Search
- Page Path
- HOME > Search
Review Article
- Beyond Empirical Antibiotics: Toward Precision-Based Urinary Tract Infection Management and Korea-Specific Guidelines
- Sang Rak Bae, Hee Jo Yang
- Urogenit Tract Infect 2026;21(1):11-14. Published online April 30, 2026
- DOI: https://doi.org/10.14777/uti.2550048024
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader - Urinary tract infection (UTI) remains one of the most common bacterial infections, yet rising antimicrobial resistance and changing healthcare environments have challenged the traditional empiric approach to antibiotic therapy. Recent international guidelines from the European Association of Urology (EAU), Infectious Diseases Society of America (IDSA), and American Urological Association (AUA) collectively demonstrate a paradigm shift toward precision diagnostics, evidencebased antibiotic selection, standardized nonantibiotic prevention strategies, and simplified disease classification systems. The EAU has emphasized culture-based diagnosis, expanded nonantibiotic prophylaxis, and introduced a new framework distinguishing localized from systemic UTI. The IDSA has strengthened restrictions on treating asymptomatic bacteriuria, provided guidance for managing antimicrobial-resistant organisms, and simplified UTI categories. The AUA similarly highlights culture-directed diagnosis and the minimization of prophylactic antibiotics in women with recurrent UTI while formalizing nonantibiotic preventive measures. In Korea, unique resistance patterns, high extended-spectrum beta-lactamase and fluoroquinolone resistance rates, and frequent movement of patients between long-term care facilities and hospitals underscore the need for Korea-specific UTI guidelines. Although national surveillance systems such as KARMS (Korean Antimicrobial Resistance Monitoring System) and KorGLASS (Global Antimicrobial Resistance Surveillance System in Korea) provide valuable data, the evidence base remains insufficient to match the robustness of international guideline development. Establishing updated, Korean-contextualized UTI guidelines is essential for improving patient safety, optimizing antimicrobial stewardship, and effectively responding to the growing threat of resistance. The field is at a pivotal turning point, requiring proactive leadership and coordinated action within Korea’s urological and infectious disease communities.
- 152 View
- 4 Download

Original Article
- Trend Analysis of Sexually Transmitted Infection Treatments in Korea
- Soeon Park, Byung Kyu Han, Sangrak Bae, Seung-Ju Lee, Jin Bong Choi
- Urogenit Tract Infect 2024;19(2):25-30. Published online August 31, 2024
- DOI: https://doi.org/10.14777/uti.2024.19.2.25
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader ePub
ePub - Purpose: The revision of the 2023 Guidelines for the Treatment of Sexually Transmitted Infections (STIs) has been released. Hence, it is necessary to analyze the current status of STI treatments in Korea.
Materials and Methods: A questionnaire was distributed to urologists and gynecologists from December 2022 to January 2023 through an online survey program. Three hundred and forty-one urologists and 302 gynecologists responded to the questionnaire.
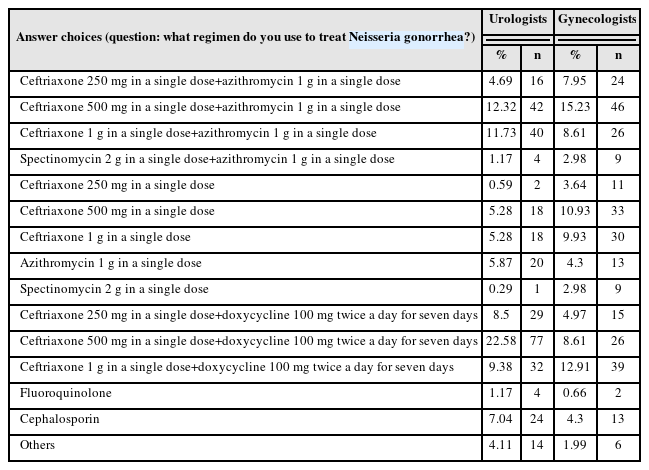
Results: For Neisseria gonorrhea treatment, ceftriaxone 500 mg and 100 mg of doxycycline twice daily for seven days were most preferred by urologists (22.58%). The treatment most preferred by gynecologists (15.23%) was 500 mg of ceftriaxone and 1 g of azithromycin in a single dose. Both urologists and gynecologists generally treat Chlamydia trachomatis according to the treatment guidelines. For treating Mycoplasma genitalium, 29.03% of urologists preferred administering azithro-mycin at 500 mg once daily, followed by 250 mg for four days. In contrast, 33.11% of gynecologists preferred doxycycline 100 mg twice daily for seven days.
Conclusions: Most urologists and gynecologists followed the treatments recommended in the 2nd edition of the STI treatment guidelines, revised in 2016. As many treatment regimens have changed because of the recent increase in antibiotic-resistant STIs, there is a need to encourage them to follow the new treatment guidelines. -
Citations
Citations to this article as recorded by- Prevalence of sexually transmitted infections among persons aged 15–24 in the Republic of Korea: A retrospective population-based descriptive study
Jinhee Seo, Minji Han, Sangrak Bae, Sooyoun Kim
Investigative and Clinical Urology.2026; 67(2): 201. CrossRef - Comparative Study of the Clinical Characteristics of Patients With Sexually Transmitted Infections Diagnosed by Nucleic Acid Amplification Tests
Jung Soo Son, Namhee Kim, Hong Sang Oh, Sang Won Park, Dong Hoon Shin
Journal of Korean Medical Science.2025;[Epub] CrossRef
- Prevalence of sexually transmitted infections among persons aged 15–24 in the Republic of Korea: A retrospective population-based descriptive study
- 7,385 View
- 39 Download
- 2 Crossref


 KAUTII
KAUTII

 First
First Prev
Prev