Articles
- Page Path
- HOME > Urogenit Tract Infect > Volume 18(2); 2023 > Article
- Review Is Human Mpox a New Sexually Transmitted Infection in Korea That Should Be Monitored?
-
Gilho Lee,

-
Urogenital Tract Infection 2023;18(2):35-44.
DOI: https://doi.org/10.14777/uti.2023.18.2.35
Published online: August 31, 2023
Department of Urology, Dankook University College of Medicine, Cheonan, Korea
-
Correspondence to: Gilho Lee,
 , Department of Urology, Dankook University College of Medicine, 119 Dandae-ro, Dongnam-gu, Cheonan 31116, Korea, Tel: +82-41-550-6630, Fax: +82-41-550-3905, E-mail: multiorigins@yahoo.com
, Department of Urology, Dankook University College of Medicine, 119 Dandae-ro, Dongnam-gu, Cheonan 31116, Korea, Tel: +82-41-550-6630, Fax: +82-41-550-3905, E-mail: multiorigins@yahoo.com
• Received: April 21, 2023 • Revised: May 6, 2023 • Accepted: May 7, 2023
Copyright © 2023, Korean Association of Urogenital Tract Infection and Inflammation. All rights reserved.
This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 526 Views
- 2 Download
Abstract
- Human monkeypox (mpox) outbreaks have been reported in more than 110 countries, with more than 86,930 confirmed cases. The World Health Organization has realized the seriousness of personal transmission and has declared a global health emergency against the infection. Traditionally, contact with infected animals in a few endemic countries has been a major transmission route of the mpox virus. On the other hand, the global mpox outbreak in 2022 has been primarily associated with sexual networks of men who have sex with men (MSM) and bisexual men exhibiting high-risk behaviors. Their common symptoms are initial fever, headache, swollen lymph nodes, and subsequent skin rashes. These presentations did not consistently occur in the 2022 outbreak. Many patients presented with skin lesions on the anogenital areas without prodromal symptoms. In addition, the atypical characteristics of the recent outbreak may result in a misdiagnosis of other skin lesions, such as chickenpox. Furthermore, infected persons are frequently co-infected with sexually transmitted infections (STIs) with similar skin lesions. The newly confirmed cases in Korea on April 2023 must have been infected through community transmission because these new patients had not traveled overseas in the past three months. Therefore, mpox is something that everybody should be concerned about in Korea. Medical practitioners must know the characteristics of the infection because patients with mpox may visit their offices with some genital lesions or other STIs. The clinical information from this paper may broaden and deepen the understanding of human mpox and curb the early transmission of the infection.
INTRODUCTION
Monkeypox (mpox) is a rare zoonotic contagious disease caused by the mpox virus (MPXV) [1]. The disease was nicknamed mpox because the MPXV was initially discovered in monkeys [2]. Although mpox was initially regarded as an animal infectious disease, the MPXV has revealed wide species tropism [3].
Several mpox outbreaks have occurred worldwide [4-7]. The earlier endemic outbreaks as a zoonotic disease occurred in some endemic African countries, such as the Democratic Republic of Congo (DRC) [8] and the Republic of the Congo (ROC) [9], and in the United States of America following contacts of MPXV-infected animals from the endemic foreign countries [7]. On September 2017, however, the first suspected case of human-to-human transmitted mpox was reported in Nigeria [9]. Between 2018 and 2019, two men who recently traveled to the UK from Nigeria [10], one man in Israel who also traveled from Nigeria [11], and one Nigerian man in Singapore [12] were diagnosed with human mpox. The four infected men might cross the boundary of the endemic areas. On May 2022, human mpox was abruptly reported across Europe in men who had not recently traveled into the endemic countries and were not exposed to infected animals. The number of infected cases has grown to more than 86,930 persons in mid-April 2023 across 110 countries (Supplementary Table 1) [13].
The rapid increase in mpox-infected cases reported in non-endemic areas suggests personal transmission without links to animal sources. Indeed, this current outbreak has occurred among men who have sex with men (MSM), and the major transmission route may be sexual intercourse [6,14-20]. Although the outbreak has been found primarily in MSM and bisexual men with high-risk behaviors, some heterosexual casual sex partners can also be infected through bisexual men [17].
The classic pathogenesis of mpox is composed of four stages: incubation, prodromal, skin eruption, and healing stages [5,21,22]. Clinical manifestations of mpox are inconsistent among the outbreaks; more severe or critical symptoms were reported in earlier outbreaks in DRC or ROC, whereas less severe or mild clinical manifestations were reported in cases of the recent global outbreak [5,21,22]. Moreover, some recently infected cases have not revealed the sequential four stages in skin lesions, and their skin lesions occurred primarily in the genital and perianal sites [5,6,14,15]. The divergent clinical courses or manifestations between two types of infection may come from different modes of transmission, skin color of the affected persons, accessible medical care systems among counties, different genetic characteristics of the MPXV, and prevalence of prior smallpox vaccination [21,22].
With the international interventions for curbing the transmission of the infection after the first notification in 2022, the incidence of new infections has just passed the peak [13]. On the other hand, phylogenetic epidemiologic studies suggest that the recent outbreak worldwide can be controlled with appropriate interventions, but the infection cannot be eradicated. MPXV may hide in unexposed social networks and survive within the connections. Indeed, of the ten total mpox infections reported thus far in Korea, five were locally transmitted mpox cases. The Korea Disease Control and Prevention Agency (KDCA) concluded that the cases resulted from community transmission, as these new patients had not traveled overseas in the past three months. In the past, human mpox was treated as a regional crisis in some endemic counties [4,7-9]. On the other hand, the recent outbreak mostly affected MSMs and bisexual men exhibiting high-risk behaviors. Mpox is not a gay disease anymore; the MPXV can be transmitted to anyone. Therefore, everybody should be concerned about viral zoonotic diseases [6].
