Abstract
-
Purpose
This study examined the epidemiological trends of bladder-related urological procedures in South Korea from 2009 to 2021.
-
Materials and Methods
The data were obtained from the Health Insurance Review and Assessment Service (HIRA) database, encompassing various bladder-related urological procedures. The frequencies and trends were analyzed using statistical methods.
-
Results
Uroflowmetry, cystoscopy, prostate biopsy, and urethral dilation showed a positive trend, while prostate massage exhibited a negative trend. The 72-hour voiding function test, which started in 2017, also demonstrated a positive trend in frequency. A urodynamic study and mid-urethral sling operation exhibited an overall decreasing trend. Bladder-indwelling catheter, Nelaton catheterization, and cystostomy catheter change showed increasing trends, while suprapubic cystostomy showed a decreasing trend.
-
Conclusions
This 12-year analysis provided valuable insights into the epidemiological patterns and utilization of bladder-related urological procedures in South Korea. These trends highlight the evolving landscape of diagnostic and therapeutic approaches in bladder-related conditions and the importance of interdisciplinary collaboration between urology and other medical departments. The results highlight the need for optimizing catheter-related care protocols, resource allocation, and continued monitoring of practices across healthcare settings.
-
Keywords: Urinary bladder diseases, Catheters, indwelling, Urinary catheteri-zation, Cystoscopy, Urodynamics
INTRODUCTION
The growing number of elderly individuals in society has led to an increase in age-related health conditions. Among these, urological disorders related to the urinary system have become a significant concern. Such disorders can substan-tially impact the quality of life for affected individuals, necessitating medical attention. Like many other countries, the population of South Korea is aging. A super-aged society is characterized by a high proportion of individuals aged 65 and above in the overall population due primarily to increased life expectancy and decreased fertility rates [
1]. The rising prevalence of urinary disorders among the elderly population has several implications. First, it places an increasing burden on the healthcare system regarding the diagnosis, treatment, and management of these conditions. Healthcare providers need to be equipped with the necessary knowledge and skills to address the specific needs of these patients. Furthermore, the growing number of patients with bladder anatomical and functional diseases requires more procedures and examinations related to these conditions. Diagnostic tests, such as cystoscopy, urodynamic studies, and imaging techniques, can assess the bladder function and identify any underlying anatomical abnormalities. The treatment options range from medication and lifestyle modifications to surgical interventions, depending on the severity and nature of the condition.
Understanding the trends and patterns of bladder-related urological procedures is essential for healthcare providers, policymakers, and researchers to optimize patient care, resource allocation, and the development of evidence-based guidelines. Transurethral surgeries and procedures that utilize the natural urethral orifice and are considered a specialized area of urology have evolved significantly with advances in technology and instruments. A rapid change in these procedures in the past eight years was recently reported [
2,
3]. Transurethral surgeries and procedures are popular for urologists and are easily performed in hospitals and clinics [
4]. In urology outpatient clinics, a wide range of bladder-related tests and procedures are performed to diagnose and treat urological diseases. Among these, cystoscopy, urodynamic studies, and uroflowmetry are indispensable diagnostic tools. Furthermore, bladder catheterizations are essential procedures carried out routinely in urology outpatient clinics. This study examined the recent epidemiologic trends in bladder-related urological procedures from 2009 to 2021 in Korea using the entire population-based cohort.
MATERIALS AND METHODS
1. Data Collection
This study is a cross-sectional epidemiological study of a Korean population using the Health Insurance Review and Assessment Service (HIRA) database from 2009 to 2021.
The ethics statement of this study was carried out in accordance with good clinical practice guidelines and the Declaration of Helsinki. The data were anonymized and analyzed. The Institutional Review Board of Hallym University Dongtan Sacred Heart Hospital approved this study (HRT 2023-06-003).
