition, other pathogens accounted for approximately 9% of isolates, as shown in
Fig. 1.
The antimicrobial susceptibility patterns of isolates obtained from patients with cUTI are presented in
Table 2. Overall, susceptibility rates were 47.2% (296 of 627) for ciprofloxacin, 63.3% (210 of 332) for cefotaxime, 92.9% (118 of 127) for fosfomycin, 75.5% (333 of 441) for nitrofurantoin, 92.7% (455 of 491) for amikacin, 70.7% (205 of 290) for amoxicillin/clavulanate, 60.2% (247 of 410) for trimethoprim/sulfamethoxazole, 80.6% (441 of 547) for piperacillin/tazobactam, and 98.8% (508 of 514) for ertapenem. In summary, the resistance rates to ciprofloxacin and cefotaxime were 52.8% and 36.7%, respectively.
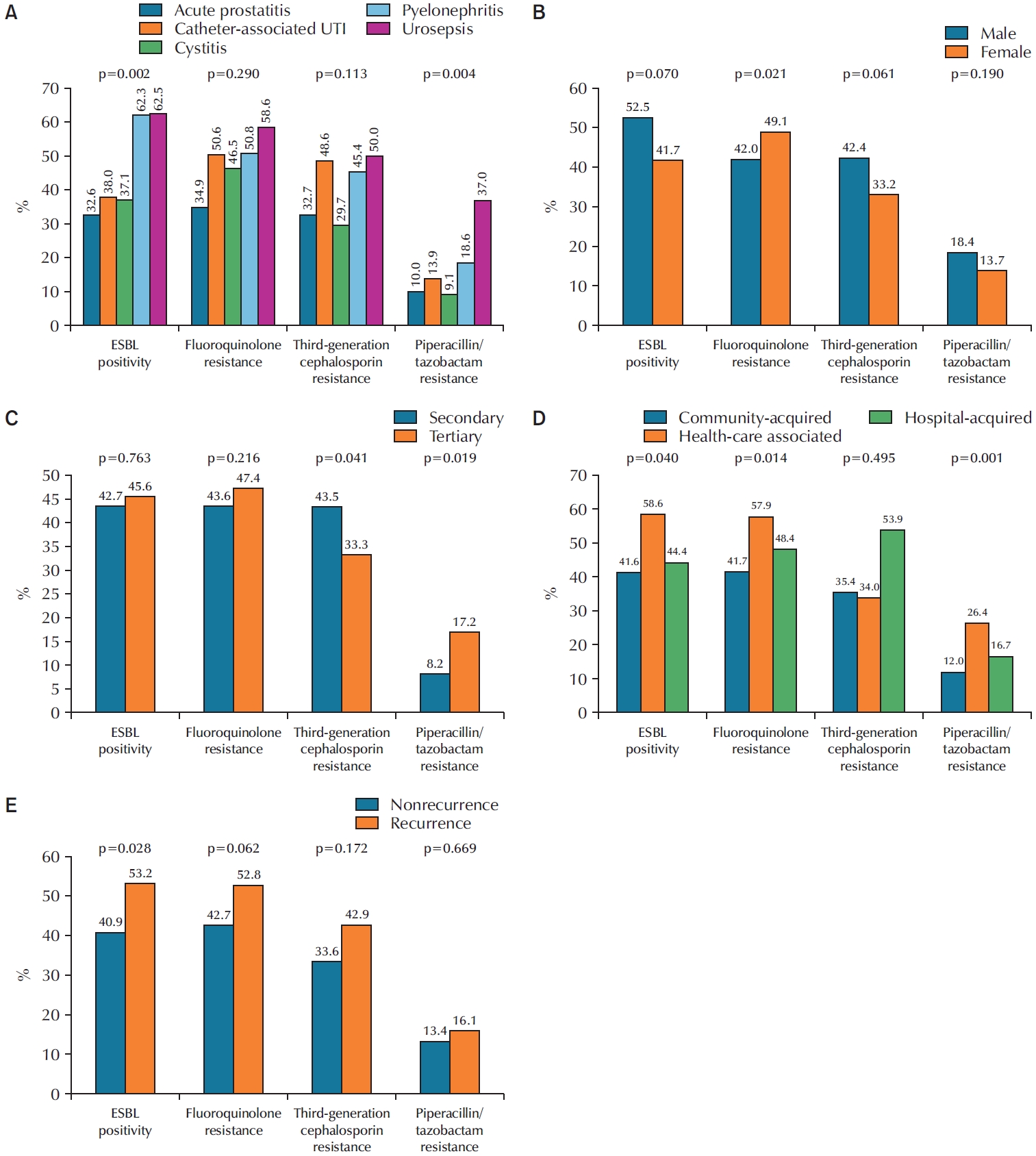
Rates of ESBL positivity, fluoroquinolone resistance, third-generation cephalosporin resistance, and piperacillin/tazobactam resistance were compared according to clinical characteristics, including sex, hospital type, UTI classification, infection association, and recurrence status. Detailed subgroup analyses are presented in
Fig. 2A–
E. ESBL positivity was significantly higher in patients with pyelonephritis and urosepsis (acute prostatitis, 32.6%; catheter-associated UTI, 38.0%; cystitis, 37.1%; pyelonephritis, 62.3%; urosepsis, 62.5%; p=0.002), in healthcare-associated UTI (community-acquired, 41.6%; healthcare-associated, 58.6%; hospital-acquired, 44.4%; p=0.040), and in recurrent cUTI (nonrecurrent, 40.9%; recurrent, 53.2%; p=0.028). Fluoroquinolone resistance was significantly higher in female patients (male, 42.0%; female, 49.1%; p=0.021) and in healthcare-associated UTI (community-acquired, 41.7%; healthcare-associated, 57.9%; hospital-acquired, 48.4%; p=0.014). Piperacillin/tazobactam resistance was significantly higher in patients with urosepsis (acute prostatitis, 10.0%; catheter-associated