Although national guidelines against human mpox should be updated as rapidly as possible, national authorities must circulate the new infection information to medical practitioners. On the other hand, in reality, this is not the case. Therefore, medical specialists must know the characteristics of the infection because patients with this contagious disease may visit their offices with some genital lesions or other sexually transmitted infections (STIs). Unrecognized or late-diagnosed infections may spread the infection to practitioners and their society. Spreading the MPXV can be overcome by knowledge-sharing and improved awareness among the population and healthcare providers. The clinical information from this paper may broaden and deepen the understanding of human mpox to curb early transmission and control the infection in the near future.
MAIN BODY
The genome of MPXV is composed of double-stranded DNA and belongs to the family of Poxviridae [23]. Under evolutional pressure, the genomes of MPXV are mutated less frequently than those of RNA viruses, such as coronavirus. The genetic information of MPXV has approximately 200,000-250,000 bp and 170-210 protein-coding genes [24].
The reported MPXV genomes can be classified phylo-genetically into three clades: two old clades (A.1 and A.2) from the earlier outbreaks and a newly emerging clade from the global outbreak in 2022 (B.1) [25,26]. The epidemiological features in genomes between clades A and B are different (Fig. 1) [25,26]. The DRC clade (A.1) and ROC clade (A.2) caused endemic diseases in sporadic outbreaks in many parts of Central and West Africa and the United States of America. In contrast to the earlier strains, the MPXV strains (clade B.1) in the 2022 outbreak are tightly clustered together by phylogenetic analysis (Fig. 1) [25]. The genetically tight clustering suggests that the outbreak in 2022 may have originated from one hidden source. In particular, the MPXV sequence of ON676708 (USA_2021_MD) from a case who traveled from Nigeria to the United States in 2021 was placed phylogenetically between the sequences of strains in 2018-2019 and 2022 (Fig. 1) and the MPXV case of ON676707 (USA_2021_TX) was genetically identical to that of ON674051 (USA_2022_FL) and ON675438 (USA_2022_VA). These three DNA sequences between 2021 and 2022 have a genetic linkage with a large outbreak that occurred in Nigeria in 2017-2018 and the export of the MPXV in 2018 and 2019 from Nigeria to the United Kingdom, Israel, and Singapore (Fig. 1) [10-12,25]. Therefore, the emergence of the 2022 outbreak may have resulted from the importation of this MPXV from one hidden source that potentially emerged from the continuously cryptic circulation of the same virus that caused the 2017-2018 outbreak in Nigeria. Finally, the virus was introduced into an unknown MSM community exhibiting high-risk behavior and has continued circulating within the core community and exported into European countries in 2022 (Fig. 2).
These phylogenetic epidemiologic studies may suggest that although the recent outbreak could be controlled with appropriate interventions, the infection could not be eradicated. MPXV may hide in unexposed social networks, waiting for a ripe opportunity (Fig. 2).
The clinical features between the two clades are also different [6,7,15,21,22,27]. The overall mortality rate of human mpox infection was 8.7% of infected cases, with a significant difference between the Central African clade (10.6%) and the West African clade (3.6%) [1,27]. In addition, the reproduction number R0 for the Central African type was estimated to be 0.6-1.0 [1,28,29], and the R0 for the Western type may be lower than that of the central clade. R0>1 indicates that the pathogen has an epidemic potential in society [28,30]. In contrast, the lower R0 in the recent outbreak means an unlikely expanding personal trans-mission of mpox in an anonymous society and a lower possibility of inter-familial transmission [27-31].
MPXV is a member of the human orthopoxvirus family, along with variola, cowpox, and vaccinia viruses [23]. MPXV is genetically similar to smallpox by the variola virus, but has milder skin lesions and a lower mortality [32]. Therefore, one infection among orthopoxviruses may substantially protect against mpox, and vaccination with the vaccinia virus against the smallpox virus can simultaneously protect against mpox through shared immunologic mechanisms [33]. Since the vaccination for smallpox was globally suspended in 1978, individuals who lack vaccine-induced immunity have no cross-protective immunity to various orthopoxviruses [34]. Therefore, the changes in vaccination policy may induce the recent globally increased frequency of human mpox cases.
Smallpox vaccination cannot achieve 100% protection against mpox but can provide approximately 85% cross-pro-tection [6,35]. The clinical course in mpox-infected persons vaccinated against smallpox differs significantly from those in unvaccinated subjects. The symptoms and signs of mpox in vaccinated persons are milder than those of unvaccinated persons [6,35]. The incubation period of mpox is 7-21 days [22]. The Centers for Disease Control and Prevention (CDC) recommended mpox vaccination within two weeks, ideally before four days, after significant, unprotected exposure to a confirmed human case because of the relatively long incubation period. On the other hand, mpox is reported frequently in patients with acquired immune deficiency syndrome (AIDS), which may compromise the host immunity against infections [36-38]. People who are at higher potential for exposure to MPXV may be offered vaccination to help prevent mpox disease. Two vaccines may be used for the prevention of mpox disease: JYNNEOS vaccine and ACAM2000 vaccine are approved for the prevention of mpox and smallpox [39].
1) Animal-to-human transmission
MPXV has wide host tropism to propagate the virus into susceptible species [40,41]. Some primates and domesticated animals are susceptible to the MPXV (Supplementary Table 2) [3]. MPXV can be transmitted by direct contact with blood and bodily fluids of infected animals. Hunting wild animals and the cooking and consumption of infected meat or bushmeat are well-known zoonotic routes of transmission [8,22]. In addition, exposed animals with MPXV can be reservoirs for future outbreaks because of its wide species tropism. Therefore, possible spillover events to domesticated animals may be an important issue of hidden reservoirs [3].