The medical service claims data of bladder-related urological procedures submitted by medical service providers during the same period were presented. The HIRA monitors and analyzes the reimbursement records from the Korean National Health Insurance and Korean Medical Aid. The HIRA records cover most Korean citizens (approximately 50 million people) because Koreans are required to join the National Health Insurance (approximately 96.3% of the population) or the Korean Medical Aid (approximately 3.7%) [
5]. The HIRA database contains information on an individual beneficiary and healthcare service information, such as diagnosis, procedures, prescriptions, and tests. All clinics and hospitals submit claims data for inpatient and outpatient care, including diagnoses, procedures, prescription records, demographic information, and direct medical costs, to the HIRA to obtain reimbursement for the medical costs from the government. The HIRA database was established based on the Korean Standard Classification of Diseases-6th revision (KCD-6), which is a modified version of the International Statistical Classification of Diseases and Related Health Problems 10th revision for the Korean healthcare system [
6]. The bladder-related urological procedures included the following: cystoscopy (E7730 and E7750), uroflowmetry (EY521-2), prostate massage (R3980), prostate biopsy (C8551), urethral dilation (R3641), 72-hour voiding function test (E6530), urethral catheterization (M0050), bladder-indwelling catheter (M0060), suprapubic cystostomy (R3576), change in cystostomy (R3577), urodynamic study (UDS; E6563-4), and mid-urethral sling operation for stress urinary incontinence (R3565).
Linear regression analyses were conducted using IBM SPSS Statistics 24.0 (IBM Co.) and Microsoft Excel 2010 (Microsoft). The Durbin–Watson method was used to evaluate the independence of residuals. All tests were two-sided with a statistical significance set to p<0.05.
RESULTS
1. Urological Outpatient Procedures from 2009 to 2021
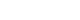
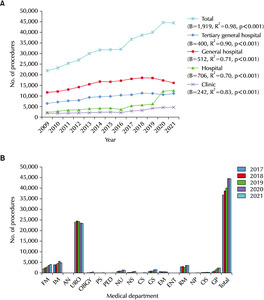
The procedures showed an increasing frequency included uroflowmetry (B=69,408, R
2=0.98, p<0.001), cystoscopy (B=7,823, R
2=0.96, and p<0.001), prostate biopsy (B=1,690, R
2=0.85, and p<0.001), urethral dilation (B=918, R
2=0.89, and p<0.001), and the 72-hour voiding function test started from 2017 (B=14,815, R
2=0.98, and p=0.001). On the other hand, prostate massage (B=-11,584, R
2=0.87, and p<0.001) showed a significant decreasing trend in frequency (
Fig. 1).
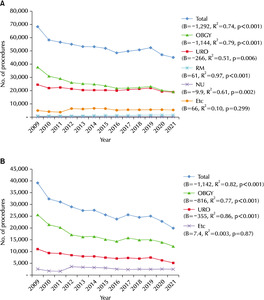
The analysis revealed a statistically significant decrease in the overall frequency of urodynamic examinations (B=-1,292, R
2=0.74, and p<0.001). Among the medical departments, obstetrics and gynecology had the highest frequency (B=-1,144, R
2=0.79, and p<0.001), followed by urology (B=-266, R
2=0.51, and p=0.006), both of which exhibited a declining trend. Rehabilitation medicine (B=61, R
2=0.97, and p<0.001), neurology (B=-9.9, R
2=0.61, p=0.002), and other departments (B=66, R
2=0.10, p=0.299) also conducted urodynamic studies, albeit at lower frequencies. The frequency of urodynamic studies in rehabilitation medicine showed an increasing trend (
Fig. 2A).
From 2009 to 2021, linear regression analysis revealed a statistically significant decreasing trend in the overall frequency of mid-urethral sling surgery (B=-1,142, R
2=0.82, and p<0.001). Among the medical specialties, obstetrics and gynecology had the highest frequency (B=-816, R
2=0.77, and p<0.001), followed by urology (B=-355, R
2=0.86, and p<0.001), both of which exhibited a declining trend in frequency. On the other hand, the frequency of mid-urethral sling surgery performed by other specialties (B=7.4, R
2=0.003, and p=0.87) was relatively low, and static trends were observed over all times (
Fig. 2B).