UTI, 13.9%; cystitis, 9.1%; pyelonephritis, 18.6%; urosepsis, 37.0%; p=0.004), in tertiary hospitals (secondary, 8.2%; tertiary, 17.2%; p=0.019), and in healthcare-associated UTI (community-acquired, 12.0%; healthcare-associated, 26.4%; hospital-acquired, 16.7%; p=0.001). Additionally, third-generation cephalosporin resistance was significantly higher in secondary hospitals compared with tertiary hospitals (43.5% vs. 33.3%, p=0.041).
DISCUSSION
Antimicrobial agents remain the cornerstone of treatment for UTIs. However, AMR has risen rapidly in recent years and is now considered a global public health con-cern [
7,
8]. Major international public health organizations, including the World Health Organization, World Economic Forum, Centers for Disease Control and Prevention, and Infectious Diseases Society of America, have identified AMR as one of the most urgent threats to global health [
14,
15]. In response to this growing challenge, the Korean Association of Urogenital Tract Infection and Inflammation (KAUTII) established a nationwide AMR surveillance system, the KARMS for UTI. KARMS is a webbased, prospective, multicenter, national observational program implemented through collaboration among medical centers throughout South Korea (
https://uti. karms.kr/main-page, accessed from 1 January 2023). This structure enables continuous and efficient AMR monitoring with reduced time and resource requirements, and more than 2000 clinical entries have been recorded to date. In the present analysis of cUTI cases within the KARMS database,
E. coli was the most frequently identified uropathogen, and AMR rates among cUTI isolates had reached concerning levels, particularly with respect to fluoroquinolones, third-generation cephalosporins, and piperacillin/tazobactam. AMR rates were especially elevated among patients with healthcare-associated cUTI.