2) Human-to-human transmission
MPXV can spread to anyone through intimate contact via skin lesions and bodily fluids from infected persons [6,22]. Contaminated touching objects and fabrics (clothing, bedding, or towels) can spread the MPXV less frequently [42]. Sexual intercourse is considered a major transmission route. The intercourse constitutes close or intimate contact, often skin-to-skin contact, and physiological responses during sexual stimulation, such as increased respiratory rates or deep respiration, prolonged face-to-face contact, kissing, touching, sweating, massage, increased secretion from genital organs that can be routes of heavily spreading the viral particles to sex partners [43,44]. Consequently, all activities during sex can be significant risk factors for spreading the MPXVs to sex partners. The current outbreak was reported mainly among MSM and can be transmitted during sexual intercourse [6,15]. This direct contact in MSMs can occur during intimate contacts, such as oral, anal, or touching the genitals of a person with mpox [45].
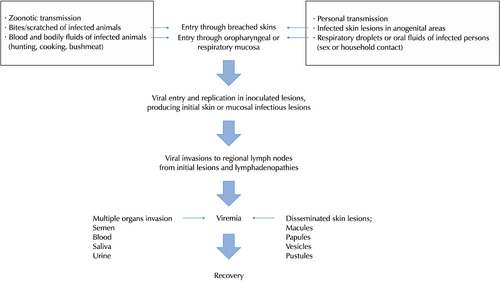
The clinical course of mpox is traditionally composed of four stages: incubation, prodromal, skin eruption, and healing stages [5,6,22,46]. MPXV can be inoculated into various lesions depending on the transmission routes. In cases of zoonotic transmission, the initial inoculated lesions must be the biting or scratching sites on human skin [7]. In cases of personal transmission via intercourse, however, initial inoculated lesions must be in the genital and anorectal areas or oral mucosa, depending on patterns of intercourse. Mpox-infected people receive a single skin lesion or multiple lesions that may be located on or near the penis, scrotum, or anus in men and the labia, vagina, or anus in women with different evolution stages of skin lesions [5,6,14,15, 19,47]. The infected lesions can evolve into perianal abscesses, incurring proctitis and ulcers in the oral cavity, incurring poor oral intake [48]. As the MPXVs in inoculated site circulate into the regional lymph nodes through nearby lymphatics, the infected person can feel painful cervical lymph node swelling or frequent inguinal lymph node swelling (Fig. 3) [5,7,22].
After incubation for 7-21 days, infected persons can present with prodromal symptoms [6,22]. The systemic symptoms through initial viremia are fever, chills, exhaustion, malaise, respiratory symptoms (e.g., sore throat, nasal congestion, or cough), headache, muscular pain, or back pain. Sometimes, people have flu-like symptoms before the rash or may experience all or only a few symptoms or no prodromal symptoms [5,6,46].
Secondary skin eruptions occurred frequently. The rash can initially look like pimples or blisters and may be painful or itchy. The rash will go through four stages (macules, papules, vesicles, and pustules) before scabbing over and desquamation on areas, such as the hands, feet, chest, face, or mouth [22,49]. A person with mpox can spread MPXVs to others from when symptoms start until the rash fully recovers. The illness typically lasts 2-4 weeks [22,45,49].
The clinical presentations differed between the outbreak in 2022 and the outbreak in 2018-2020 [1,4-6,9,35]. Divergent clinical presentations could be caused by transmission mode, the virulence of MPXV strains, the prevalence of prior smallpox vaccinations, and the initial health of the individuals. From two typical outbreaks, more severe symptoms or signs were reported in the 2018-2020 outbreak than in the 2022 outbreak. Fever as a prodromal symptom is milder or often occurs in the 2022 outbreak. Lymph node swellings were frequently found in neck or cervical lymphatics in the earlier outbreak, whereas inguinal lymphadenopathies were mainly noted in 2022. Skin lesions have been described predominantly on the limbs or face for individuals with the earlier outbreak, whereas only two-thirds of cases in the last outbreak had genital involvement. The skin lesions in 2022 are found in limited numbers with pleomorphic stages, distributed mostly in one or two anatomical sites, such as penile or perianal involvement. In contrast, the lesions in the earlier eruptions were predominantly on the face and neck, with higher numbers and monomorphisms or stage by stage in skin eruptions. Previous reports have consistently reported that the outbreak in 2022 generally showed mild illness with smaller rates of prodromal symptoms than the previous outbreak. Consequently, some patients in the recent outbreak may have a window period for surveillance because those prodromal symptoms might be mild or not even noticed at all, and some individuals may not be aware of any symptoms until the appearance of the rash. Therefore, current detailing acute symptoms for the case definition of mpox should be reviewed to adapt best to the current findings [26]. Indeed, the case definition for mpox has not been standardized worldwide.
Close physical contact during intercourse could result in an infection [5,6,43,44]. The infected persons in the 2022 outbreak involved high-risk sexual behaviors. They had approximately five sex partners in the previous three months; 20% of patients reported chemsex in the previous month, and 32% visited a sex-on-site event in the previous month [6]. Consequently, a high rate of other concurrent STIs was observed in infected patients, such as gonococcal or chlamydial infections in the pharyngeal, urethral, and rectal areas or combined lesions or concurrent STIs [5,6]. A HIV infection has more severe skin lesions associated with genital ulcers than HIV-negative individuals [9].