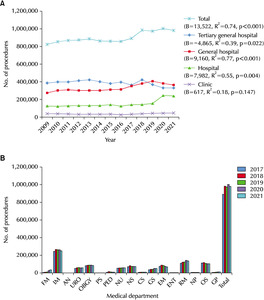
From 2009 to 2021, a linear regression analysis was conducted to examine the total frequency trend of bladder-indwelling catheter usage. The analysis revealed a statistically significant increasing trend (B=54,155, R
2=0.72, and p<0.001). Considering the different hospital classes, tertiary general hospitals, general hospitals, and hospitals demonstrated a statistically significant increasing trend in bladder-indwelling catheter usage. Among them, general hospitals had the highest frequency (B=25,128, R
2=0.81, and p<0.001), followed by tertiary general hospitals (B=12,242, R
2=0.82, and p<0.001), hospitals (B=15,550, R
2=0.55, and p=0.004). In contrast, clinics exhibited an overall static trend (B=-869, R
2=0.03, and p=0.596), but this trend was not significant (
Fig. 3A). In 2021, the top seven departments ranked by total frequency were as follows: 1. Internal medicine, 489,076 cases; 2. Orthopedic surgery, 281,589 cases; 3. Neurosurgery, 210,838 cases; 4. General surgery, 186,922 cases; 5. Urology, 172,042 cases; 6. Obstetrics and gynecology, 127,954 cases; 7. Emergency medicine, 73,997 cases (
Fig. 3B).
An analysis of the Nelaton catheterization frequency from 2009 to 2021 using linear regression revealed a statistically significant increasing trend (B=13,522, R
2=0.74, and p< 0.001). When considering different hospital classes, tertiary general hospitals were initially the most frequent (B=-4,865, R
2=0.39, and p=0.022). On the other hand, general hospitals (B=9,160, R
2=0.77, and p<0.001) surpassed them as the most frequent category and maintained the highest frequency since 2019. Hospitals (B=7,982, R
2=0.55, and p=0.004) ranked third in frequency, followed by clinics (B=617, R
2=0.18, and p=0.147). Both general hospitals and hospitals exhibited a significant increasing trend, while tertiary general hospitals showed a significant decreasing trend. Although the clinics showed an increasing trend, it did not reach statistical significance (
Fig. 4A). In 2021, the top seven departments ranked by frequency are as follows: 1. Internal medicine, 251,592 cases; 2. Rehabilitation medicine, 138,040 cases; 3. Orthopedic surgery, 104,169 cases; 4. Obstetrics and gynecology, 86,322 cases; 5. Neurosurgery, 73,491 cases; 6. Emergency medicine, 69,064 cases; 7. Urology, 60,448 cases (
Fig. 4B).
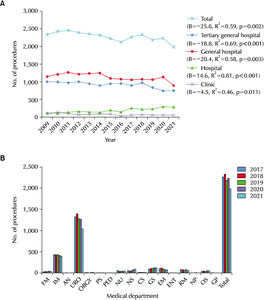
An analysis of the suprapubic cystostomy frequency using linear regression from 2009 to 2021 revealed a statistically significant decreasing trend (B=-25.8, R
2=0.59, and p=0.002). When considering the different hospital classes, general hospitals were the most frequent (B=-20.4, R
2=0.58, and p=0.003), followed by tertiary general hospitals (B=-18.8, R
2=0.69, and p<0.001), and hospitals (B=14.6, R
2=0.81, and p<0.001) ranked third in terms of frequency for the overall time. Clinics (B=-4.5, R
2=0.46, and p=0.011) represented the fourth highest frequency. Hospitals exhibited a significant increasing trend in the suprapubic cystostomy frequency. In contrast, significant decreasing trends were observed in tertiary general hospitals, general hospitals, and clinics (
Fig. 5A). In 2021, the top seven departments ranked by frequency were as follows: 1. Urology, 1,041 cases; 2. Internal medicine, 398 cases; 3. General surgery, 118 cases; 4. Neurosurgery, 91 cases; 5. Emergency Medicine, 75 cases; 6. Rehabilitation medicine, 66 cases; 7. Orthopedic surgery, 51 cases (
Fig. 5B).