cUTI is not uncommon and frequently occurs in individuals with host-related risk factors, such as diabetes or immunosuppression, or in those with anatomical or functional abnormalities of the urinary tract, such as obstruction or impaired bladder emptying associated with detrusor dysfunction [
5]. As with uncomplicated UTI, cUTI may be caused by gram-negative or gram-positive bacteria, although
E. coli remains the most prevalent uropathogen, followed by
Enterococcus species,
Klebsiella species,
Pseudomonas aeruginosa, and
Proteus mirabilis [
9,
10,
16]. Previous studies have reported that
E. coli accounts for approximately 40% to 60% of cUTI cases, a proportion generally lower than that observed in uncomplicated UTI, likely due to the greater clinical heterogeneity and broader range of predisposing conditions in cUTI populations [
9,
10,
16]. In the present study,
E. coli accounted for 51.1% of cases, followed by
Enterococcus species (11.5%),
Klebsiella pneumoniae (10.9%), and
Pseudomonas aeruginosa (4.7%), consistent with prior data. Additionally, ESBL positivity was 45.2%, and was significantly higher among patients with pyelonephritis and urosepsis (acute prostatitis, 32.6%; catheter-associated UTI, 38.0%; cystitis, 37.1%; pyelonephritis, 62.3%; urosepsis, 62.5%; p=0.002), in healthcareassociated UTI (community-acquired, 41.6%; healthcareassociated, 58.6%; hospital-acquired, 44.4%; p=0.040), and in recurrent cUTI (nonrecurrence, 40.9%; recurrence, 53.2%; p=0.028). ESBL-producing gram-negative organisms are resistant to most β-lactam antibiotics, including extended-spectrum cephalosporins and monobactams, and their global prevalence continues to rise [
17]. The elevated ESBL rate observed in this study may reflect the distribution of patient populations with differing socio-environmental exposures, anatomical or functional urinary tract abnormalities, and underlying comorbidities [
18].
The primary therapeutic approach for patients with cUTI is the use of antimicrobial agents. However, cUTI typically presents with systemic symptoms such as fever, chills, and costovertebral angle pain or tenderness, and is often associated with risk factors that increase the likelihood of a more complicated clinical course and reduce treatment success [
2,
5,
6]. Furthermore, AMR in cUTI is generally higher than in uncomplicated UTI across most antimicrobial agents [
16,
19] and is associated with increased morbidity and mortality.
In the present study, resistance rates to ciprofloxacin and cefotaxime among patients with cUTI were 52.8% and 36.7%, respectively. These rates were higher than those reported for uncomplicated cystitis in the KARMS database, which demonstrated 41.6% resistance to fluoroquinolones and 16.4% resistance to third-generation cephalosporins [
3]. Compared with a South Korean nationwide cUTI registry study conducted in 2008, the current resistance rates represent increases of approximately 10% for ciprofloxacin and 35% for cefotaxime [
16]. Third-generation cephalosporin resistance among cUTI pathogens in South Korea has therefore reached a critical level. Clinicians should take this into consideration when selecting empiric antimicrobial therapy, and unnecessary or nonjudicious use of third-generation cephalosporins should be avoided. In addition, the resistance rate to piperacillin/tazobactam was 19.4% in the present study. Piperacillin/tazobactam is a combination of an extended-spectrum penicillin and a β-lactamase inhibitor used to treat a wide range of serious bacterial infections and is active against many gram-positive and gram-negative organisms, including
Pseudomonas aeruginosa [
20]. However, if the upward trend in resistance continues, resistance to piperacillin/tazobactam may also reach clinically concerning levels. On the other hand, fosfomycin has shown a high susceptibility of over 90% for cUTI. Although fosfomycin is mainly recommended for acute uncomplicated cystitis, it may have a possibility in the treatment of cUTI, particularly in the outpatient settings.