Differential diagnostic processes are imperative for precise diagnosis, early recognition, and public health control of mpox infections [5]. Certain patients in the 2022 outbreak revealed a single penile skin lesion mimicking chancre in primary syphilis. Herpes simplex virus can be a concomitant STI or lesion mimicking mpox [5,6]. In addition, severe chickenpox with lesions in the palms and soles can be a primary differential diagnosis in mpox infections [50]. The lesions in chickenpox are more superficial and occur in clusters of the same stage, with denser manifestations on the trunk than on the face and extremities [50]. The symptoms and signs of the 2022 outbreak were nonspecific. Therefore, other varieties of differential diagnoses should be considered, ranging from chickenpox, molluscum contagiosum, measles, rickettsial infections, bacterial skin infections (such as those caused by Staphylococcus aureus), anthrax, scabies, syphilis, and drug reactions with other noninfectious causes of rash [9]. Ogoina et al. [9] reported that their hospital reported false alarms for mpox during the outbreak. These skin lesions include chicken pox, mosquito bites, molluscum conta-giosum, impetigo, facial acne, tinea corporis, psoriasis, scabies, and petechiae rash in a patient with a bleeding disorder.
MPXV revealed various tissue tropisms [19,27,48,51]. Optimal clinical specimens for laboratory analyses depend on the disease stages or infectious routes. Four typical skin lesions are used frequently because the skin lesions occur frequently, can be harvested easily, and have high viral loads in the lesions (Fig. 4). In addition to the skin lesions, MPXV DNA was detected in the saliva or oral mucosal swab, rectal swab, nasopharyngeal swab, semen, urine, and feces [19,48]. The viral loads from various samples depend on the infec-tious routes and disease stages [51]. Interestingly, MPXVs are consistently isolated in semen during the pathogenesis of a mpox infection [51]. Although pathogenicity by semen or vaginal fluids has not yet been established, the presence in secretions can support the potential for sexual transmission [18,19]. Therefore, The UK Health Security Agency (UKHSA) guidelines have advised condom use for eight weeks after infection, but the potential duration and infectiousness of viral shedding in semen requires further study [6].
A variety of methods have been developed for mpox infections. Nucleic acid detection of the MPXV by real-time PCR (RT-PCR) is the preferred method for routine diagnosis [6,52]. This amplification test is conducted in a biosafety level-three facility [53]. The genetically conserved areas for amplification contain the extracellular-envelope protein gene (B6R) [52], DNA polymerase gene, E9L [54], DNA-depen-dent RNA polymerase subunit 18, rpo18 [55], and F3L gene [56]. The restriction length fragment polymorphism (RFLP) of PCR-amplified genes or gene fragments is also used to detect MPXV DNA [57], but RFLP is time-consuming and requires a virus culture. Whole-genome sequencing, using next-generation sequencing technologies, remains the gold standard for the diagnosis and genetic characterization of MPXV [25]. Enzyme-linked immunosorbent assay (ELISA) can detect the MPXV IgM and IgG antibodies in the serum [58]. On the other hand, the specificity is insufficient because of the antigenic cross-reaction between MPXV and other orthopoxviruses [1,58].
The measures for infection control have played decisive roles in preventing personal spreading in human society. Improved protection facilities, isolation practices, and adequate education are essential to curb personal trans-mission. MPXV is not heat-resistant and can be inactivated after 30 minutes of treatment at 56℃. The virus is inactivated easily by organic solvents, such as formaldehyde, methanol, sodium dodecyl sulfonate, phenol, and chloroform [59]. MPXV is resistant to drying and low temperature and can maintain vitality for a long time at 4℃ [23].
CONCLUSIONS
Mpox was previously an endemic disease in only a few countries. Mpox infections may be an epidemic disease in certain societies with high-risk sexual behaviors. Mpox may be a new emerging STI in high-risk groups worldwide. Owing to the unique patterns of transmission and divergent manifestations in the recent outbreak, urologists must know the characteristics of the infection because patients with mpox may visit their offices with some genital lesions or other STIs. As mpox DNA can be detected in the seminal fluid of infected men, the long-term effect of MPXV in the genital organs needs to be examined. The clinical infor-mation from this paper may deepen the understanding of human mpox and curb the early transmission of the infection.
FUNDING
No funding to declare.
SUPPLEMENTARY MATERIALS
uti-18-2-35-supple.pdf
Supplementary data can be found via https://doi.org/10.14777/uti.2023.18.2.35.
Fig. 1
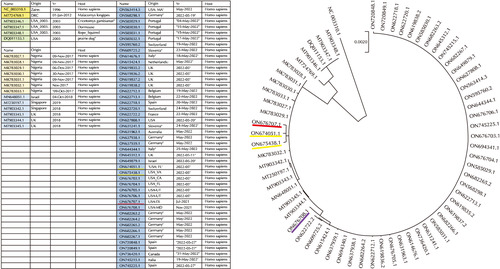
Phylogenetic analysis of 64 monkeypox (mpox) virus (MPXV) genome sequences in the National Center for Biotechnology Information (NCBI). The sequences were analyzed using mega software (version 10.16). The bootstrap consensus tree inferred from 1,000 replicates was taken to represent the evolutionary history of the taxa analyzed. The reference sequence of the Democratic Republic of the Congo (DRC) clade (A.1) from human (GenBank accession no. NC_003310.1) was reported from DRC in 1996. Some sequences were obtained from a sporadic outbreak from the USA in 2003 and genetically classified into the Republic of the Congo (ROC) clade (A.2). MT724769.1 from Malacomys longipes was reported from the DRC in 2012 and can be classified genetically into the ROC clade (A.2). The sequences from 2017 to 2022 phylogenetically form a new clade (clade B.1); seven sequences that reported from Nigeria in 2017 and six sequences in 2018 and 2019 from Israel, Singapore, and UK are tightly clustered together. The clinical information from the patients in 2018 and 2019 and their genetic information suggest that they originated in Nigeria. Three sequences (ON676701.1 from Texas in 2021, ON674051.1 from Florida in 2022, and ON675438.01 from Virginia) revealed high similarity with the earlier Nigeria strains and the MPXV sequence of ON676708 (USA_2021_MD) from a case who traveled from Nigeria to the United States in 2021 was phylogenetically placed between the sequences of strains in 2018-2019 and 2022. These findings suggest that mpox cases were already presented in the USA before the global outbreak in 2022. As all sequences in 2022 are identical, the emergence of the 2022 outbreak may be transmitted from one hidden source that potentially emerged from the continuous cryptic circulation of the same virus that caused the 2017-2018 outbreak in Nigeria. Origins and Yr (year) mean “which country” and “when” submits the sequences to the NCBI site. Host means an organism that is infected with the MPXV.