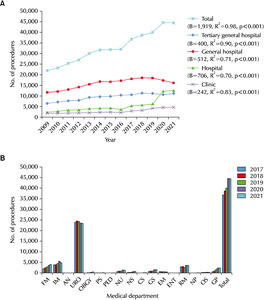
Linear regression analysis indicated a statistically significant increasing trend in the frequency of cystostomy catheter changes from 2009 to 2021 (B=1,919, R
2=0.98, and p<0.001). During the study period, the increase in the change in cystostomy was higher in the hospital than in other hospital classes. When considering different hospital classes for the overall time, general hospitals had the highest frequency (B=512, R
2=0.71, and p<0.001), followed by tertiary general hospitals (B=400, R
2=0.90, and p<0.001). Hospitals ranked third in terms of frequency (B=706, R
2=0.70, and p<0.001), while clinics represented the fourth highest frequency (B=242, R
2=0.83, and p<0.001). All hospital classes showed significant increases in the frequency of cystostomy catheter changes. On the other hand, the shift in frequency between tertiary general hospitals and hospitals was particularly noteworthy from 2020 to 2021 (
Fig. 6A). In 2021, the top seven departments in terms of frequency were as follows: 1. Urology, 23,428 cases; 2. Internal medicine, 4,834 cases; 3. Family medicine, 4,138 cases; 4. Rehabilitation medicine, 3,627 cases; 5. General practitioner, 2,453 cases; 6. General surgery, 1,695 cases; 7. Neurology, 1,318 cases (
Fig. 6B).
DISCUSSION
Bladder-related urological conditions encompass a broad spectrum of disorders that significantly affect the quality of life for individuals. The use of a temporary or permanent catheter may be necessary when individuals experience urination disorders, such as prostatic hyperplasia or neurogenic bladder, and face difficulties in mobility due to aging, chronic diseases, operations, or falls. Understanding the trends and patterns of bladder-related urological procedures is crucial for healthcare providers, policymakers, and researchers to optimize patient care, resource allocation, and the development of evidence-based guidelines.
The findings of this nationwide population-based cohort study provide valuable insights into the trends in bladder-related urological procedures in South Korea from 2009 to 2021. This study identified increasing and decreasing trends in various procedures, highlighting the changing landscape of urological care in South Korea.
Uroflowmetry is a non-invasive test that measures the urine flow rate, providing valuable information on the bladder function. Cystoscopy, however, is an invasive procedure that allows direct visualization of the bladder and urethra, aiding in the diagnosis and treatment of various urologic conditions. The increasing frequency of these procedures suggests a growing recognition of the importance of assessing bladder function and diagnosing bladder-related disorders in clinical practice. A prostate biopsy and urethral dilation also showed an increasing trend in frequency. A prostate biopsy is performed to diagnose prostate cancer, while urethral dilation treats urethral strictures. The 72-hour voiding function test, which was introduced and became eligible for national health insurance coverage in 2017, is essential for assessing the bladder function and showed a significant increase in frequency. The rising frequency of these procedures reflects the growing demand for urological evaluation and management, which was likely driven by the increasing prevalence of urological disorders, particularly among the elderly population. In contrast, prostate massage showed a significant decreasing trend in frequency. Prostate massage is a diagnostic procedure for obtaining prostatic secretions for laboratory analysis. The decline in its frequency may be due to advances in diagnostic techniques and the availability of more accurate and non-invasive diagnostic tests.
The study also examined the frequency of urodynamic studies and mid-urethral sling operations, which showed decreasing trends. Urodynamic studies assess the bladder and urethral function and are commonly used to evaluate urinary incontinence and other bladder-related disorders. Mid-urethral sling operations are surgical procedures to treat stress urinary incontinence in women. In South Korea, a urodynamic study must be conducted in advance to perform a mid-urethral sling operation. Hence, a urodynamic study is decreasing in line with the trend of decreasing mid-urethral sling operations in obstetrics, gynecology, and urology because of population decline and a low birth rate. The urodynamic study has declined less than that in obstetrics and gynecology because the urology department specializes in bladder function and preoperative urinary incontinence evaluations. Obstetrics and gynecology have the highest frequency of urodynamic study, followed by urology because more mid-urethral slings are performed in obstetrics and gynecology than in urology. Rehabilitation medicine showed an increasing trend in the frequency of urodynamic studies, suggesting an expanding the role in managing bladder dysfunction in patients with neurological or musculoskeletal conditions.
The bladder-indwelling catheter is a commonly used medical device that has been subject to very few design modifications since its intervention [
7]. Up to 25% of patients in UK stay hospitals will undergo urethral catheterization for various indications during their inpatient stay, and up to 13% of nursing home patients have long-term urinary catheters [
8]. The indwelling urinary catheter is the most common cause of infections in hospitals and other healthcare facilities [
9].