The present study also evaluated differences in AMR to fluoroquinolones, third-generation cephalosporins, and piperacillin/tazobactam according to clinical factors such as sex, hospital type, UTI classification, infection association, and recurrence status. In detailed analysis, healthcare-associated UTI showed higher resistance rates to fluoroquinolones (community-acquired, 41.7%; healthcare-associated, 57.9%; hospital-acquired, 48.4%; p=0.014) and piperacillin/tazobactam (community-acquired, 12.0%; healthcare-associated, 26.4%; hospital-acquired, 16.7%; p=0.001). Third-generation cephalosporin resistance was 34%. When compared with previous reports of healthcare-associated UTI, the current AMR rates have not changed substantially over the past decade (ciprofloxacin, 50%, cephalosporins, 35%– 50% [
9]; ciprofloxacin, 54.9%, cephalosporins, 42% [
10]) However, in the present study, resistance to fluoroquinolones and piperacillin/tazobactam in healthcare-associated UTI was significantly higher than in hospital-acquired UTI. Several factors may contribute to these findings, but inappropriate antibiotic use without adherence to local, national, or international stewardship guidelines is likely the most significant. For example, a nationwide registry study of UTI management in South Korea reported that 28% of urologists did not obtain a urine culture before initiating treatment, and 54% did not obtain a urine culture even in cases of initial treatment failure [
21]. Prolonged misuse of antimicrobials can lead to the development of multidrug-resistant organisms by gradually altering normal gastrointestinal and vaginal microbiota [
18]. In addition, the number of healthcare institutions in South Korea has increased rapidly due to socio-environmental changes, including population aging and the rising prevalence of chronic medical diseases [
22]. These facilities frequently care for elderly patients who may have impairments in communication, mobility, or cooperation due to conditions such as dementia, cerebral infarction, Parkinson disease, and spinal cord injuries [
23,
24]. Although these patients often present with various urologic problems, they may not receive appropriate management due to limited access to certified urologists and insufficient nursing staff trained in antimicrobial stewardship principles [
25]. Therefore, clinicians and healthcare providers working in these settings must prioritize efforts to address the growing AMR burden in healthcare-associated UTI.
AMR in patients with cUTI in South Korea has already reached a critical level, particularly among healthcare-associated cases. Although the benefits of antibiotics in reducing mortality and prolonging life expectancy are undeniable, the indiscriminate and prolonged use of these agents has substantially contributed to the rise of AMR [
26]. Therefore, comprehensive antimicrobial stewardship programs are urgently required to optimize clinical outcomes, ensure cost-effective therapy, and minimize the unintended consequences of inappropriate antibiotic use [
27]. Antimicrobial stewardship encompasses a series of coordinated interventions designed to promote the appropriate use of antimicrobials. These include regular training of healthcare staff in the optimal application of antimicrobial agents; strict adherence to local, national, and international treatment guidelines; systematic audits of adherence and treatment outcomes; ongoing monitoring and feedback to prescribers; and the evaluation of local pathogen resistance trends [
28]. Despite the global emphasis on such initiatives, South Korea currently lacks an official nationwide antimicrobial stewardship program. Consequently, establishing a robust stewardship framework in conjunction with the ongoing AMR surveillance system is essential to address this growing threat effectively.
This study has several limitations. First, although it was a web-based, prospective, multicenter, and nationwide observational study, potential selection bias may exist due to regional and institutional disparities in patient inclusion and UTI classification. As a result, standardization and quality control of data could not be fully ensured. Second, methodologies for pathogen identification and antimicrobial susceptibility testing were not uniform across all institutions. Nonetheless, all laboratories adhered to their respective microbial standards, and susceptibility results were interpreted according to the CLSI breakpoints [
13]. Third, because data entry relied on multiple investigators within a web-based system, inter-investigator variability may have influenced the dataset. In fact, geographic distribution is imbalanced due to differences in participating hospitals, regional demographics, or data-entry profiles. Consequently, the lack of centralized verification is a limitation of this study. Fourth, several possible confounders (e.g., outpatient antibiotic exposure, device status, prior hospitalization and relevant comorbidities) are unmeasured in this study. This might contribute to the results of subgroup analysis. Therefore, further investigations including these possible confounders are needed.