Fig. 2
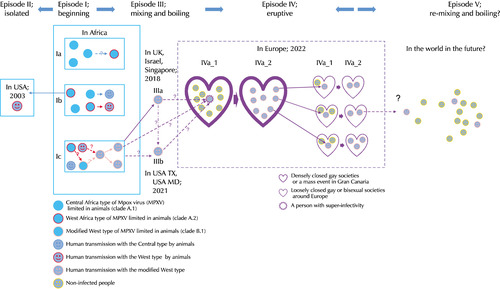
Suggested model of monkeypox (mpox) virus (MPXV) transmission. From Episode I as a beginning, the MPXV has been in a wild forest in Central Africa and infects wild animals. The zoonotic transmission routes can occur by hunting wild animals, cooking, and consuming infected meat or bushmeat. During evolutional pressure, the MPXV of the Democratic Republic of the Congo (DRC) clade (A.1) may change its genetic sequence slightly to the Republic of the Congo (ROC) clade (A.2) and clade B.1. From animal to animal, animal to human, and personal transmission may occur endemically within the African boundary. Episode II, as a limited infection, occurred in the USA in 2003. Some infected animals exported from African endemic areas transmitted the infection to humans by direct contact with blood and bodily fluids. Episode III can be defined as the mixing and pre-boiling stage. The mpox in the African countries crossed the border. New genetic sequences (clade B.1) from a Nigerian person or tourists to Nigeria were found in 2017 and 2018 around the world. Four sequences (ON676701.1 from Texas in 2021, ON674051.1 from Florida in 2022, ON675438.01 from Virginia, and ON676708 from MD revealed high similarity with the earlier Nigeria strains, suggesting that the cases of mpox were already presented in the USA before the global outbreak in 2022. Episode IV, as a boiling or eruptive stage, one super-spreader of mpox may attend densely closed gay societies or mass events in earlier 2022 and densely transmit the infection into societies. Finally, secondary person-to-person transmission occurred during sexual contacts around the world. The World Health Organization realized the seriousness of personal transmission and has declared a global health emergency against the infection. In the near future, the mpox may be endemic worldwide and progress into the re-mixing and boiling stage if we are not concerned about the infection.

Fig. 4
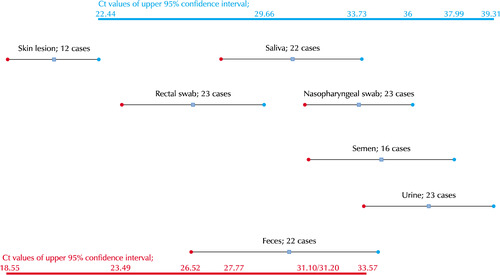
Monkeypox (mpox) virus (MPXV) load in various clinical samples. MPXV revealed various tissue tropisms. Although optimal clinical specimens for laboratory analyses depend on the disease stages or infectious routes, typical skin lesions are frequently used because skin lesions occur frequently, can be easily harvested, and have high viral loads in the lesions. In addition to skin lesions, MPXV DNA was detected in saliva or oral mucosal swab, rectal swab, nasopharyngeal swab, semen, urine, and feces. The Ct (cycle threshold) is defined as the number of cycles required for the fluorescent signal to cross the threshold or background (adapted from the article of Peiró-Mestres et al. Euro Surveill 2022;27:2200503 [48]).

- 1. Alakunle E, Moens U, Nchinda G, Okeke MI. Monkeypox virus in Nigeria: infection biology, epidemiology, and evolution. Viruses 2020;12:1257. ArticlePubMedPMC
- 2. Marennikova SS, Seluhina EM, Mal'ceva NN, Ladnyj ID. Poxviruses isolated from clinically ill and asymptomatically infected monkeys and a chimpanzee. Bull World Health Organ 1972;46:613-20.PubMedPMC
- 3. Centers for Disease Control. Prevention (CDC). Mpox in animals [Internet]. CDC; Atlanta (GA).
- 4. Yinka-Ogunleye A, Aruna O, Dalhat M, Ogoina D, McCollum A, Disu Y, et al. ; CDC Monkeypox Outbreak Team. Outbreak of human monkeypox in Nigeria in 2017;
- 5. Girometti N, Byrne R, Bracchi M, Heskin J, McOwan A, Tittle V, et al. Demographic and clinical characteristics of confirmed human monkeypox virus cases in individuals attending a sexual health centre in London, UK: an observational analysis. Lancet Infect Dis 2022;22:1321-8. ArticlePubMedPMC
- 6. Thornhill JP, Barkati S, Walmsley S, Rockstroh J, Antinori A, Harrison LB, et al. ; SHARE-net Clinical Group. Monkeypox virus infection in humans across 16 countries - April-June 2022;
- 7. Reed KD, Melski JW, Graham MB, Regnery RL, Sotir MJ, Wegner MV, et al. The detection of monkeypox in humans in the Western Hemisphere. N Engl J Med 2004;350:342-50. ArticlePubMed
- 8. Breman JG, Steniowski MV, Zanotto E, Gromyko AI, Arita I. Kalisa-Ruti. Human monkeypox, 1970-79. Bull World Health Organ 1980;58:165-82.PubMedPMC
- 9. Ogoina D, Izibewule JH, Ogunleye A, Ederiane E, Anebonam U, Neni A, et al. The 2017 human monkeypox outbreak in Nigeria-Report of outbreak experience and response in the Niger Delta University Teaching Hospital, Bayelsa State, Nigeria. PLoS One 2019;14:e0214229. ArticlePubMedPMC
- 10. Vaughan A, Aarons E, Astbury J, Balasegaram S, Beadsworth M, Beck CR, et al. Two cases of monkeypox imported to the United Kingdom, September 2018. Euro Surveill 2018;23:1800509. ArticlePubMedPMC
- 11. Erez N, Achdout H, Milrot E, Schwartz Y, Wiener-Well Y, Paran N, et al. Diagnosis of imported monkeypox, Israel, 2018. Emerg Infect Dis 2019;25:980-3. ArticlePubMedPMC
- 12. Ng OT, Lee V, Marimuthu K, Vasoo S, Chan G, Lin RTP, et al. A case of imported monkeypox in Singapore. Lancet Infect Dis 2019;19:1166. ArticlePMC
- 13. Mathieu E, Spooner F, Dattani S, Ritchie H, Roser M. Mpox (monkeypox) [Internet]. Our World in Data; Oxford.