Urinary tract infections (UTIs) account for approximately 20% of hospital-acquired (nosocomial) infections [
10], and approximately 80% of these are associated with urinary catheters. Such infections prolong hospital stay, are expensive to treat [
11], and cause unpleasant symptoms, such as fever and chills in up to 30% of the patients. Approximately 17% of hospital bacteremia is due to catheter-associated UTI [
12]. The indications for indwelling urethral catheterization include acute urinary retention or bladder outlet obstruction, the need for precise urinary output monitoring, and in patients undergoing urological or gynecological surgery who might be unable to micturate immediately after surgery [
12].
Bladder-indwelling catheter usage has increased signi-ficantly across different hospital classes, with general hospitals having the highest frequency. The increasing frequency of bladder-indwelling catheter usage suggests a growing need for urinary management in clinical practice. In 2021, the frequency of bladder-indwelling catheter use was high in internal medicine, orthopedic surgery, neurosurgery, general surgery, and urology. Interdisciplinary cooperation is valued as an area where urology expertise can greatly help manage patients requiring long-term bladder catheterization.
The analysis of Nelaton catheterizations revealed an increasing trend in frequency over the study period. Nelaton catheterization is also a method of bladder catheterization commonly used in clinical practice. The increasing frequency of Nelaton catheterization may be attributed to factors, such as an aging population and an increased awareness of the importance of urinary management.
Suprapubic cystostomy demonstrated a significant de-crease in frequency. The frequency of this procedure was highest in general hospitals, followed by tertiary general hospitals, hospitals, and clinics. Despite the rising trend of bladder-related procedures due to the growing elderly population, suprapubic cystostomy has consistently declined in general hospitals, tertiary general hospitals, and clinics from 2009 to 2021. This decline can be attributed to the cumulative impact of the urology residency shortage spanning from 2009 to 2021, resulting in a shortage of urologists [
13].
The frequency of cystostomy catheter changes showed a significant increasing trend, with general hospitals and tertiary general hospitals having the highest frequencies. This increase may be associated with the rising number of patients with long-term bladder catheterization who require regular catheter changes to prevent complications.
Coronavirus disease 2019 (COVID-19) was prevalent during 2020 and 2021. At this time, the COVID-19 epidemic greatly impacted medical care. On the other hand, it did not appear to affect the annual flow of bladder-related urological procedures. This essential medical area is not greatly affected by external factors.
These findings provide important insights into the chang-ing landscape of bladder-related urological procedures in South Korea. The trends observed in this study can help healthcare providers, policymakers, and researchers optimize patient care and allocate resources.
CONCLUSIONS
This study analyzed the epidemiological trends of bladder-related urological procedures in South Korea from 2009 to 2021. The findings indicate increasing frequencies of uroflowmetry, cystoscopy, prostate biopsy, urethral dilation, and 72-hour voiding function test. On the other hand, prostate massage demonstrated a significant decrea-sing trend. Urodynamic studies and mid-urethral sling operations exhibited an overall decreasing trend. Bla-dder-indwelling catheter, Nelaton catheterization, and cystostomy catheter change also demonstrated an increasing trend. Suprapubic cystostomy exhibited a decreasing trend. These trends highlight the evolving landscape of a diagnostic and therapeutic approach in bladder-related conditions and the importance of interdisciplinary collaboration between urology and other medical departments. The results highlight the need to optimize catheter-related care protocols, resource allocation, and continued monitoring of practices across healthcare settings. This information can inform healthcare providers, policymakers, and researchers in optimizing patient care, resource allocation, and identifying areas for further investigation and improvement in managing bladder-related urological conditions.
FUNDING
No funding to declare.
NOTES
-
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
-
AUTHOR CONTRIBUTIONS
J.H.H. conceived and designed the research, overseeing its progress. Data was gathered by H.K., W.Y., S.P., and H.L. Statistical analysis was performed by J.K.K. and H.K. They, along with J.H.H., interpreted the data. H.K. and J.H.H. drafted the manuscript, which J.K.K. critically reviewed. J.K.K. provided administrative and technical support, while J.H.H. supervised the project and granted final manuscript approval. All authors read and approved the final manuscript.
Fig. 1Urological outpatient procedures from 2009 to 2021 in a Korean popula-tion.