Despite these limitations, the present study provides valuable and timely insights into the distribution of uropathogens and the current status of AMR in cUTI within South Korea during the ongoing global AMR crisis. The KARMS initiative for UTI continues to collect and monitor nationwide data, enabling the identification of emerging resistance patterns and temporal trends. Such continuous surveillance will be instrumental in reducing AMR through evidence-based prescribing and the avoidance of unnecessary antibiotic use.
CONCLUSIONS
In the context of the ongoing global AMR crisis, continuous surveillance is essential to guide the selection of optimal antibiotics based on accurate susceptibility data. To address this critical need, the KARMS was established for the nationwide surveillance of AMR in UTIs and is officially endorsed by the KAUTII. In the present study focusing on cUTI, the resistance rates to ciprofloxacin and cefotaxime were found to have reached an alarming level, and resistance to piperacillin/tazobactam remains particularly concerning. These findings underscore the urgent need for continuous monitoring and systematic data accumulation to curb the escalation of AMR. In this regard, the KARMS system provides contemporary nationwide surveillance data on AMR patterns in cUTI and may support evidence-based empirical antibiotic selection in South Korea.
NOTES
-
Funding/Support
This study received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
-
Research Ethics
This study protocol was reviewed and approved by the institutional review board of Chonnam National University Hospital (CNUH-2024-085) and Chonnam National University Hwasun Hospital (CNUHH-2023-017). The study was conducted in accordance with the principles of the Declaration of Helsinki and the Ethical Guidelines for Clinical Studies. Patient consent was waived because only anonymized registry data were analyzed.
-
Conflict of Interest
DL, HC, and JHJ, members of the Editorial Board of Urogenital Tract Infection, are authors of this article. However, they played no role whatsoever in the editorial evaluation of this article or the decision to publish it. The other authors have nothing to disclose.
-
Acknowledgments
The authors thank the following urologists for their contributions of case material and patient information: Dae Hee Kim (Tower Urologic Clinic, Seoul), Doo Sang Kim (Soonchunhyang University Cheonan Hospital, Cheonan), Su Jin Kim (The Catholic University of Korea, St. Vincent’s Hospital, Suwon), Yeon Ju Kim (Daegu Fatima Hospital, Daegu), Woong Bin Kim (Bucheon St. Mary’s Hospital, College of Medicine, The Catholic University of Korea, Bucheon), Tae Heon Kim (Bundang CHA Hospital, CHA University College of Medicine, Seongnam), Hwanik Kim (Hallym University Sacred Heart Hospital, College of Medicine, Hallym University, Anyang), Seong Woong Na (Gwangju Veterans Hospital, Gwangju), Kyeong Ho Ryu (Goldman Urologic Clinic, Seoul), Seung Ki Min (Goldman Urologic Clinic, Seoul), Jun Baek Park (National Police Hospital, Seoul), Tae Young Park (Uijeongbu Eulji Medical Center, Eulji University, Uijeongbu), Sangrak Bae (The Catholic University of Korea, Uijeongbu St. Mary’s Hospital, College of Medicine, Uijeongbu), Yumi Seo (Dankook University College of Medicine, Cheonan), Ju Hyeon Shin (Chungnam National University Hospital, Daejeon), So Yeon Lee (Myongji Hospital, Ilsan), Yeong Hoon Lee (Yonsei Cham Urologic Clinic, Ilsan), Hae Do Jung (Inje University Ilsan Baik Hospital, Ilsan), Hee Ju Jo (Joheeju Urologic Clinic, Incheon), Chang Il Choi (Hallym University Dongtan Sacred Heart Hospital, College of Medicine, Hallym University, Hwaseong), Yun Seok Ha (Kyungpook National University Hospital, Daegu), Eu Chang Hwang (Chonnam National University Medical School, Chonnam National University Hwasun Hospital, Hwasun), and Jin Cheol Hwang (Grand Urologic Clinic, Seongnam).