- 14. Kumar N, Acharya A, Gendelman HE, Byrareddy SN. The 2022 outbreak and the pathobiology of the monkeypox virus. J Autoimmun 2022;131:102855. ArticlePubMedPMC
- 15. Adler H, Gould S, Hine P, Snell LB, Wong W, Houlihan CF, et al. ; NHS England High Consequence Infectious Diseases (Air-borne) Network. Lancet Infect Dis 2022;22:1153-62; Erratum. PubMedPMC
- 16. Noe S, Zange S, Seilmaier M, Antwerpen MH, Fenzl T, Schneider J, et al. Clinical and virological features of first human monkeypox cases in Germany. Infection 2023;51:265-70. ArticlePubMedPDF
- 17. Ogoina D, Yinka-Ogunleye A. Sexual history of human monkeypox patients seen at a tertiary hospital in Bayelsa, Nigeria. Int J STD AIDS 2022;33:928-32. ArticlePubMedPDF
- 18. Antinori A, Mazzotta V, Vita S, Carletti F, Tacconi D, Lapini LE, et al. ; INMI Monkeypox Group. Epidemiological, clinical and virological characteristics of four cases of monkeypox support transmission through sexual contact, Italy, May 2022;
- 19. Sah R, Abdelaal A, Reda A, Katamesh BE, Manirambona E, Abdelmonem H, et al. Monkeypox and its possible sexual transmission: where are we now with its evidence? Pathogens 2022;11:924. PubMedPMC
- 20. Kupferschmidt K. Why monkeypox is mostly hitting men who have sex with men. Science 2022;376:1364-5. ArticlePubMed
- 21. Sale TA, Melski JW, Stratman EJ. Monkeypox: an epidemiologic and clinical comparison of African and US disease. J Am Acad Dermatol 2006;55:478-81. ArticlePubMedPMC
- 22. Kaler J, Hussain A, Flores G, Kheiri S, Desrosiers D. Monkey-pox: a comprehensive review of transmission, pathogenesis, and manifestation. Cureus 2022;14:e26531. ArticlePubMedPMC
- 23. Cho CT, Wenner HA. Monkeypox virus. Bacteriol Rev 1973;37:1-18. ArticlePubMedPMCPDF
- 24. National Library of Medicine (NLM). Monkeypox virus [Internet]. NLM; Bethesda (MD).
- 25. Isidro J, Borges V, Pinto M, Sobral D, Santos JD, Nunes A, et al. Phylogenomic characterization and signs of microevolution in the 2022 multi-country outbreak of monkeypox virus. Nat Med 2022;28:1569-72; Erratum. ArticlePubMedPMCPDF
- 26. Kmiec D, Kirchhoff F. Monkeypox: a new threat? Int J Mol Sci 2022;23:7866. ArticlePubMedPMC
- 27. Bunge EM, Hoet B, Chen L, Lienert F, Weidenthaler H, Baer LR, et al. The changing epidemiology of human monkeypox-a potential threat? PLoS Negl Trop Dis 2022;16:e0010141. ArticlePubMedPMC
- 28. Blumberg S, Lloyd-Smith JO. Inference of R(0) and trans-mission heterogeneity from the size distribution of stuttering chains. PLoS Comput Biol 2013;9:e1002993. ArticlePubMedPMC
- 29. Fine PE, Jezek Z, Grab B, Dixon H. The transmission potential of monkeypox virus in human populations. Int J Epidemiol 1988;17:643-50. ArticlePubMed
- 30. Leung NHL. Transmissibility and transmission of respiratory viruses. Nat Rev Microbiol 2021;19:528-45. ArticlePubMedPMCPDF
- 31. Beer EM, Rao VB. A systematic review of the epidemiology of human monkeypox outbreaks and implications for outbreak strategy. PLoS Negl Trop Dis 2019;13:e0007791. ArticlePubMedPMC
- 32. Nolen LD, Osadebe L, Katomba J, Likofata J, Mukadi D, Monroe B, et al. Extended human-to-human transmission during a monkeypox outbreak in the democratic Republic of the Congo. Emerg Infect Dis 2016;22:1014-21; Erratum. ArticlePubMedPMC
- 33. Cann JA, Jahrling PB, Hensley LE, Wahl-Jensen V. Comparative pathology of smallpox and monkeypox in man and macaques. J Comp Pathol 2013;148:6-21. ArticlePubMedPMC
- 34. Geddes AM. The history of smallpox. Clin Dermatol 2006;24:152-7. ArticlePubMed
- 35. Petersen E, Kantele A, Koopmans M, Asogun D, Yinka-Ogun-leye A, Ihekweazu C, et al. Human monkeypox: epidemiologic and clinical characteristics, diagnosis, and prevention. Infect Dis Clin North Am 2019;33:1027-43. PubMedPMC
- 36. Jezek Z, Szczeniowski M, Paluku KM, Mutombo M. Human monkeypox: clinical features of 282 patients. J Infect Dis 1987;156:293-8. ArticlePubMed
- 37. Geretti AM, Brook G, Cameron C, Chadwick D, French N, Heyderman R, et al. British HIV Association guidelines on the use of vaccines in HIV-positive adults 2015. HIV Med 2016;17 Suppl 3:s2-81. PubMed
- 38. Petersen BW, Damon IK, Pertowski CA, Meaney-Delman D, Guarnizo JT, Beigi RH, et al. Clinical guidance for smallpox vaccine use in a postevent vaccination program. MMWR Recomm Rep 2015;64:
- 39. Centers for Disease Control. Prevention (CDC). 2023;Interim clinical considerations for use of JYNNEOS and ACAM2000 vaccines during the 2022 U.