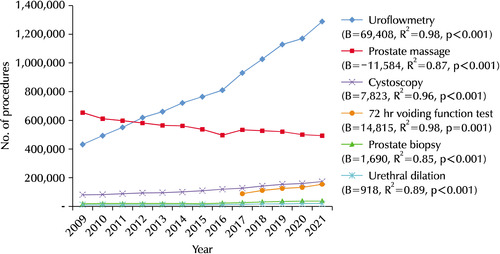
Fig. 2Urodynamic study (A) and mid- ure-thral sling operation (B) according to the medical department from 2009 to 2021 in a Korean population. OBGY: obstetrics & gynecology, URO: urology, RM: rehabilitation medicine, NU: ne-urology.
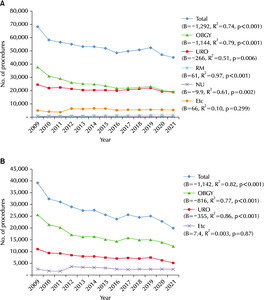
Fig. 3Frequency of bladder-indwelling catheters according to the hospital classes in the Korean population from 2009 to 2021 (A) and according to the medical department from 2017 to 2021 (B). FM: family medicine, IM: internal medicine, AN: anesthesiology, URO: uro-logy, OBGY: obstetrics & gynecology, PS: plastic surgery, PED: pediatrics, NU: neurology, NS: neurosurgery, CS: chest surgery, GS: general surgery, EM: emergency medicine, ENT: ear, nose, and throat, RM: rehabilitation medicine, NP: neuropsychiatry, OS: orthopedic sur-gery, GP: general practitioner.
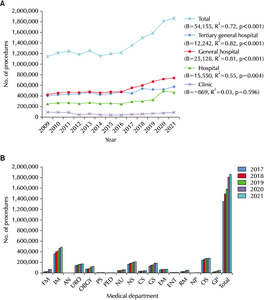
Fig. 4Frequency of Nelaton cathete-rization according to the hospital classes in the Korean population from 2009 to 2021 (A) and according to the medical department from 2017 to 2021 (B). FM: family medicine, IM: internal medicine, AN: anesthesiology, URO: urology, OBGY: obstetrics & gynecology, PS: plastic surgery, PED: pediatrics, NU: neurology, NS: neurosurgery, CS: chest surgery, GS: general surgery, EM: emer-gency medicine, ENT: ear, nose, and throat, RM: rehabilitation medicine, NP: neuropsychiatry, OS: orthopedic sur-gery, GP: general practitioner.
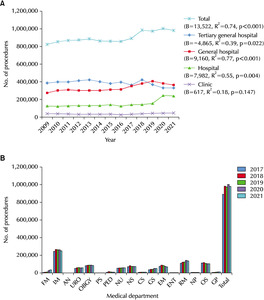
Fig. 5Frequency of suprapubic cysto-stomy according to the hospital classes in the Korean population from 2009 to 2021 (A) and according to the medical department from 2017 to 2021 (B). FM: family medicine, IM: internal medicine, AN: anesthesiology, URO: urology, OBGY: obstetrics & gynecology, PS: plastic surgery, PED: pediatrics, NU: neurology, NS: neurosurgery, CS: chest surgery, GS: general surgery, EM: emer-gency medicine, ENT: ear, nose, and throat, RM: rehabilitation medicine, NP: neuropsychiatry, OS: orthopedic sur-gery, GP: general practitioner.
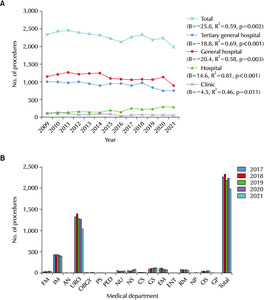
Fig. 6Frequency of cystostomy catheter changes according to the hospital classes in the Korean population from 2009 to 2021 (A) and according to the medical department from 2017 to 2021 (B). FM: family medicine, IM: internal medicine, AN: anesthesiology, URO: urology, OBGY: obstetrics & gynecology, PS: plastic surgery, PED: pediatrics, NU: neurology, NS: neurosurgery, CS: chest surgery, GS: general surgery, EM: emergency medicine, ENT: ear, nose, and throat, RM: rehabilitation medicine, NP: neuropsychiatry, OS: orthopedic sur-gery, GP: general practitioner.