-
Author Contribution
Conceptualization: SHY, SIJ; Data curation: SHY, SIJ, DHL, JWL, SJL, HJ, MMO, JBC, JHJ, HJY; Methodology: SHY, SIJ, JWL, SJL; Writing - original draft: SHY; Writing - review & editing: SHY, SIJ.
Fig. 1.Distribution of uropathogens in patients with complicated urinary tract infection.
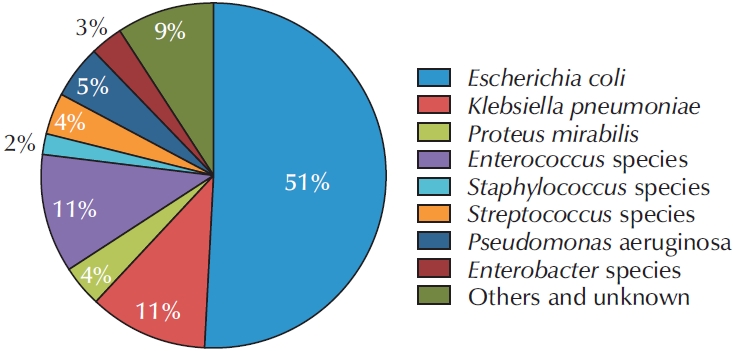
Fig. 2.Extended-spectrum β-lactamase (ESBL) positivity, fluoroquinolone resistance, third-generation cephalosporin resistance, and piperacillin/tazobactam resistance in complicated urinary tract infection according to clinical factors: urinary tract infection (UTI) classification (A), sex (B), hospital type (C), UTI association (D), and recurrence of infection (E).
Table 1.Demographic characteristics of patients with complicated urinary tract infection (N=698)
|
Variable |
Value |
|
Age (yr) |
68.94±15.95 |
|
Sex |
|
|
Male |
249 (35.7) |
|
Female |
449 (64.3) |
|
Hospital type |
|
|
Primary |
4 (0.6) |
|
Secondary |
126 (18.0) |
|
Tertiary |
568 (81.4) |
|
Hospital region |
|
|
Seoul |
114 (16.3) |
|
Gyeonggi-do |
121 (17.3) |
|
Gyeongsang-do |
8 (1.2) |
|
Jeolla-do |
143 (20.5) |
|
Chungcheong-do |
84 (12.0) |
|
Gangwon-do |
228 (32.7) |
|
Outpatient |
565 (81.0) |
|
Recurrent UTI |
240 (34.4) |
|
Association |
|
|
Community-acquired |
466 (66.8) |
|
Healthcare-associated |
171 (24.5) |
|
Hospital-acquired |
35 (5.0) |
|
Unknown |
26 (3.7) |
|
UTI classification |
|
|
Acute prostatitis |
66 (9.5) |
|
Catheter-associated UTI |
86 (12.3) |
|
Chronic prostatitis |
8 (1.1) |
|
Cystitis |
252 (36.1) |
|
Pyelonephritis |
136 (19.5) |
|
Urosepsis |
32 (4.6) |
|
Asymptomatic bacteriuria |
42 (6.0) |
|
Unknown |
76 (10.9) |
|
ESBL positive (n=367) |
166 (45.2) |
Table 2.Antimicrobial susceptibility patterns in patients with complicated urinary tract infection
|
Antibiotics susceptibility |
Value |
|
Amikacin |
455/491 (92.7) |
|
Amoxicillin/clavulanate |
205/290 (70.7) |
|
Cefepime |
392/571 (68.7) |
|
Cefotaxime |
210/332 (63.3) |
|
Cefoxitin |
429/512 (83.8) |
|
Ceftazidime |
378/560 (67.5) |
|
Ciprofloxacin |
296/627 (47.2) |
|
Levofloxacin |
174/393 (44.3) |
|
Ertapenem |
508/514 (98.8) |
|
Fosfomycin |
118/127 (92.9) |
|
Gentamicin |
441/632 (69.8) |
|
Imipenem |
503/541 (93.0) |
|
Meropenem |
341/362 (94.2) |
|
Nitrofurantoin |
333/441 (75.5) |
|
Piperacillin/tazobactam |
441/547 (80.6) |
|
Trimethoprim/sulfamethoxazole |
247/410 (60.2) |
REFERENCES
- 1. Yu SH, Jung SI, Lee SJ, Oh MM, Choi JB, Choi CI, et al. Antimicrobial resistance of escherichia coli for uncomplicated cystitis: Korean Antimicrobial Resistance Monitoring System. Antibiotics (Basel) 2024;13:234.ArticlePubMedPMC
- 2. Flores-Mireles AL, Walker JN, Caparon M, Hultgren SJ. Urinary tract infections: epidemiology, mechanisms of infection and treatment options. Nat Rev Microbiol 2015;13:269-84.ArticlePubMedPMCPDF