- 40. National Library of Medicine (NLM). Mpox: how it spreads [Internet]. NLM; Bethesda (MD).
- 41. McFadden G. Poxvirus tropism. Nat Rev Microbiol 2005;3:201-13. ArticlePubMedPMCPDF
- 42. World Health Organization (WHO). Mpox (monkeypox) [Internet]. WHO; Geneva.
- 43. Oliva-Lozano JM, Alacid F, Muyor JM. López-Miñarro PA. What are the physical demands of sexual intercourse? Arch Sex Behav 2022;51:1397-417. ArticlePubMedPMCPDF
- 44. Fox CA. Recent studies in human coital physiology. Clin Endocrinol Metab 1973;2:527-43. ArticlePubMed
- 45. European Centre for Disease Prevention. Control (ECDC). Risk assessment: monkeypox multi-country outbreak [Internet]. ECDC; Stockholm.
- 46. National Library of Medicine (NLM). Mpox: signs and symptoms [Internet]. NLM; Bethesda (MD).
- 47. et al. Iñigo Martínez J. Gil Montalbán E. Jiménez Bueno S. Martín Martínez F. Nieto Juliá A. Sánchez Díaz J. Monkeypox outbreak predominantly affecting men who have sex with men, Madrid, Spain, 26 April to 16 June 2022. Euro Surveill 2022;27:2200471.PubMedPMC
- 48. Fuertes I, Vilella A, Navarro M, et al. Peiró-Mestres A. Camprubí-Ferrer D. Marcos MÁ. ; Hospital Clinic de Barcelona Monkeypox Study Group. Frequent detection of monkeypox virus DNA in saliva, semen, and other clinical samples from 12 patients, Barcelona, Spain, May to June 2022;
- 49. National Library of Medicine (NLM). Mpox: clinical recognition [Internet]. NLM; Bethesda (MD).
- 50. Jezek Z, Szczeniowski M, Paluku KM, Mutombo M, Grab B. Human monkeypox: confusion with chickenpox. Acta Trop 1988;45:297-307.PubMed
- 51. Lapa D, Carletti F, Mazzotta V, Matusali G, Pinnetti C, Meschi S, et al. ; INMI Monkeypox Study Group. Lancet Infect Dis 2022;22:1267-9. PubMedPMC
- 52. Li Y, Olson VA, Laue T, Laker MT, Damon IK. Detection of monkeypox virus with real-time PCR assays. J Clin Virol 2006;36:194-203. ArticlePubMedPMC
- 53. Hughes L, Wilkins K, Goldsmith CS, Smith S, Hudson P, Patel N, et al. A rapid Orthopoxvirus purification protocol suitable for high-containment laboratories. J Virol Methods 2017;243:68-73. ArticlePubMedPMC
- 54. Mills MG, Juergens KB, Gov JP, McCormick CJ, Sampoleo R, Kachikis A, et al. Evaluation and clinical validation of monkeypox (mpox) virus real-time PCR assays. J Clin Virol 2023;159:105373. ArticlePubMedPMC
- 55. Reynolds MG, Carroll DS, Olson VA, Hughes C, Galley J, Likos A, et al. A silent enzootic of an orthopoxvirus in Ghana, West Africa: evidence for multi-species involvement in the absence of widespread human disease. Am J Trop Med Hyg 2010;82:746-54. ArticlePubMedPMC
- 56. Orba Y, Sasaki M, Yamaguchi H, Ishii A, Thomas Y, Ogawa H, et al. Orthopoxvirus infection among wildlife in Zambia. J Gen Virol 2015;96(Pt 2):390-4. ArticlePubMed
- 57. Ropp SL, Jin Q, Knight JC, Massung RF, Esposito JJ. PCR strategy for identification and differentiation of small pox and other orthopoxviruses. J Clin Microbiol 1995;33:2069-76. ArticlePubMedPMCPDF
- 58. Macneil A, Abel J, Reynolds MG, Lash R, Fonnie R, Kanneh LD, et al. Serologic evidence of human orthopoxvirus infections in Sierra Leone. BMC Res Notes 2011;4:465. ArticlePubMedPMCPDF
- 59. Kampf G. Efficacy of heat against the vaccinia virus, variola virus and monkeypox virus. J Hosp Infect 2022;127:131-2. ArticlePubMedPMC
REFERENCES
Figure & Data
REFERENCES
Citations
Citations to this article as recorded by 

Is Human Mpox a New Sexually Transmitted Infection in Korea That Should Be Monitored?