REFERENCES
- 1. Kim KW, Kim OS. Super aging in South Korea unstoppable but mitigatable: a sub-national scale population projection for best policy planning. Spat Demogr 2020;8:155-73. ArticlePubMedPMCPDF
- 2. Kim JK, Cho YS, Park SY, Joo KJ, Min SK, Lee YG, et al. Recent surgical treatments for urinary stone disease in a Korean population: national population-based study. Int J Urol 2019;26:558-64. ArticlePubMedPDF
- 3. Kim JK, Choi C, Kim US, Kwon H, Lee SH, Lee YG, et al. Recent trends in transurethral surgeries and urological outpatient procedures: a nationwide population-based cohort study. J Korean Med Sci 2020;35:e315. ArticlePubMedPMCPDF
- 4. Jeon BJ, Chung H, Bae JH, Jung H, Lee JG, Choi H. Analysis of present status for surgery of benign prostatic hyperplasia in Korea using nationwide healthcare system data. Int Neurourol J 2019;23:22-9. ArticlePubMedPMCPDF
- 5. Park J, Lee YJ, Lee JW, Yoo TK, Chung JI, Yun SJ, et al. Comparative analysis of benign prostatic hyperplasia management by urologists and nonurologists: a Korean nationwide health insurance database study. Korean J Urol 2015;56:233-9. ArticlePubMedPMC
- 6. Kim JA, Yoon S, Kim LY, Kim DS. Towards actualizing the value potential of Korea Health Insurance Review and Assessment (HIRA) data as a resource for health research: strengths, limitations, applications, and strategies for optimal use of HIRA data. J Korean Med Sci 2017;32:718-28. ArticlePubMedPMCPDF
- 7. Feneley RC, Hopley IB, Wells PN. Urinary catheters: history, current status, adverse events and research agenda. J Med Eng Technol 2015;39:459-70; Erratum. ArticlePubMedPMC
- 8. Loveday HP, Wilson JA, Pratt RJ, Golsorkhi M, Tingle A, Bak A, et al. Epic3: national evidence-based guidelines for preventing healthcare-associated infections in NHS hospitals in England. J Hosp Infect 2014;86 Suppl 1:S1-70. ArticlePubMed
- 9. Hooton TM, Bradley SF, Cardenas DD, Colgan R, Geerlings SE, Rice JC, et al. 2009;; Infectious Diseases Society of America.
- 10. Smyth ET, McIlvenny G, Enstone JE, Emmerson AM, Humphreys H, Fitzpatrick F, et al. ; Hospital Infection Society Prevalence Survey Steering Group. Four country healthcare associated infection prevalence survey 2006: overview.
- 11. Nasr A. State of the globe: catheterizations continue to cultivate urinary infections. J Glob Infect Dis 2010;2:81-2. ArticlePubMedPMC
- 12. Gould CV, Umscheid CA, Agarwal RK, Kuntz G. Pegues DA; Healthcare Infection Control Practices Advisory Committee. Guideline for prevention of catheter-associated urinary tract infections 2009. Infect Control Hosp Epidemiol 2010;31:319-26. ArticlePubMed
- 13. Han JH, Min SK, Lee YG. Application rate for urology majors and appropriateness of urology medical expenses. Korean J Insur Med 2014;9:5-14.
 , Wonjong Yang
, Wonjong Yang , Sangyong Park
, Sangyong Park , Heesub Lee
, Heesub Lee , Jong Keun Kim
, Jong Keun Kim , Jun Hyun Han,
, Jun Hyun Han,

 , Department of Urology, Hallym University Dongtan Sacred Heart Hospital, 7, Keunjaebong-gil, Hwaseong 18450, Korea, Tel: +82-31-8086-2730, Fax: +82-31-8086-2728, E-mail: junuro@naver.com
, Department of Urology, Hallym University Dongtan Sacred Heart Hospital, 7, Keunjaebong-gil, Hwaseong 18450, Korea, Tel: +82-31-8086-2730, Fax: +82-31-8086-2728, E-mail: junuro@naver.com 







 KAUTII
KAUTII

 ePub Link
ePub Link Cite
Cite