- 3. Yu SH, Jung SI, Lee SJ, Oh MM, Choi JB, Choi CI, et al. Nationwide surveillance of antimicrobial resistance for uncomplicated cystitis in 2023: Conducted by the Korean Association of Urogenital Tract Infection and Inflammation. Investig Clin Urol 2025;66:161-71.ArticlePubMedPMCPDF
- 4. Foxman B. Epidemiology of urinary tract infections: incidence, morbidity, and economic costs. Dis Mon 2003;49:53-70.ArticlePubMed
- 5. Lichtenberger P, Hooton TM. Complicated urinary tract infections. Curr Infect Dis Rep 2008;10:499-504.ArticlePubMedPDF
- 6. Spoorenberg V, Hulscher ME, Geskus RB, de Reijke TM, Opmeer BC, Prins JM, et al. [Better antibiotic use in complicated urinary tract infections; multicentre cluster randomised trial of 2 improvement strategies]. Ned Tijdschr Geneeskd 2016;160:D460.PubMed
- 7. Aslam B, Wang W, Arshad MI, Khurshid M, Muzammil S, Rasool MH, et al. Antibiotic resistance: a rundown of a global crisis. Infect Drug Resist 2018;11:1645-58.ArticlePubMedPMCPDF
- 8. Jernigan JA, Hatfield KM, Wolford H, Nelson RE, Olubajo B, Reddy SC, et al. Multidrug-resistant bacterial infections in U.S. hospitalized patients, 2012-2017. N Engl J Med 2020;382:1309-19.ArticlePubMedPMC
- 9. Cek M, Tandoğdu Z, Wagenlehner F, Tenke P, Naber K; Bjerklund-Johansen TE. Healthcare-associated urinary tract infections in hospitalized urological patients--a global perspective: results from the GPIU studies 2003-2010. World J Urol 2014;32:1587-94.ArticlePubMedPDF
- 10. Choe HS, Lee SJ, Cho YH, Çek M, Tandoğdu Z, Wagenlehner F, et al. Aspects of urinary tract infections and antimicrobial resistance in hospitalized urology patients in Asia: 10-year results of the Global Prevalence Study of Infections in Urology (GPIU). J Infect Chemother 2018;24:278-83.PubMed
- 11. Choi JB, Lee S. Healthcare-associated urinary tract infection: multi drug resistance and risk factors. Urogenit Tract Infect 2018;13:21-5.ArticlePDF
- 12. Humphries RM, Abbott AN, Hindler JA. Understanding and addressing CLSI breakpoint revisions: a primer for clinical laboratories. J Clin Microbiol 2019;57:e00203-19.ArticlePubMedPMCPDF
- 13. Weinstein MP, Lewis JS. The clinical and laboratory standards institute subcommittee on antimicrobial susceptibility testing: background, organization, functions, and processes. J Clin Microbiol 2020;58:e01864-19.ArticlePubMedPMCPDF
- 14. Michael CA, Dominey-Howes D, Labbate M. The antimicrobial resistance crisis: causes, consequences, and management. Front Public Health 2014;2:145.ArticlePubMedPMC
- 15. Spellberg B, Srinivasan A, Chambers HF. New societal approaches to empowering antibiotic stewardship. JAMA 2016;315:1229-30.ArticlePubMedPMC