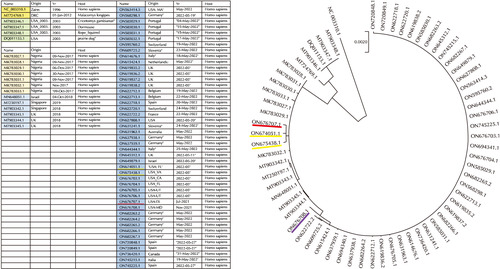
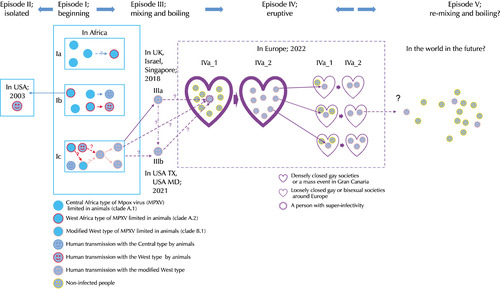
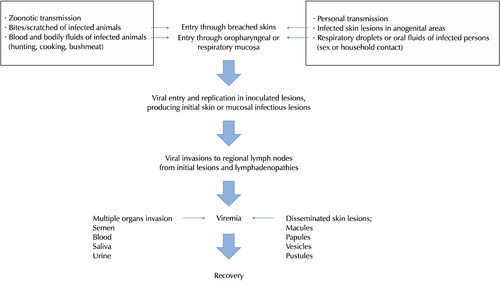
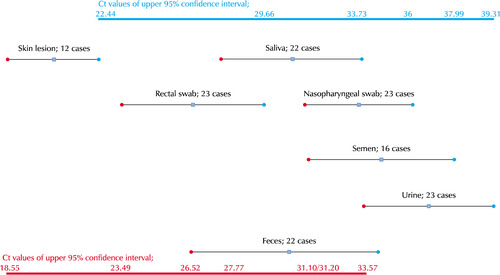
Fig. 1
Phylogenetic analysis of 64 monkeypox (mpox) virus (MPXV) genome sequences in the National Center for Biotechnology Information (NCBI). The sequences were analyzed using mega software (version 10.16). The bootstrap consensus tree inferred from 1,000 replicates was taken to represent the evolutionary history of the taxa analyzed. The reference sequence of the Democratic Republic of the Congo (DRC) clade (A.1) from human (GenBank accession no. NC_003310.1) was reported from DRC in 1996. Some sequences were obtained from a sporadic outbreak from the USA in 2003 and genetically classified into the Republic of the Congo (ROC) clade (A.2). MT724769.1 from Malacomys longipes was reported from the DRC in 2012 and can be classified genetically into the ROC clade (A.2). The sequences from 2017 to 2022 phylogenetically form a new clade (clade B.1); seven sequences that reported from Nigeria in 2017 and six sequences in 2018 and 2019 from Israel, Singapore, and UK are tightly clustered together. The clinical information from the patients in 2018 and 2019 and their genetic information suggest that they originated in Nigeria. Three sequences (ON676701.1 from Texas in 2021, ON674051.1 from Florida in 2022, and ON675438.01 from Virginia) revealed high similarity with the earlier Nigeria strains and the MPXV sequence of ON676708 (USA_2021_MD) from a case who traveled from Nigeria to the United States in 2021 was phylogenetically placed between the sequences of strains in 2018-2019 and 2022. These findings suggest that mpox cases were already presented in the USA before the global outbreak in 2022. As all sequences in 2022 are identical, the emergence of the 2022 outbreak may be transmitted from one hidden source that potentially emerged from the continuous cryptic circulation of the same virus that caused the 2017-2018 outbreak in Nigeria. Origins and Yr (year) mean “which country” and “when” submits the sequences to the NCBI site. Host means an organism that is infected with the MPXV.
Fig. 2
Suggested model of monkeypox (mpox) virus (MPXV) transmission. From Episode I as a beginning, the MPXV has been in a wild forest in Central Africa and infects wild animals. The zoonotic transmission routes can occur by hunting wild animals, cooking, and consuming infected meat or bushmeat. During evolutional pressure, the MPXV of the Democratic Republic of the Congo (DRC) clade (A.1) may change its genetic sequence slightly to the Republic of the Congo (ROC) clade (A.2) and clade B.1. From animal to animal, animal to human, and personal transmission may occur endemically within the African boundary. Episode II, as a limited infection, occurred in the USA in 2003. Some infected animals exported from African endemic areas transmitted the infection to humans by direct contact with blood and bodily fluids. Episode III can be defined as the mixing and pre-boiling stage. The mpox in the African countries crossed the border. New genetic sequences (clade B.1) from a Nigerian person or tourists to Nigeria were found in 2017 and 2018 around the world. Four sequences (ON676701.1 from Texas in 2021, ON674051.1 from Florida in 2022, ON675438.01 from Virginia, and ON676708 from MD revealed high similarity with the earlier Nigeria strains, suggesting that the cases of mpox were already presented in the USA before the global outbreak in 2022. Episode IV, as a boiling or eruptive stage, one super-spreader of mpox may attend densely closed gay societies or mass events in earlier 2022 and densely transmit the infection into societies. Finally, secondary person-to-person transmission occurred during sexual contacts around the world. The World Health Organization realized the seriousness of personal transmission and has declared a global health emergency against the infection. In the near future, the mpox may be endemic worldwide and progress into the re-mixing and boiling stage if we are not concerned about the infection.
Fig. 3
Pathogenesis of the mpox virus.
Fig. 4
Monkeypox (mpox) virus (MPXV) load in various clinical samples. MPXV revealed various tissue tropisms. Although optimal clinical specimens for laboratory analyses depend on the disease stages or infectious routes, typical skin lesions are frequently used because skin lesions occur frequently, can be easily harvested, and have high viral loads in the lesions. In addition to skin lesions, MPXV DNA was detected in saliva or oral mucosal swab, rectal swab, nasopharyngeal swab, semen, urine, and feces. The Ct (cycle threshold) is defined as the number of cycles required for the fluorescent signal to cross the threshold or background (adapted from the article of Peiró-Mestres et al. Euro Surveill 2022;27:2200503 [48]).
Fig. 1
Fig. 2
Fig. 3
Fig. 4
Is Human Mpox a New Sexually Transmitted Infection in Korea That Should Be Monitored?

 KAUTII
KAUTII
 ePub Link
ePub Link Cite
Cite