- 16. Lee SJ, Lee DS, Choe HS, Shim BS, Kim CS, Kim ME, et al. Antimicrobial resistance in community-acquired urinary tract infections: results from the Korean Antimicrobial Resistance Monitoring System. J Infect Chemother 2011;17:440-6.ArticlePubMed
- 17. Castanheira M, Simner PJ, Bradford PA. Extended-spectrum β -lactamases: an update on their characteristics, epidemiology and detection. JAC Antimicrob Resist 2021;3:dlab092.PubMedPMC
- 18. Kostakioti M, Hultgren SJ, Hadjifrangiskou M. Molecular blueprint of uropathogenic Escherichia coli virulence provides clues toward the development of anti-virulence therapeutics. Virulence 2012;3:592-4.ArticlePubMedPMC
- 19. Grados MC, Thuissard IJ, Alós JI. Stratification by demographic and clinical data of the antibiotic susceptibility of Escherichia coli from urinary tract infections of the community. Aten Primaria 2019;51:494-8.ArticlePubMedPMC
- 20. El-Haffaf I, Caissy JA, Marsot A. Piperacillin-tazobactam in intensive care units: a review of population pharmacokinetic analyses. Clin Pharmacokinet 2021;60:855-75.ArticlePubMedPMCPDF
- 21. Bae S. Practice pattern survey I : analysis study on the actual clinical practices for cystitis treatment. 2024 KUA abstract 2024.EP-015.
- 22. Yu SH, Hwang EC, Jung SI. Care of voiding dysfunction in rehabilitation and convalescent hospitals. Urogenit Tract Infect 2021;16:32-43.Article
- 23. Jung HB, Kim HJ, Cho ST. A current perspective on geriatric lower urinary tract dysfunction. Korean J Urol 2015;56:266-75.ArticlePubMedPMC
- 24. Lee SH, Cho ST, Na HR, Ko SB, Park MH. Urinary incontinence in patients with Alzheimer's disease: relationship between symptom status and urodynamic diagnoses. Int J Urol 2014;21:683-87.PubMed
- 25. Lee SH, Suh J, Kim HS, Lee YJ, Lee SR, Kim KH, et al. Prevalence and management status of urologic diseases in geriatric hospitals in South Korea: a field research. Investig Clin Urol 2017;58:70-6.ArticlePubMedPMCPDF
- 26. Adedeji WA. The treasure called antibiotics. Ann Ib Postgrad Med 2016;14:56-7.PubMedPMC
- 27. Dellit TH, Owens RC, McGowan JE, Gerding DN, Weinstein RA, Burke JP, et al. Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America guidelines for developing an institutional program to enhance antimicrobial stewardship. Clin Infect Dis 2007;44:159-77.PubMed
- 28. Schuts EC, Hulscher ME, Mouton JW, Verduin CM, Stuart JW, Overdiek HW, et al. Current evidence on hospital antimicrobial stewardship objectives: a systematic review and meta-analysis. Lancet Infect Dis 2016;16:847-56.ArticlePubMed
 , Seung Il Jung1
, Seung Il Jung1 , Donghoon Lim2
, Donghoon Lim2 , Jeong Woo Lee3
, Jeong Woo Lee3 , Seung-Ju Lee4
, Seung-Ju Lee4 , Hong Chung5
, Hong Chung5 , Mi-Mi Oh6
, Mi-Mi Oh6 , Jing Bong Choi7
, Jing Bong Choi7 , Jae Hung Jung8
, Jae Hung Jung8 , Hee Jo Yang9
, Hee Jo Yang9 , KAUTII Investigators
, KAUTII Investigators 






 Cite
Cite